Managing pain, temperature two sides of the same coin?
Call them the kinfolk of patient physiology joined at the hip. Clinicians and medical experts regard temperature as one of the primary vital signs, while pain represents one of the primary indicators of health and wellness. With pain, temperature generally escalates; higher temperatures can lead to rising pain.
Because a high fever may cause pain you have to break the fever. To manage aching joints and muscles, however, you may apply heat. To operate on the body safely and with minimal-to-no pain you manage the body temperature and anesthetize or numb nerves and tissue. To help the body heal you manage temperature and relieve pain through medicinal or technological means.
Pain also can affect the other vital signs besides body temperature, causing fluctuations in pulse rate, respiration rate and blood pressure.
When caring for critical and surgical patients the management of pain and temperature fit like hand-in-glove. There’s something synergistic, if not complementary, between the two.
Jessica Mathieson, Vice President and General Manager of Acute Care, Stryker Corp., makes the connection, too.
But managing pain and/or managing temperature doesn’t necessarily gravitate toward medications and pharmaceuticals, such as acetaminophen, analgesics, ibuprofen, opioids and other pain killers. Holistically, the tasks span the gamut between the clinicians – nurse and physician, products, staff and system as well as the patient.
Clinicians and patients have a variety of non-pharmaceutical options when it comes to managing pain. Over-the-counter (OTC) and prescription devices, therapies and technologies to relieve chronic or post-surgical pain can include wearable heat pads and patches and sensors, transcutaneous electrical nerve stimulation (TENS) devices, radiofrequency ablation and radiofrequency catheter ablation devices, spinal cord devices that deliver electrical impulses and stimulation and devices that emit infrared light as alternatives to meds.
For temperature, clinicians and patients also can choose from a variety of OTC and prescription devices, therapies and technologies that start with non-contact and direct-contact external thermometers to warming and cooling devices as well as core/whole-body temperature control and localized temperature control devices that can be used during the entire perioperative process – from patient room to surgical suite to recovery and the transport in between and post-discharge. These devices and technologies also involve a variety of blankets, gel pads, packs, central venous catheters.
Clinical experts know that managing pain and temperature extends well beyond patient comfort and convenience. The mere act of maintaining a patient’s normothermia, defined as the normal core body temperature, during surgical procedures, can prevent a number of dangerous complications, according to experts at Gentherm Medical, which actively promotes patient temperature management as part of its “Right Now” campaign.
Failure to manage patient temperature properly can lead to increased risks for such complications as adverse myocardial outcomes, surgical site infections, increased blood loss, impaired wound healing, lengthened hospital stays and recovery time and increased transfusion requirements, states Gentherm Medical, which also translates to additional charges on billing and higher surgical expenses overall.
Product demand challenges
Stryker’s Mathieson stresses the volatility of demand and supply for temperature management techniques and technologies.
“Demand in the market for temperature management (TM) can be somewhat volatile based on accepted practices and recommendations,” she noted. “For example, as new studies come to market and new disease states like COVID introduce large patient populations in need of TM devices, demand increases. In 2020, we saw rapid demand growth for TM devices and disposables, which could help to control patient fevers that were unmanageable through medication alone. In addition, in more recent months, hospitals are seeing high-acuity patients from Cardiac to Neuro ICUs who are also in need of temperature management, but from a more precise and controlled device. The market needs accessible and versatile TM products throughout the continuum of care.”
But patient temperature management decision-making extends beyond device availability.
“TM encompasses both low acuity warming and cooling to achieve normothermia, in addition to more critical Targeted Temperature Management protocols, which require the caregiver to start treatment quickly and manage temperature precisely,” Mathieson explained. “Finding a device which offers multiple modes, disposables and safety features to meet both needs can be a challenge for hospitals. In addition, infection prevention is at the top of caregivers’ minds more than ever, which makes it important that any TM device is safe in highly critical environments.”
A simultaneous multi-faceted technique would be welcome, according to Sarah Ford, RN, CCRN-A, Lead Clinical Advisor, Medical Division, Gentherm Medical.
“In the perioperative area temperature is one of many factors in preventing adverse outcomes,” Ford said. “There is a need for temperature control combined with pressure reduction and moisture diversion away from the skin. A way to monitor skin temp, change patient temperature and reduce pressure at the same time with the same device would be impressive. In the ER and critical care, portability and data collection/transmission are being requested with increasing frequency.”
Augustine Surgical’s Scott Augustine points to a lower-tech issue at stake.
