One of the biggest concerns of infection-prevention professionals is the amount of time their heads are buried in data rather than focused on patient and staff needs. Reporting requirements from regulatory agencies such as Centers for Medicare and Medicaid Services demand that infection preventionists (IPs) use their time to gather, analyze, and report data in multiple formats to their hospital and other places such as the National Healthcare Safety Network (NHSN). Whether the hospital gets paid for a service may depend on this data, for instance, so it really is important. Some sources estimate that nearly one-half of IPs’ time is spent on surveillance. This ever-growing demand for data places more responsibilities on IPs, but it is an important component in the battle against infection, because from this data are derived strategies to reduce infection.
This is where technology is a valuable tool. Manual data entry is tedious, time-consuming, and vulnerable to human error. People can get tired, distracted, frustrated, and stressed. Electronic technology, not so much. It doesn’t grow weary or feel pressured or get confused, and it does not miscalculate. It can provide more accurate results and do it much faster. Meanwhile, the IP can get out from behind the desk and onto the floors, the intensive-care units, and the operating rooms, to observe and consult as an active team member. They have more time to go on rounds, lead safety drills, educate staff, and design other activities to protect staff and patients.
Scoping out the territory
The options in data-mining systems have grown with the demand for more usable data. What may have started out as electronic surveillance of HAIs has grown to encompass so much more. Healthcare Purchasing News talked to some of the vendors of data-mining systems who explained their capabilities.
Brian Foy, Chief Product Officer, Q-Centrix, described how their solution is set up. “The Q-Centrix infection-screenings solution evaluates a healthcare facility’s data for process-improvement opportunities related to infection prevention. A unique aspect is its holistic approach: in addition to a technology solution, Q-Centrix partner-facilities are supported by a highly skilled team of certified IPs that are part of the solution. These individuals typically have 10 years of infection-prevention experience, and seventy-five percent are certified in infection control.
“The solution’s process involves validating and reporting positive infection-screening cultures using the NHSN Patient Safety Component Protocols,” continued Foy. “In reviewing the cultures, the Q-Centrix IPs can assist in offering recommendations related to infection prevention, including approaches that have helped other facilities, approaches that the Q-Centrix partner-facility’s team may not otherwise be aware of.”
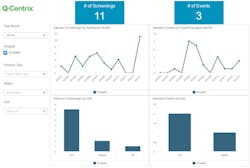
Foy explained how data is managed through Q-Centrix’s technology platform, Q-Apps. “Embedded in Q-Apps is an NHSN algorithm. The Q-Centrix IPs enter a facility’s data into the system, and the automated NHSN algorithm guides the IPs in determining an NHSN event. The process ensures NHSN events are accurately documented and reported by deadline, and it produces a report for the facility to review. It also alleviates the facility’s IPs of time-intensive surveillance and reporting tasks, and diminishes disruption from any IP turnover at the facility.”
Q-Centrix’s approach has yielded significant recouped time and costs for partner facilities. Foy cited the example of Baptist Hospital, a 492-bed acute-care facility in Pensacola, FL, which experienced favorable results in partnering with Q-Centrix over the course of the year 2017. (1) There were twenty-plus hours per month recouped from data-management–related tasks, (2) a forty-five percent reduction in catheter-associated urinary-tract–infection incidents, (3) a seventy-three percent reduction in central-line–associated bloodstream-infection incidents, and (4) $1.2 million savings in penalties and costs.
Foy noted, “While data on the Q-Centrix infection-prevention screening has not been reported in a scientific journal, we developed a case study on Baptist Hospital that further explains the approach and results for that particular case.” Readers also might be interested in Foy’s two-part guest blog about evaluating infection-prevention–screening needs published to the HPN online blog in July 2018. (Getting serious about infection prevention:Tips for evaluating your infection prevention screening needs Part Two)
BD offers the MedMined Surveillance Advisor. Chad Glover, Vice President and General Manager, MedMined at BD, explained that MedMined Surveillance Advisor “collects and standardizes clinical data from healthcare systems to ensure comparability across all facilities, and utilizes patented analytics to transform data into actionable information. MedMined evaluates billions of permutations of data to identify statistically significant and clinically relevant changes in pathogen occurrence and resistance trends. These services assist clinicians in the identification, prevention, and drug-therapy management of community- and hospital-onset organisms including HAIs and multidrug-resistant organisms.”
Glover highlighted how MedMined assists IPs in the battle against antimicrobial resistance. “MedMined provides computer-assisted decision-support technology to aid in the evaluation of the appropriateness of antibiotics, to measure antimicrobial usage, and to track and trend resistance. Through timely notifications, clinicians can optimize antimicrobial prescribing to improve outcomes and reduce unnecessary antibiotic use.
“When combined with our clinical customer service, BD MedMined Surveillance Advisor helps hospitals improve clinical and financial outcomes,” stated Glover. He provided an example. “DCH Health System’s partnership with BD MedMined led to an enterprise-wide reduction in infection rates. During a three-year system-wide analysis, DCH utilized the MedMined solution to protect 418 patients and to avoid 3,584 patient-days, totaling $3,224,562 in potential cost avoidance.”
