Technology takes the lead in reducing sepsis
According to the Centers for Disease Control and Prevention (CDC), “Anyone can get an infection, and almost any infection can lead to sepsis.”1 The report indicates that people age 65 and older; those with chronic medical conditions, such as diabetes, lung disease, cancer, and kidney disease; the immunocompromised; and children younger than one year are at higher risk of infection and sepsis.1 Staphylococcus aureus, Escherichia coli, and some types of Streptococcus are the most frequently identified pathogens causing infections that can develop into sepsis.1
Another CDC report stated that more than 1.5 million people get sepsis each year in the U.S, approximately 250,000 Americans die from sepsis each year, and one in three patients who die in a hospital have sepsis.2
Clearly, it is important for healthcare workers to be educated on the signs of sepsis so that patients can be treated as soon as it is suspected. That is not as easy as it sounds. Fever, chills, rapid breathing and heart rate, rash, confusion, and disorientation are some of the symptoms of sepsis. These symptoms are common in other conditions, too, making it difficult to diagnose sepsis.
Calvin K. Janney RN, MSN-L, Ascom Clinical Application Specialist, noted, “Sepsis is a complicated and challenging condition to diagnose. Both patients and healthcare providers often don’t recognize the early symptoms, which can mimic common ailments such as the flu, and therefore do not fully recognize or understand that the real problem is sepsis. Most cases of sepsis occur in the intensive care unit (ICU), where the patient population is older, has weakened immune systems, often has drug resistance to certain types of bacteria, and has multiple invasive lines or tubes. These conditions can lead to the types of infection most likely to lead to sepsis.”
Bart Abban, Data Scientist, VigiLanz, added, “Because of its complexity, it has historically been difficult to find consensus in the definition, diagnosis, and treatment of sepsis among the medical community. A major reason for the lack of awareness is that sepsis is often secondary to other diseases and conditions. Although sepsis might be what delivers the coup de grace to a patient, the initial hospitalization is often for another illness or condition.”
Along the same vein, Rose Mary Casados, MBA, BSMT, ASCP, WW Marketing Manager, BD Life Sciences, said, “Sepsis is a secondary condition, usually the final common pathway to death. The challenges lie in driving education beyond first-line infections—such as pneumonia, urinary tract infection, and wound infection—but rather to the outcome of these diseases, which could include sepsis.”
Sepsis is a puzzle to healthcare workers, so it is no surprise that the public knows little about it. The flu epidemic of 2017-2018 has drawn more attention to sepsis, according to Phillip Chan, MD, PhD, Chief Executive Officer, CytoSorbents Corporation. “The most recent influenza epidemic and the daily highly publicized stories of otherwise healthy individuals dying rapidly of the flu and associated complications due to ‘cytokine storm’ and excessive inflammation has likely improved awareness of sepsis.”
Communication is key
When sepsis is suspected, minutes count; so, quick and easy communication is critical among those involved in the patient’s care. Janney, Ascom, noted, “Most hospitals have sepsis protocols they initiate when a patient is suspected of being septic. Improved communication opportunities arise when a nurse or healthcare professional can receive alerts and send messages regarding diagnostic tests results. Because sepsis can progress rapidly, early detection and treatment improves outcomes.”
The Ascom Healthcare Platform software captures, tracks, and records vital signs, alarms, and other data from patient-room equipment, ICUs, operating rooms, and other wards. Information is continuously analyzed and presented as meaningful data in a controlled, secure manner to the right person or system at the right time and at the right place, resulting in faster responses to individual patient events.
“Because time is of the essence when treating sepsis,” said Janney, “Ascom’s Clinical Consulting Service and portfolio of products, such as the Ascom Myco smart phone with the Unite Context clinical collaboration application, allow hospital staff members to communicate and collaborate at a time when speed is critical.”
