Let's get right down to it – healthcare facilities can be dangerous environments. Healthcare staff members are exposed to a wide range of hazards – from the bodily fluids of infectious patients to toxic chemicals and drugs. This includes everyone from the nurse at the bedside to the central sterile/sterile processing department (CS/SPD) professional in decontamination, as well as product and service suppliers that enter the environment. Patients too are at risk – from contaminated instruments, devices and surfaces.
In this article, we examine basic guidelines for selecting personal protective equipment (PPE), specific needs based on the environment (e.g. patient bedside, OR, CS/SPD), and special PPE considerations (e.g. infectious diseases, toxic drugs). We include commentary from infection prevention and CS/SPD professionals, including some items on their PPE wish lists, as well as insights from product and service suppliers on the latest PPE innovations.
PPE guidelines and standards
The Occupational Safety and Health Administration (OSHA) defines PPE as:
"Equipment worn to minimize exposure to hazards that cause serious workplace injuries and illnesses. These injuries and illnesses may result from contact with chemical, radiological, physical, electrical, mechanical, or other workplace hazards. Personal protective equipment may include items such as gloves, safety glasses and shoes, earplugs or muffs, hard hats, respirators, or coveralls, vests and full body suits."1
The Centers for Disease Control and Prevention (CDC) offers Standard Precautions for use in all patient care, including recommendations for improved use of PPE by healthcare personnel. In its Guidance for the Selection and Use of Personal Protective Equipment (PPE) in Healthcare Settings, the CDC specifies the following PPE: Gloves to protect the hands, gowns or aprons to protect the skin and/or clothing, masks and respirators to protect the mouth and nose, goggles to protect the eyes, and face shields to protect the entire face. The organization offers three considerations when selecting PPE: Anticipated exposure, durability and appropriateness, and fit.2
"We should always practice with the standard precautions in mind to keep ourselves safe from whatever possible infection we may get from touching the patients or entering their environment," said Paulina Rodriguez, RN, Infection Control Practitioner, Abilene Regional Medical Center, Abilene, TX.
"The correct use of the PPE is multifaceted: We must provide proper protection to our employees in all environments in order to be compliant with OSHA, the manufacturers' instructions for use and compliance to the safety data sheets (SDS)," said Mary K. Lane, MHA, CSPDM, CSPDS, CSPDT, MK Lane, SPD Consulting. "Failure to do so can result not only in an employee injury, but also liability issues and a negative finding on a regulatory survey."
Anticipated exposure
The CDC says PPE selection should be determined by the type of anticipated exposure, such as touch, splashes or sprays, or large volumes of blood or body fluids that might penetrate the clothing.
"Selecting the most appropriate PPE begins with a careful assessment of the level(s) of protection needed, especially the degree of fluid or biohazard exposure," said Edmund S. Tai, Vice President of Healthcare, Tronex International.
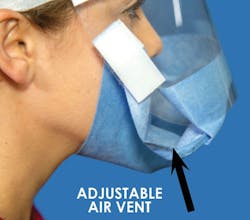
"Although face shields are generally recognized as a good PPE option due to deficiencies that exist in traditional models both the CDC and many other healthcare professionals believe that face shields should not be used as solitary facial protection, but rather as an adjunctive tool to other PPE," said Machson. "However, until the Drape Short 18000S came along, there were no face shields on the market that met the CDC's recommendations."
Durability and appropriateness
When selecting PPE, the CDC says healthcare facilities must assess its durability and appropriateness for the environment and task at hand. For example, determining whether a gown must be fluid resistant, fluid proof or neither based on its use and anticipated risks.
"We are one of the only launderers who do this – and we do it every time, to keep compliance easy for our healthcare facilities customers," said Geraghty. "PPE is about protection of your staff. When considering PPE, it depends on the risk and ease of use of the situation. Ultimately, you have to make compliance practical. That doesn't mean you shouldn't prioritize safety. What it means is building in processes that make it easy for staff."