“The current demand challenges for temperature management devices [involve] the unavailability of disposable blankets,” Augustine said. “Our customers report that many forced-air products have been backordered for some time due to supply chain issues. When unavailability is added to forced-air warming’s other drawbacks – moderate effectiveness, increased implant infection risks, increased disposal costs and much bigger carbon footprint – many hospitals are switching to reusable products such as HotDog Patient Warming. While this has created production challenges for us, we have been able to meet the increased demand.”
Ecolab acknowledges the supply chain disruptions in components, raw materials and procedure volume changes since COVID-19 emerged, too, according to Ryan Cushman, Assistant Marketing Manager, Healthcare, Surgical Solutions.
“Supply chain disruptions have been felt across nearly every industry and patient temperature management [medical] devices have not been exceptions,” Cushman said. “Managing inventories and mitigating backorders for products that are involved in life-saving procedures elevates the pressure and urgency for our teams.
“Since the COVID-19 pandemic really started making an impact in early 2020, procedure volume has declined and to date, has not completely rebounded to pre-pandemic levels,” he continued. “In addition, hospitals have had to reallocate resources and trim budgets as they have seen reduced revenue-generating elective procedures. Business development plans and budgets have had to make big adjustments for these market shifts.”
Necessary device, process improvements
Devices and products used to manage pain and temperature may have undergone considerable advancements and development over the years, but clinical experts acknowledge more room for continued improvement.
“The medical community’s response to the COVID pandemic resulted in new importance of temperature screening at the hospital and clinic/office level, and this demand for quick and easy measurement unfortunately spawned the proliferation of many limited-capability thermometers which, at best, were focused on consumer/retail applications and low-acuity situations,” he noted. “It’s important to understand that performance at the true professional level is only offered by instruments which have been clinically documented and approved for use in high-acuity medical environments.”
Augustine, an anesthesiologist and inventor, concentrates on the physical application and procedure.
“The single biggest improvement in patient temperature management devices is warming simultaneously from above and below” he said. “Warming effectiveness is directly proportional to the amount of skin surface in contact with the heat. Warming from above only, for example with a forced-air blanket, results in failing to reach normothermia (therapeutic failure) in 30% to 50% of surgeries. In contrast, warming from above and below simultaneously, results in less than 4% therapeutic failure.”
Gentherm Medical’s Ford cites footprint. “Decreasing the size of patient temperature management devices and making them portable would be how I would improve existing patient temperature management devices,” she noted.
Stryker’s Mathieson, however, focuses on facilitation and quality. “Temperature management devices and products need to be easy to use and safe,” she said. “Temperature management devices continue to improve in accuracy and precision, which helps to prevent patient instability linked to post-therapy complications – but the ease of use of these devices and the safety of the water and air quality could use improvement.”
Seven years ago, the Food and Drug Administration began notifying the healthcare industry about the aerosolization of microbes from water-based devices and the linkage to patient infections, according to Mathieson.
“Since 2015, several additional notifications have gone out – as recently as 2021 – but many devices are not meeting the higher disinfection standards which guarantee the devices are safe enough for use, even in the OR,” she continued. “Achieving this high-level disinfection is key for patient and caregiver safety but reducing frequency and simplifying the process would greatly benefit nurses in the current staffing environment.”
Looking forward
As healthcare organizations evaluate and invest in pain and temperature management devices and technologies, Benincasa, Augustine, Cushman and Ford offer relevant and useful tips for supply chain to consider.
“When your organization is considering upgrading your temperature management devices, be sure that the instrument is designed specifically for professional clinical use, covered by a strong warranty and easy-to-access technical support; offers accessories such as wall-mounts, basket-mounts, calibration checkers, security tethers (where needed) and other items which will help maintain process utilization and strengthen performance,” Thermomedics’ Benincasa advised.
Augustine insists on assessing the patient’s condition while on the surgical table.
“The majority of hospitals still use forced-air warming blankets, which result in 30% to 50% failure to reach normothermia,” he said. “Hypothermic patients, especially if they are shivering, experience significantly more pain and general discomfort than normothermic patients. I invented Bair Hugger forced-air warming 35 years ago specifically to address the issue of significant postoperative discomfort due to hypothermia. To achieve surgical normothermia, the clear solution is to warm from above and below simultaneously.”
Ecolab’s Cushman echoes the importance of maintaining normothermia for surgical patients.
“Many organizations don’t recognize the value of the improvements made in irrigation fluid temperature and volume tracking during invasive procedures,” he noted. “Maintaining patient normothermia has been linked to improved patient outcomes. Negative patient outcomes can be tremendously costly for healthcare organizations.”