Rhonda Collins, Chief Nursing Officer, Vocera Communications, agreed, saying, “Time is of the essence when diagnosing and treating sepsis. Real-time communication between clinicians is critical. To help care teams identify sepsis sooner and initiate
treatment quicker, Vocera technology can integrate with a hospital’s electronic health records system and predictive analytics tool.”
Collins provided an example of how their product works to thwart sepsis. “At Halifax Health in Florida, Vocera teamed up with Wolters Kluwer Health to arm care teams with a high-powered sepsis surveillance and alerting solution. Wolters Kluwer’s POC Advisor analyzes 250+ data points within a patient’s medical record to identify early signs of sepsis, warn caregivers of escalating risks, and empower them with evidence-based guidance at the point of care. When early signs of an infection are detected, an alert with situational information is sent directly to the patient’s care-team members via their Vocera badges and smartphone apps. This clinical workflow and proactive communication can result in faster diagnoses and treatment of sepsis, which leads to reduced severity, decreased mortality, and lower costs.”
Steve Claypool, MD, Medical Director for Wolters Kluwer Clinical Software Solutions, concurred. “POC Advisor can detect and alert the clinical staff to sepsis cases faster and provide guidance on the right course of treatment. It does that accurately, early, and effectively.”
“Identification and communication are key to expediting diagnosis of sepsis,” declared Tim O’Malley, President, EarlySense Inc. “For every hour a patient is septic, their mortality rate will increase by almost 8 percent; therefore, any infection needs to be determined earlier and treatment initiated. As time goes by, acuity of these patients increases. Left undiagnosed and untreated, these patients will become more complex, requiring more time in a higher acuity environment.”
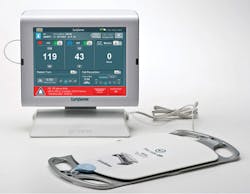
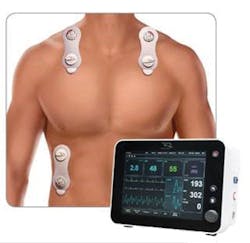
O’Malley explained that the EarlySense System is a contact-free, continuous monitoring system employing a small sensor under the patient’s mattress that collects the heart rate and respiratory rate twice per second. “The goal of the EarlySense System is to identify the earliest warning signs, so providers can expedite action, diagnosis, and treatment. One of the first signs of infection, and concurrently sepsis, is an increase in these key vital signs,” said O’Malley. “This system helps alert clinicians that a patient is experiencing an increase in heart rate and respiratory rate and should be evaluated. We introduced a multi-parameter alert recently that warns caregivers if heart rate combined with respiratory rate is elevated over a period of time. If both of these parameters are elevated for, say, 4 hours, it merits a check of other parameters to determine if the patient is developing a more advanced infection or is pre-septic.”
In a study of more than 7,000 patient outcomes, using the EarlySense System, the number of ICU days for transferred patients decreased by 46 percent, the overall hospital length of stay decreased by 9 percent in the intervention group, and the number of code-blue events decreased by 86 percent, all because patients were treated as soon as they began to deteriorate.3
Chan, CytoSorbents, highlighted the importance of all healthcare professionals being alert to sepsis, “particularly when patients have signs and symptoms of infection, exhibit fever, or have instability, especially concerning blood pressure, oxygenation, or kidney function. CytoSorbents’ CytoSorb blood-purification technology is designed to control the deadly inflammation that kills patients in severe sepsis and septic shock, helping to round out the spectrum of treatment approaches for sepsis that include rapid detection, antibiotics, supportive-care therapy, and active control of inflammation.”
Blood cultures are an important component in diagnosing sepsis. “A key component is promoting best practices in blood culturing and offering proven performance in the diagnosis of sepsis,” stated Casados. “BD’s integrated blood-culture solution includes the BD BACTEC blood-culture media, BD BACTEC FX Series Automated Blood Culture Instrument, and the BD Synapsys informatics solution. BD recognizes the key role of data-management solutions in measuring quality metrics and workflow efficiencies. BD Synapsys Microbiology Informatics Solution connects data from BD blood-culture instruments in disparate systems and settings, which expedites communication to clinicians and pharmacists, facilitating accurate, timely diagnosis and appropriate therapy for patients.”