Fit
Healthcare workers come in all shapes and sizes; therefore, each individual must have PPE that fits properly. For example, a gown that fit a six-foot tall, 200 lb man is unlikely to fit his five-foot tall, 120 lb female co-worker. The CDC states, "it is up to the employer to ensure that all PPE are available in sizes appropriate for the workforce that must be protected."
"Proper fit for the range of end users, and overall comfort/breathability through duration of use, are important considerations as well," said Tai. "Product designs that help to ensure proper donning and doffing practices are often of added value."
Comfort
Beyond fit another important consideration is comfort. Compliance levels could be lower if staff members find PPE uncomfortable or challenging to put on or take off.
"Choosing the highest level of protection should be the first consideration with any PPE, followed by comfort, ease of use and cost-effectiveness," said Dr. Alex Birrell, CEO, CleanSpace Technology. "Without comfort, you will not get satisfactory staff compliance, the equipment is under or poorly utilized, front-line staff are not protected, and patient care can be compromised.
With regards to the CS/SPD, there is a balance between protecting staff members from exposure or injury, and preventing them from becoming overheated as a result of the protective layers, particularly in decontamination. Sharon Greene-Golden, BA, CRCST, CER, SME, FCS, points out how the ANSI/AAMI ST79:2017 gives the alternatives for keeping cool in the decontamination area in Annex Q for the standards:
"It is our fiduciary responsibility to the staff members that we supply them with the best protection that allows them to function without the stress of getting wet or overheating," said Greene-Golden. All PPE is not created equal and the cost sometimes hinders the selection of the best product.
"You can visit 10 hospitals and all 10 will have a different interpretation of the PPE needed in the decontamination area," Greene-Golden added. "I tend to err on the side of complete safety for my team members because as I state daily 'PPE is all about me.' We have the best leak-proof, impervious, water resistant gowns and gloves that we can purchase for our team. We recently added jumpsuits that meet the criteria to our supplies because some of our members get wet or sweat from the inside out. They must stop and change once or twice during an eight-hour shift. The PPE selected must protect and give comfort to the workers while they are wearing these items to decontaminate and clean items."
Cost
While in an ideal world, every staff member in every department in every healthcare facility would have the optimal PPE in terms of level of protection, durability, fit and comfort, cost is an in important consideration as every aspect of healthcare attempts to do more with less.
"Even with the increased price of synthetic gloves, hospitals can reduce total costs standardizing to Biogel synthetic gloves," said Seltzer. "A case study found that Alta Bates Summit Medical Center's 100 percent conversion to Biogel synthetic surgical gloves significantly reduced overall costs by 25 percent, saving $74,542."3
According to Tai, as more healthcare systems move toward category-wide standardization, selection of PPE across the range of applications is driven by the following factors: Consolidating product variation to optimize program and operational efficiency while preserving proper protection levels for each application and, when possible, that products incorporate features that support high compliance and encourage proper use across many facilities and tens of thousands of end-users.
"Cost is usually a priority as well, driven by careful product selection to minimize the purchasing of significantly more protection than needed or ideal for a given application," he added.
Tronex has developed clinically accepted national product formularies for major health systems that incorporate evolving industry standards and the latest product designs, while delivering on the critical aspects of product craftsmanship, construction, and optimal protection.
"Sustainability is a trend with serious impact," said Peg Fox, MSN, BSN, RN, National Director of Surgical Services, Standard Textile. "Providing safety is primary but recognizing that we need to improve environmental stewardship is reflected in stances like AORN's Position Statement on Environmental Responsibility. Decreasing carbon footprint in the OR can be supported through reusable PPE. Reusables offer research-supported4 energy, water, and waste savings, as well as improved comfort and protective properties."
"Hospitals are challenged with providing more affordable care while also providing the highest safety measures," Fox added. "If we seriously evaluate reusable PPE for the OR and other sensitive areas of the hospital, we are addressing the sustainability challenge, as well as the significant potential cost savings of reducing hazardous waste. There is a place in a hospital's supply chain where reusables and disposables can be used in coordination, providing safety and increasing environmental leadership."