Steve Meurer, PhD, MBA, MHS, Executive Principal, Data Science and Member Insights, Vizient, described their solution and how its capabilities produce findings that boost best practices. “Vizient’s Clinical Data Base (CDB) is uniquely designed to provide hospitals with insights into finance, operations, quality, and safety. Hospitals are able to populate leadership dashboard metrics and targets, and to set up transparent, custom benchmarking groups; then, users can drill substantially into those metrics to identify areas for improvement.”
Meurer noted the CDB “also produces a number of template reports and dashboards that can be used to motivate change. “For example,” continued Meurer, “CDB data may show a twenty-five percent higher risk-adjusted mortality than a comparable group of forty hospitals that they picked by name. The CDB enables users to become ‘investigators’ and drill into the data to understand where and why they are different. The data may show they have a lower use of palliative care than those in their compare group. They may find their length of stay before getting patients to hospice care is five days longer than all of the forty hospitals. They may decide to create in-hospital hospice beds that could result in lower length of stay and mortality, reduce in-hospital complications, and lower costs.” Meurer highlighted another virtue of CDB. “Because CDB data is transparent, users can connect with each other to answer questions and share best practices.”
Meurer noted, “Vizient’s CDB has been cited in hundreds of articles over the last five years in many journals, including the Journal of the American Medical Association.” He cited a couple of examples where CDB was used to good effect. In the first example, CDB revealed that, among hospital discharges at U.S. academic medical-center–affiliated hospitals, blacks exhibited lower adjusted rates of sepsis hospitalizations and mortality than whites.2 The second example centered on skin and soft-tissue infections (SSTI), revealing a decline in SSTI incidence in U.S. emergency departments between 2009 and 2014, a significant shift from the increase in SSTIs after 2000.3
Daisy Jackson, BSEH, CIC, Manager, Member Engagement — Clinical Surveillance Solutions, Premier Inc., succinctly described how their solution works to improve IPs’ work. “The TheraDoc solution provides real-time data that has been standardized across various data sources to alert clinicians of potential risks and supports the necessary interventions to improve outcomes, lower costs, and meet compliance.”
“TheraDoc’s capabilities have a history of success with over 1,100 facilities across the United States,” Jackson noted. She offered the example of three hospitals and 1,100 beds, all within the Detroit Medical Center: Detroit Receiving Hospital, Harper University Hospital, and Sinai-Grace Hospital. Jackson summarized the study’s findings.1 “TheraDoc’s active alerting, coupled with stewardship intervention in patients with Gram-negative bacteremia, demonstrated a positive impact on time to appropriate therapy, length of stay, and mortality. After controlling for differences between groups, being in the intervention arm was associated with a decrease in length of stay of 2.2 days.”
Good advice for purchasers from the experts
What advice do these vendors have for purchasers of data-mining systems? Well, they have plenty to say. Foy, Q-Centrix, suggested, “One of the biggest challenges for a facility’s IP team is effectively balancing time on the floor with time needed to review data for potentially positive cultures. Consider solutions that provide expert support and the right amount of technology to help give time back to a facility’s team, enabling its IPs to focus on their other responsibilities, such as rounding at their respective nursing units or affiliated clinics, providing education, observing aseptic techniques during device-insertion procedures and/or surgery, and performing construction rounds to mitigate physical-environment infection risks.”
Glover, BD, advised, “When choosing a surveillance system, it is important to first articulate your organization’s goals of deploying and maximizing the technology. Next, you need to understand how the vendor’s product and clinical support align with your goals, facilitate effective use and optimization, and enable desired outcomes. To maintain confidence in the data and analytics, it is imperative to understand if you or the vendor is responsible for standardizing the data over time. When selecting a partner, ensure they are equipped to meet the ever-changing needs of the industry through their technology and support models, and offer universal data standardization for accurate comparisons, benchmarks, and best practices.”
Jackson, Premier, offered, “There are so many factors to keep in mind when selecting a system. This makes prioritization incredibly important. Mobility, ability for your clinical teams to customize, and workflow aligned to your clinical team should be high on the list. In short, your solution should have clinical and technology expertise that can support your evolving clinical and organizational initiatives. Systems are expected to streamline compliance and help clinical teams operate at the top of their license.”
Meurer, Vizient, added, “The two most important attributes of a data-mining system is transparency and substantial drill-down capabilities. Without those attributes, it is difficult to network with other hospitals, which is a proven path to speed process improvement.”
References
- Pogue JM, Mynatt RP, Marchaim D, et al. Automated alerts coupled with antimicrobial stewardship intervention lead to decrease in length of stay in patients with Gram-negative bacteremia. Infect Control Hosp Epidemiol. 2014;35(2);132-132. Last accessed January 1, 2019.
- Chaudhary NS, Donnelly JP, Wang HE. Racial differences in sepsis mortality at U.S. academic medical center-affiliated hospitals. Crit Care Med. 2018 Jun;46(6):878-883.
- Morgan E, Hohmann S, Ridgeway J, et al. Decreasing incidence of skin and soft tissue infections at 86 U.S. emergency departments, 2009-2014. Clin Infect Dis. 2018 Jun 15. [Epub ahead of print]. Last accessed January 1, 2019.
About the Author

Susan Cantrell
Susan Cantrell is Infection Prevention Editor for Healthcare Purchasing News.