BD BACTEC blood culture media
Connecting the dots between sepsis and readmissions
The Centers for Medicare and Medicaid are required to reduce payments to certain hospitals that have excessive readmissions within 30 days of the patient’s dismissal,4 so it is vital that sepsis patients are stable before leaving the hospital. Abban, VigiLanz, cited some readmission statistics. “More than 12 percent of all unplanned 30-day readmissions are associated with a sepsis diagnosis during the previous admission and patients who are readmitted with an infection within 30 days of discharge are at risk of sepsis.”
Abban described how the VigiLanz platform’s tools can lead to prevention and reduction of HAIs, sepsis, and readmissions. “The Infection Control Module services, including cluster detection, provide early detection of hospital outbreaks that lead to HAIs; HAI identification provides the data analytics needed to help understand population risk factors and opportunities for improvement; a prevention tool box helps in preventing infections; and drug-bug mismatch rules automate the process of identifying patients who are on ineffective anti-infective drugs. Sepsis Discrete Service provides highly-sophisticated customizable rules to detect cases of sepsis that are present on admission and monitors to ensure protocols are followed. The Sepsis Predictive Machine Learning Algorithms predict the risk of sepsis for inpatients.”
Claypool, Wolters Kluwer, observed, “Sepsis is the most common condition resulting in readmission.” He explained that electronic surveillance could help by catching the condition early, when it is most treatable, so the patient’s condition doesn’t escalate, and the patient isn’t discharged while their health is still compromised.
“Wolters Kluwer’s POC Advisor aggregates, normalizes, and analyzes patient data from disparate clinical systems to drive early, accurate sepsis detection and treatment,” said Claypool. “Hundreds of rules are built into the platform to account for possible comorbidities and medication abnormalities. This enables prescriptive alerts that have scientifically demonstrated unprecedented levels of sensitivity and specificity,5 alerting clinicians to at-risk patients without alert fatigue.” According to Claypool, POC Advisor reduces sepsis mortality by half, reduces related 30-day readmissions by 30 percent, and lowers lengths of stay.
Chan, CytoSorbents, noted, “Sepsis is a two-part equation consisting of a serious infectious trigger followed by an overzealous immune response that can lead to uncontrolled inflammation, organ failure, and death. “If these patients survive, they are often severely debilitated and often wind up back in the ICU or dead in the first year after hospital discharge.”
Chan described how CytoSorb works to combat deadly inflammation in septic patients. “CytoSorb is an extracorporeal cytokine adsorber that reduces cytokines and cytokine storm, as well as many bacterial toxins and other mediators that contribute to uncontrolled systemic inflammation. In doing so, CytoSorb has helped to stabilize and turn patients around, reducing organ injury, and restoring adequate blood pressure during septic shock.”
CytoSorb is compatible with existing dialysis, renal replacement, and extracorporeal membrane oxygenation machines found in hospital ICUs today. It is approved in the European Union but not yet in the U.S.
“By reducing the severity of illness,” added Chan, “CytoSorb helps to reduce the debilitating effects of sepsis, helps patients get out of the ICU faster, controls costs, and potentially reduces the incidence of readmissions later.”
Bob Gerberich, CCO, Magnolia Medical Technologies, talked about the importance of accuracy in blood cultures when diagnosing sepsis: “Blood-culture contamination introduces substantial uncertainty about accurate diagnosis, as well as a lack of clarity for patients and their families. Forty percent of positive results are actually false positives due to blood-culture contamination.
“Steripath is a patented closed system that mechanically diverts and sequesters the initial 1.5 to 2.0 mL of blood, which is known to contain contaminants, into an isolation chamber. Once diversion is complete, an independent second sterile blood-flow pathway mechanically opens, allowing only pure, contaminant-free venous blood to flow into the culture bottle.”