PPE considerations by department
Healthcare environments are as diverse as the patients they treat; therefore, healthcare workers require PPE specific to their department and tasks, as Chris Franklin, CRCST, CIS, CFER, Owner, The SPD Network, Endo Tech, IU Health explains:
"There's an understanding that PPE is a requirement in certain hospital settings, whether it be providing patient care, cleaning up a chemical spill or decontaminating surgical instruments," said Franklin. "However, what's not always clear is that not all PPE are universal, meaning that some circumstances call for specifically designed PPE. It's important that not only do personnel have the correct PPE for the job, but also know how to distinguish between them."
"For example, while a simple pair of latex gloves is acceptable in most areas of the hospital, instrument decontamination requires a thicker, puncture resistant glove with an extended sleeve. Our PPE policies follow recommendations from AAMI, AORN and other professional organizations," Franklin added.
Operating room (OR)
As Rodriguez explains, PPE in the OR is largely dependent upon the procedure being performed, stating:
"If you are cutting into bone or performing an open heart surgery, the OR staff might have full gowning. When there is a very bloody case, such as a C-section or some GI procedures, staff can wear shoe covers that go above the knee. PPE in the OR is very driven by AORN standards. At this time of year when the weather becomes colder, men often want to grow out their beards. In accordance with AORN standards, they must wear beard covers, and there are even sideburn covers available."
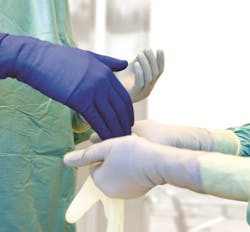
Because gloves are such a critical part of PPE in the OR, Seltzer recommends that those responsible for glove selection request data from glove manufacturers so they can compare performance, stating:
"Surgical gloves differ substantially when comparing in-use failure rates. A surgical staff-based observational research study comprised of five facilities found statistically significant results concluding that non-Biogel gloves were at least 3.5 times as likely to fail as Biogel gloves."5
Patient bedside
Clinicians care for a wide range of patients; therefore, PPE selection for bedside care varies broadly based on the patient's condition and course of treatment. While Rodriguez stresses the importance of following standard precautions, there are times when clinicians must make their own decisions regarding the level of protection they need when providing care.
"If you are a nurse coming into a patient's room you must be prepared for any possible exposure to bodily fluid. A patient does not need to be in isolation in order for you to follow standard practices," said Rodriguez. "But sometimes we see incidents occur, such as splashes, because a nurse did not go beyond standard precautions to protect him or herself. So if you see a sign on the door that says 'contact transmission,' be aware that you should be wearing gloves and a gown and possibly a mask. Or if the sign says 'droplet transmission,' put on your shielded mask."
CS/SPD
Damien Berg, Regional Manager of Sterile Processing at UCHealth, Immediate Past President of International Association of Healthcare Central Service Materiel Management (IAHCSMM), says decontamination can be a challenging – and confusing – area when it comes to selecting appropriate PPE.
"Some say the moment you walk through the decontamination threshold you have to be in 100 percent PPE, then others say you just need booties with your scrubs," said Berg. "You have to personally evaluate your own department's workflow for areas of potential contamination and plan the PPE from there. I believe everything in decontamination has the potential for contact contamination – the walls, floors, doorknobs, etc. Therefore, anyone entering decontamination should be wearing gloves – even if they are just stopping in to say 'hi' – because you never know when you might touch something."
Greene-Golden points to the standard precautions and other industry guidance documents that are available to help CS/SPD professionals select the proper PPE, stating:
"The selection of PPE for the sterile processing department is selected by the facility that will be using the product through their material management, sterile processing and infection control departments. Factors used are in accordance with OSHA requirements, ANSI/AAMI ST79:2017 recommended practice standards, and the AORN."
"Technicians and other vital staff members may come in contact with physical, chemical or mechanical hazards, such as the transportation or maintenance crew. For instance, you contact a maintenance technician for calibration of the enzymatic dispenser. In accordance with the enzymatic dispenser's instructions for use, the maintenance technician should wear the appropriate eyewear protection such as fitted goggles or safety spectacles."
