Preventing infection from surface to stratosphere
Success in infection prevention and control has so many facets it is truly mindboggling. There is a constant search for innovative products that can help to keep the environment cleaner, make diagnosis faster, make data more accessible, keep patients safer, and help caregivers to be more efficient.
Centers for Disease Control and Prevention say, “On any given day, about one in 31 hospital patients has at least one healthcare-associated infection [HAI].”1 There is a slight reduction in some HAIs in the past few years, but it is measured in single-digit percentages, so clearly there is a great deal of room for improvement.2
Advances in technology play an important role in improving health care. Healthcare Purchasing News talked to some of the vendors in the industry who are on the cutting edge of innovative medical products and services centered on infection prevention and diagnosis. We will start with products beginning at the ground and end by ascending to the cloud.
Footwear sanitizing station
Tip: Infection prevention should begin from the ground up.
Have you ever stopped to think how much dirt, debris, and germs are tracked in and out of a medical facility in a day? Depending on the size of the facility, hundreds if not thousands of employees, patients, and visitors cross the facility’s thresholds. PathO3Gen Solutions has a product devised to prevent infection from gaining a foothold at medical-facility doors.
Sunil Pandya, MD, MBA, Chief Clinical Officer, PathO3Gen Solutions, explained their mission. “At PathO3Gen Solutions, we imagine a world where the number of deaths due to preventable, life-threatening infections are significantly reduced with the use of our materials, products, responsible technology, and expertise in helping clients solve problems.”
PathO3Gen Solutions’ UVC + Ozone Footwear Sanitizing Station eliminates deadly pathogens—such as methicillin-resistant Staphylococcus aureus (MRSA), Candida species, and Clostridium difficile (C. diff)—from the bottom of footwear. Virtually no change in routine is required. Step on the station, wait for about six to eight seconds, and done.
The proof of a product’s efficacy is in the statistics. Pandya related the experience of an acute-care hospital in Florida undergoing construction, an environment that presents added opportunities for contaminants to travel. Nine of their Footwear Sanitizing Stations were installed. The results are that they “saw a 34 percent reduction in infections from February 2019 through July 2019,” said Pandya. “We also did an employee satisfaction survey that resulted in a 92 percent overall satisfaction rate. Nurses feel comfortable taking their shoes home after stepping on the stations, and the public feels safer for their loved ones in the hospital.”
Pandya also cited an independent study of a local hospital performed in 2017 by My Lien Dao, PhD, Associate Professor at the University of South Florida. At the time, the product was named SoleMate Sanitizing Device but has since rebranded to PathO3Gen Solutions Footwear Sanitizing Station. “The results showed a 99.59-percent reduction in MRSA and a 97.5-percent reduction in C. diff after stepping on the unit for eight seconds,” related Pandya.3
In August 2019, a study conducted by NSF Labs International showed kill rates at four, six, eight, and ten seconds of UVC and ozone exposure. The log-reduction results at ten seconds are as follows: Candida auris, 5.16; Escherichia coli (ESBL), 4.96; Klebsiella pneumoniae (CRE), 4.86; Pseudomonas aeruginosa (MDRO), 4.53; MRSA, 4.51; C. diff, 4.40; Enterococcus faecalis (VRE), 3.86.
Disinfectant surface cleaner
Tip: Select the appropriate product to eliminate the toughest pathogens from touch surfaces.
Our next stop will take us from the ground to the mid-level environment. It is a given that the patient environment should be kept squeaky clean for everyone, patient and staff alike. It is particularly important for patients who are very young, very old, or immunocompromised at any age. Acquisition of a hospital-acquired infection (HAI) presents even more danger for those individuals.
Ferris described Clorox Healthcare Fuzion Cleaner Disinfectant as a next-generation bleach product with the ability to kill C. diff spores in two minutes and specifically designed for expansive daily use. “With its low odor profile, little-to-no residue after use, and wide-range surface compatibility, Fuzion can be used throughout hospitals for more comprehensive disinfection,” averred Ferris.