“Using standard techniques of the past, hospitals have strived to meet the blood-culture contamination national benchmark of 3 percent. By comparison,” Gerberich said, “Steripath is clinically proven to virtually eliminate blood-culture contamination.” This is important, because an accurate diagnosis of sepsis helps differentiate between patients who need treatment and those who do not, meaning unnecessary use of antibiotics can be avoided.
Gerberich referred to recently published results from a prospective, controlled trial of Steripath, versus standard phlebotomy procedures, in the emergency department at the University of Nebraska Medical Center (UNMC), which showed a 92 percent reduction in false positives with a 12-month sustained contamination rate of 0.2 percent when using Steripath.6 “Results from the UNMC study of Steripath conservatively estimated $4,850 as the cost of a blood-contamination event resulting in a false-positive test result for sepsis,”6 said Gerberich. “Using this conservative estimate, infection control expert and study author Mark Rupp, MD, said the use of Steripath would save his single hospital $1.8 million per year by preventing 373 cases of contamination leading to false positives.”6
Casados, BD Life Sciences, stressed the importance of understanding the link between HAIs, antimicrobial therapy, readmissions, and sepsis. “HAIs can lead to many complications during hospital admission,” she said. Casados offered an example: immunocompromised patients initially admitted with pneumonia or for surgery, etc., may be placed on antimicrobial therapy for a prolonged period of time, increasing the chance of building resistance to the antibiotic, which increases the chance of contracting an HAI, which, in turn puts the patient at risk of acquiring sepsis.
Shane Cooke, Chief Strategy Officer, Cheetah Medical, referred to a study published in JAMA indicating that the proportion and cost of readmissions due to sepsis are even higher than those more widely known conditions.” In the U.S., one patient every 20 seconds is diagnosed with sepsis, and 28 percent to 50 percent of these patients die.”7
“Achieving the proper fluid balance during sepsis is critical to avoiding complications and even death,” said Cooke, noting that balance between too little and too much fluid for sepsis patients may sometimes be delicate. “More than 80 percent of patients within a hospital are receiving fluids intravenously, especially in emergency situations such as with low blood pressure. Unlike prescription medicines, however, infusion fluids are often prescribed without measuring a patient’s ability to absorb or respond to them. Receiving too little fluid intravenously, or too much for a patient’s specific needs, can lead to serious complications, even death.
“Studies have shown Cheetah Medical’s non-invasive technology equips clinicians with the information needed to guide fluid-management decisions accurately, which may lead to improved clinical and economic outcomes,” stated Cooke. He alluded to sepsis studies from the University of Kansas Health System demonstrating that stroke volume optimization, “guided by Cheetah technology, led to a reduction in ICU length of stay of 2.9 days and reduced the risk of both mechanical ventilation and initiation of acute dialysis.8 Additionally, the data show total hospital cost savings of over $1.4 million during the six-month study.”8
The staggering cost of sepsis
O’Malley, EarlySense, brought out an astounding fact. “The financial burden of sepsis is incredibly costly. In 2015, Medicare paid $6 billion to treat sepsis.”9, 10
“Sepsis carries an estimated annual financial burden of nearly $24 billion, with the average hospital bearing costs of nearly $19,000 per case for a primary diagnosis,” contributed Claypool, Wolters Kluwer. “Yet, the Advisory Board notes that the typical Medicare reimbursement for sepsis and sepsis with complications is just $7,100 to $12,000. POC Advisor helps to lower those costs by reducing lengths of stay, as well as sepsis-related 30-day readmissions.”