Nancy Chobin, RN, AAS, ACSP, CSPM, CFER, President, Sterile Processing University, points out how the PPE selected for the CS/SPD relates not only to the tasks at hand but also the specific chemical(s) in use," stating:
"Therefore, the PPE required for the chemical in use should reference the PPE recommended by the chemical manufacturer and the safety data sheet (SDS)."
Berg recommends that CS/SPD professionals and healthcare industry associations, including the Association for Professionals in Infection Control and Epidemiology (APIC), International Association of Healthcare Central Service Materiel Management (IAHCSMM), Association of periOperative Registered Nurses (AORN), Society of Gastroenterology Nurses and Associates (SGNA) and Association for the Advancement of Medical Instrumentation (AAMI), come together to discuss best practices in PPE. He states:
"I've seen more collaboration among these groups than I have seen in years. We have different points of view so let's have a discussion, learn from each other and work together because we are all working toward the same goal."
Special considerations
While PPE is a part of the normal workflow in most areas of healthcare, there are specific instances where PPE considerations extend beyond the day-to-day or outside of what is typically considered when thinking about the care delivery environment.
Infectious disease outbreaks
Deadly infectious disease outbreaks, such as SARS and Ebola, have called attention to the need to protect healthcare workers and patients. The SARS outbreak of 2003, sickened nearly 8,500 people, claimed 900 lives and cost an estimated $40 billion across East Asia Canada and the United States.6
"Recent epidemics highlighted the acute need for training and improved PPE in healthcare settings," said Birrell. "In the case of SARS in North America, 20-40 percent of people who contracted the illness were healthcare workers. Many leading hospitals are currently implementing pandemic preparedness programs. Globally hospitals are now looking for innovative, reusable solutions that offer high protection, easy training, ease of use and comfort."
"A major lesson for healthcare providers from epidemics is the huge challenge of stockpiling and shortages of disposable masks," Birrel added. "There are 18 million workers across 5,500 hospitals in the U.S. It has been calculated that 7.3 billion N95 masks would be needed to protect workers during a pandemic. Currently 60 million masks are stockpiled."
Greene-Golden says her hospital has in place specific PPE processes should they admit an Ebola patient. It requires gowns, jump suits, special shoes and gloves. It also requires a distinct process for donning and doffing the PPE.
"For our clients, the waste handling of standard infectious material is the primary concern," said Brandie Laudel, Facility Planning and Development, San-I-Pak. "Many clients are also responsible for treating special pathogen patients, like those with Ebola. In the Ebola setting, shelf life is a critical concern. Hospitals are spending significant capital to stock up for situations that may not happen. A shorter shelf-life translates into higher cost."
"PPE is perceived as a 'hassle' by staff in their day-to-day performance of their jobs," said Steve Hilliker, Sr. Facility Planning and Development, San-I-Pak. "The Johns Hopkins Center for Bioengineering and Innovation & Design (CBID) developed a new PPE for use areas where Ebola is being treated. They specifically designed it to make donning and doffing easier and safer for the staff. This approach, intentionally seeking improvements to design, can be applied to everyday PPE."
Drug administration
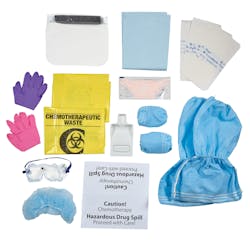
According to Greg Metcalf, Global Director for Gloves and Apparel, Halyard, hospitals must be especially careful to follow protocol when working with hazardous materials such as cytotoxic chemotherapy drugs. He points out how new USP General Chapter <800> guidelines require hospitals to provide appropriate PPE for employees handling potentially hazardous drugs, as well as to have spill kits available anywhere in the facility where employees are handling them. Guidelines to ensure proper protection include the following PPE:
- Coverage for hair and beards
- Goggles and a face shield
- A fit-tested N95 respirator mask
- 2 pairs of gloves tested against drugs commonly used in chemotherapy
- A chemo-rated impervious gown that extends below knees and closes in the back
- Shoe or boot covers
"With PPE, a trend that never disappears is its ability to meet the most stringent of industry guidelines, especially when dealing with hazardous drugs," said Metcalf. "Beyond that, there is an increased focus on customization of PPE bundles so hospitals can tailor orders to meet their specific protocols. For example, by creating customized bundles, or kits, for PPE related to administration and spills of hazardous materials such as cytotoxic chemotherapy drugs, that eliminates the need for hospital staff to pull the individual components that are needed to safely deliver or clean up chemotherapy drugs. This creates efficiencies and saves valuable time for clinicians, while also ensuring that all the PPE needed to meet guidelines is included."