Clorox Healthcare Fuzion Cleaner Disinfectant is used to reduce C. diff at Fairfield Medical Center (FMC), a not-for-profit community healthcare facility serving more than 250,000 residents in southeastern Ohio. FMC uses the product in all inpatient and outpatient areas, on all furniture, and in all public spaces such as waiting rooms, public restrooms, and common areas. It is important to cover these areas in addition to patient rooms, because, as Ferris pointed out, “Patients with C. diff and other infectious diseases may visit many different areas in the hospital such as the emergency room, waiting rooms, labs, etc., making a product like Fuzion valuable due to its ability to adequately address more severe infection risks in both clinical and public areas of hospitals.”
Ferris continued, “FMC launched a facility-wide infection-prevention campaign, beginning in 2016, that combined innovative techniques, including daily hospital-wide cleaning with Clorox Healthcare Fuzion Cleaner Disinfectant, to decrease its healthcare-associated C. diff incident rate. Through its elevated infection-prevention protocols, including the daily use of Fuzion, FMC achieved an 88-percent reduction in its healthcare-associated C. diff incident rate and maintained a 0.68-percent incident rate from January to July 2018, creating a significantly safer environment for patients, staff, and visitors, as well as far exceeding expectations, given the initial goal was to reduce C. diff infection rates by 50 percent.”4
Room disinfection
Tip: Approach disinfection holistically.
Room disinfectors have only been employed in recent history, but an appreciation of their value increased quickly. The value is in their ability to treat the whole environment, nooks and crannies where wipes, cloths, mops, and disinfectants may not be able to reach, making for a safer environment for patients, visitors, and staff.
Ed Striefsky, Vice President, Sales and Operations, related the experience of how Bioquell helped to improve the rate of infection, creating a safer environment for patients as well as enhancing best practices, at North Mississippi Medical Center (NMMC) in Tupelo. “C. diff rates were on the rise in 2010 and 2011. In 2012, they decided to implement Bioquell’s Proactive service, which includes having Bioquell technicians on-site full-time to run decontamination cycles, as needed, using Bioquell equipment. Doing this allowed the NMMC infection control and environmental-services teams to coordinate with Bioquell team members to formulate the best course of action for their specific needs to reduce HAIs, in particular, C. diff. Rooms vacated by patients with C. diff were either decontaminated immediately with Bioquell technology or held until the technology was available to decontaminate the room.
In 2010, the C. diff infection rate per 1,000 patient-days at NMMC was 0.8, then it rose to 1.2 in 2011. “Bioquell’s hydrogen-peroxide–vapor technology was implemented with the Bioquell Proactive in 2012,” said Striefsky. “In 2012, the C. diff infection rate dropped to 0.4 and maintained about the same in 2013. A total of 3,060 rooms were decontaminated during this two-year span with Bioquell technology.”5
Rapid diagnostic tools
Tip: Rapid diagnostics help to save lives and limit antibiotic resistance
Rapid diagnostic tools can play a critical role in patient health and survival. If, for example, a patient has sepsis, time is of the essence. A delayed diagnosis can cost a life. T2 Biosystems has a rapid diagnostic test that can cut down diagnosis from days to hours.
The products are two of several panels that are approved or in development that are run on the Company’s T2Dx Instrument, powered by miniaturized magnetic-resonance (T2MR) technology.
Rapid diagnostic tests play a role in preventing spread of antibiotic resistance. Often, a doctor will make an educated guess as to what kind of antibiotic a patient needs, and administer it, while awaiting diagnostic results. If a patient takes an antibiotic for days that proves to be inappropriate, there is the risk of developing resistance to that antibiotic and then spreading that resistant organism to others through shed cells. When that antibiotic is truly needed, it may not work for the patient. Diagnostics that take only hours as opposed to days can lower the risk of resistance.