“Globally, sepsis is one of the leading causes of mortality and critical illness, contributing to 25 percent to 30 percent of hospital mortality rates,”11 said Casados, BD Life Sciences. “Clinical studies have demonstrated a two-fold increase in mortality caused by sepsis when inappropriate antimicrobial therapy is given.12 Sepsis is the No. 1 cost of hospitalization in the U.S., consuming more than $24 billion each year.13
Collins, Vocera Communications, talked about a 2016 study,14 which revealed “the annual costs for treating sepsis in hospitals increased over $3.4 billion during a two-year period. While sepsis can have a significant impact on a hospital’s bottom line, the impact it can have on the lives of patients and families is staggering. Every year, sepsis kills approximately 258,000 people in the U.S., or one person every two minutes. For every hour that passes without treating sepsis, the likelihood of death increases. The best way to beat sepsis is by beating the clock. Time is a key factor in the battle against sepsis. So, an integrated clinical workflow with mobile communication, intelligent alerting, and real-time situational awareness is essential for reducing sepsis-related complications and costs.”
References
- Centers for Disease Control and Prevention. Get ahead of sepsis. Last accessed March 1, 2018.
- Centers for Disease Control and Prevention. Sepsis data & reports. https://www.cdc.gov/sepsis/datareports/index.html. Last accessed March 1, 2018.
- Brown, H, Terrence J, Vasquez P, et al. Continuous monitoring in an inpatient medical-surgical unit: a controlled clinical trial. Am J Med. 2014 March;127:226-232.
- Centers for Medicare and Medicaid Services. Readmissions Reduction Program (HRRP). https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/AcuteInpatientPPS/Readmissions-Reduction-Program.html. Last accessed March 1, 2018.
- Manaktala S, Claypool SR. Evaluating the impact of a computerized surveillance algorithm and decision support system on sepsis mortality. J Am Med Inform Assoc. 2017 Jan;24(1):88-95.
- Rupp ME, Cavalieri RJ, Marolf C, et al. Reduction in blood culture contamination through use of initial specimen diversion device. Clin Infect Dis. 2017 Jul 15;65(2):201-205.
- Mayr FB, Talia VB, Balakumar V, et al. Proportion and cost of unplanned 30-day readmissions after sepsis compared with other medical conditions. JAMA. 2017;317(5):530-531. https://jamanetwork.com/journals/jama/fullarticle/2598785.
- Latham HE, Bengtson CD, Satterwhite L, et al. Stroke volume guided resuscitation in severe sepsis and septic shock improves outcomes. J Crit Care. 2017;42(12):42-46. http://www.jccjournal.org/article/S0883-9441(16)30938-8/fulltext.
- Castellucci M. Sepsis costs Medicare $6 billion in 2015, more than any other discharge. Modern Healthcare. September 1, 2017. http://www.modernhealthcare.com/article/20170901/NEWS/170909982. Last accessed March 2, 2018.
- Center for Medicare and Medicaid Services. Inpatient charge data FY 2015. https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/Medicare-Provider-Charge-Data/Inpatient2015.html. Last accessed March 2, 2018.
- Fleischmann C, Scherag A, Adhikari NK, et al. Assessment of global incidence and mortality of hospital-treated sepsis. Am J Respir Crit Care Med. 2016;193(3):259-272.
- LaRosa SP. Sepsis. Cleveland Clinic Center for Continuing Education, Cleveland Clinic Foundation: Lyndhurst, OH; August 2010. https://www.hpnonline.com/wp-content/uploads/2018/03/HPN_LaRosa_Ref.pdf Last accessed March 8, 2018.
- Torio CM, Moore BJ. Agency for Healthcare Research and Quality. Healthcare Cost and Utilization Project. Statistical Brief #204. National inpatient hospital costs: the most expensive conditions by payer, 2013. May 2016. http://www.hcup-us.ahrq.gov/reports/statbriefs/sb204-Most-Expensive-Hospital-Conditions.pdf.
- Sepsis Alliance. New U.S. government report reveals annual cost of hospital treatment of sepsis has grown by $3.4 billion. Sepsis Alliance News. June 30, 2016. https://www.sepsis.org/sepsis-alliance-news/new-u-s-government-report-reveals-annual-cost-of-hospital-treatment-of-sepsis-has-grown-by-3-4-billion/.
About the Author

Susan Cantrell
Susan Cantrell is Infection Prevention Editor for Healthcare Purchasing News.