Service providers
Healthcare facilities require a number of service providers to keep their operations up and running. There is the potential that an individual could bring contaminants into the care setting, or carry dangerous organisms out beyond the four walls of the hospital or other facility. Therefore, there are a whole other set of PPE considerations for these individuals and their tasks.
"Pest management professionals should always wear proper PPE to inspect. They should also follow all label language on PPEs when performing any treatments. From a pest management standpoint, ensure that your pest management company understands your particular site and any specific PPE that might be necessary. A good provider will ensure that those who are servicing a healthcare facility have clean uniforms and shoes, as well as
equipment."
"From a pest management aspect, we are engineering our PPE in many cases," said Hartzer. "We use products that do not require much or any PPE. We focus on preventing issues, which allows for less product use and limits the necessity to access and work in difficult areas that require PPE."
What is in your PPE wish list?
We asked healthcare professionals what PPE items they would like to see manufacturers develop to meet their needs and received the following responses.
Keeping it safe and cool in decontamination
"I would like to see antimicrobial/reusable sweatbands and a cooling aid created specifically for those that work in the decontamination area," said Pettyjohn. "This area is notorious for making a technician hot, after donning all the required PPE and performing tedious work at the reprocessing sink. Not to mention all the machines that are generating heat."
"I wish some of the PPE was made of 'breatheable' material so it was not so uncomfortable," said Chobin. "While there are methods such as cooling vests that can be used beneath PPE, it is another cost factor."
"An option for a cooler gown in the decontamination area that is not cost prohibitive," said Lane. "The options now are limited and most of the cooler gowns are not approved by materials management and value analysis due to cost."
Safe and easy transport for isolation patients
Rodriguez explains the challenges of transporting patients from one clinical area to another and the challenges that presents from a PPE perspective. On her wish list is an all-encasing isolation barrier for transport. She states:
"When transporting a patient, say either from a unit by transporter or from isolation in the ICU, I always get asked, 'Who wears the PPE – the nurse or the patient? And when you are transporting them in a bed, what happens to that bed? Say the patient has MRSA. If they sneeze on themselves then it is all over the bed. If they touch their nose then they touch the bedrails, the IV catheter, the foley catheter or anything else then they put the microorganism there. Then their whole environment within the proximity of their nose and body is evident with that microorganism.
"We tell our staff to wear PPE but I wish there was an all encasing isolation solution that would encase the bed momentarily with a banner or something that would flag the clinical person to the transmission dangers," she added.
References
1. Occupational Safety and Health Administration (OSHA) Personal Protective Equipment, https://www.osha.gov/SLTC/personalprotectiveequipment/
2. CDC Guidance for the Selection and Use of Personal Protective Equipment (PPE) in Healthcare Settings, https://www.cdc.gov/HAI/pdfs/ppe/PPEslides6-29-04.pdf
3. Wharton, Kurt R., Thomas, J,, Henderdon, Phillippe,, "Can converting to synthetic surgical gloves lower hospital operating room costs? OR Manager, May 2016
4. Conrardy J, Hillanbrand M, Myers S, Nussbaum G.F. (2010). Reducing Medical Waste. AORN Journal,91,717-18. https://aornjournal.onlinelibrary.wiley.com/doi/abs/10.1016/j.aorn.2009.12.029
5. MHC Study #G09-005
6. More than a decade later, SARS offers lessons on Ebola, Los Angeles Times, October 19, 2014 https://www.latimes.com/science/la-sci-ebola-sars-20141018-story.html
About the Author
Kara Nadeau
Senior Contributing Editor
Kara Nadeau is Sterile Processing Editor for Healthcare Purchasing News.