Cloud-based infection-prevention software
Tip: Sometimes it is good to have your head in the clouds
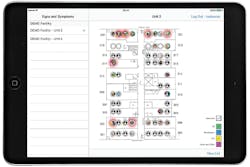
We are wrapping up with our head in the clouds. It is amazing how much work is accomplished unseen, in the “cloud.” One such product is offered by HealthConnex. Alex Hunter, Senior Project Manager, HealthConnex, CKMHealthcare, broke down how it works for those of us who are technologically impaired. “HealthConnex is a cloud-based infection-prevention and -control software as a service solution that improves resident safety and helps to reduce time needed to collect and report on infection-control–related data. The software, designed specifically for skilled-nursing and senior-living facilities, incorporates the use of innovative mobile apps, reducing time needed to collect hand-hygiene and signs-and-symptoms data.
Much like rapid diagnostic tests, one of the software’s advantages is that it can save precious time, allowing for earlier identification of a possible infection or an outbreak. Hunter further explained that these apps utilize “a unique rules engine, based on McGeer criteria, to alert staff of possible, confirmed, and suspected infection cases, as well as outbreaks, in real time as symptoms are recorded. HealthConnex allows staff to capture and report on information including infection cases, laboratory results, hand-hygiene audits, immunization, antibiotic-resistant organisms and multidrug-resistant organism history, and more.”
Hunter described the experience of a 155-bed long-term–care home in Canada that was able to minimize the effects of an outbreak by using the HealthConnex Signs & Symptoms app. “In January 2019, the home recorded early-onset symptoms in residents, viewed clusters of symptoms on our unique floor-plan mapping, and quarantined residents, identifying best-practice precautions. The home successfully identified the outbreak, leading to faster treatment and a safer environment for other residents.”
“Historically,” continued Hunter, “an outbreak during influenza season regularly consisted of approximately twenty to twenty-five suspected and confirmed cases across the home, normally lasting for two months.” In contrast, this time the home was able to reduce the outbreak to just two confirmed cases and two suspected cases on one unit, declaring an outbreak within three days of onset and resolving the outbreak in less than two weeks of onset. The results were good all-round. Hunter briefly outlined some positive outcomes from use of the HealthConnex Signs & Symptoms app. “The home was able to reduce costs from the smaller outbreak, no staff time was lost due to sickness, and they were able to maintain revenue by continuing to admit to other areas of the home.”
Conclusion
The many facets of infection prevention and control translate into many opportunities for improvement. Sometimes little effort or investment is required. It may take only a tweak in best practices or a linear change in a product to reap the desired results. Anything that can reduce risk of infection and save time to diagnosis and action to therapy is an enormous advantage for patient and staff alike. Bigger projects may mean a bigger bite out of the budget, but a closer examination may reveal resultant cost savings over a period of time as well as improved patient care. A win-win is always welcome.
References
1. Centers for Disease Control and Prevention. HAI data. https://www.cdc.gov/hai/data/index.html. Last accessed October 3, 2019.
2. Centers for Disease Control and Prevention. Current HAI progress report: 2017 national and state healthcare-associated infections progress report. https://www.cdc.gov/hai/data/portal/progress-report.html. Last accessed October 3, 2019.
3. Dao ML. Prevalence of methicillin-resistant Staphylococcus aureus (MRSA) and Clostridium difficile (C. diff) on shoe soles, and effect of their exposure to the GEM’s SoleMate Sanitizing Device (SSD). https://www.patho3gen.com/wp-content/uploads/Dao_Final-Report-on-GEM-SSD-at-Hospital_9-3-2017-.pdf. Last accessed October 4, 2019.
4. Schuman K, Cass T. Battling hospital-acquired Clostridium difficile with innovative infection prevention tools. Am J Infect Control. 2018;46(6);S87.
5. McCord J, Prewitt M, Dyakova E, et al. Reduction in Clostridium difficile infection associated with the introduction of hydrogen peroxide vapour automated room disinfection. J Hosp Infect. 2016 Oct;94(2):185-187.
About the Author

Susan Cantrell
Susan Cantrell is Infection Prevention Editor for Healthcare Purchasing News.