Ford recommends portability. “Continuous therapy with a portable device – especially for perioperative warming – is missing at most facilities,” she said. “This ability to have your patients warm and comfortable as they are preparing for surgery, having surgery and recovering from surgery would improve outcomes and improve patient satisfaction.”
Mathieson expresses concern about device and equipment age, cautioning how that can affect quality outcomes.
“Many facilities maintain temperature management technology that is decades old,” she noted. “This older technology often has outdated algorithms that check in on patient temperature a couple of times per hour, rather than every few seconds – which limits their ability to precisely control patient temperature and increases the likelihood for a patient temperature overshoot. In addition, older temperature management technology also often has limited disposables which are not insulated, easy to clean or self-sealing. Newer disposables help with heat transfer to control patient temperature more precisely and improve clinical efficiency through ease of use and by reducing water spills and limiting pad replacement due to patient bioburden.”
Mathieson encourages hospitals that are not seeing the precision or control they need to look to new devices for improved precision.
“Hospitals that are struggling with nurse turnover and staff shortages should consider upgrading to new TM technology for newer easy-to-use technology that will improve efficiency in the TM treatment process,” she recommended. “Lastly, hospitals that are renewing focus on wound care and infection prevention should consider newer technology that does not aerosolize microbes and promotes skin integrity through the use of non-adhesive disposables.”
Pain Management device and technology companies
Abbott Laboratories |
https://www.neuromodulation.abbott/us/en/hcp/products/radiofrequency-chronic-pain/ionic-rf-generator.html |
AVACEN Medical |
https://www.avacen.com/ |
BioElectronics Corp. |
https://www.bielcorp.com/products/ |
Bioventus LLC |
https://stimrouter.com/ |
Boston Scientific |
https://www.bostonscientific.com/en-US/medical-specialties/pain-management/products.html |
Diros Technology Inc. |
https://dirostech.com/ |
O&M Halyard |
https://products.halyardhealth.com/patient-care-supplies/heat-cold-therapy.html |
NeuroMetrix |
https://www.quellrelief.com |
NovaaLab |
https://novaalab.com/ |
Omron |
https://healthcare.omron.com/healthcare-solutions/pain-management |
PainPod Biotechnology |
https://painpodusa.com/ |
Smiths Medical, an ICU Medical company |
https://www.smiths-medical.com/en-us/products |
SPR Therapeutics |
https://www.sprtherapeutics.com/physicians/ |
Temperature Management device and technology companies
3M Health Care |
https://www.3m.com/3M/en_US/p/c/medical/temperature-management/i/health-care/ |
Augustine Surgical |
https://www.augustinesurgical.com/ |
Exergen Corp. |
https://www.exergen.com/ |
Gentherm Medical |
https://www.gentherm.com/en/medical/home# for hyper-hypothermia, normothermia, localized therapy and blood temperature control |
Medtronic |
https://www.medtronic.com/covidien/en-us/products/temperature-management.html |
O&M Halyard |
https://products.halyardhealth.com/surgical-solutions/temperature-management.html |
Pintler Medical |
https://www.pintlermedical.com/our-family-of-products/ |
Smiths Medical, an ICU Medical company |
https://www.smiths-medical.com/en-us/products |
Stryker Corp. |
https://www.stryker.com/us/en/portfolios/medical-surgical-equipment/temperature-management.html |
Thermomedics Inc. |
https://www.thermomedics.com/ |
ZOLL Medical Corp. |
https://www.zoll.com/medical-technology/temperature-management |
Augustine Surgical HotDog Patient Warming System

Achieve better normothermia outcomes by warming above and below the patient simultaneously, which the versatile HotDog® Patient Warming System does efficiently with the WC77 Controller, U101 Warming Mattress overlay, and B500 Universal Blanket.
CareGiver Thermometer from Thermomedics

THE CAREGIVER® PROFESSIONAL is a clinical-grade infrared thermometer for measurement of forehead temperature in adults, children, and infants without contact. It is designed for use in a wide variation of medical settings and can also deliver ambient/skin surface temperatures with the flick of a switch.
Ecolab Hush Slush 2.0
The newest offering in patient temperature management products is the Ecolab Hush Slush 2.0. This device is primarily used in open heart and transplant procedures. It is engineered to make velvety soft surgical slush that may aid in minimizing damage to sensitive organs or tissues. It comes with a built-in fluid warmer for surgical site irrigation and improvements to speed and safety over the previous generation of Ecolab ORS slush machines. Healthcare organizations more than ever need improved products they can rely on for the safety of their patients.
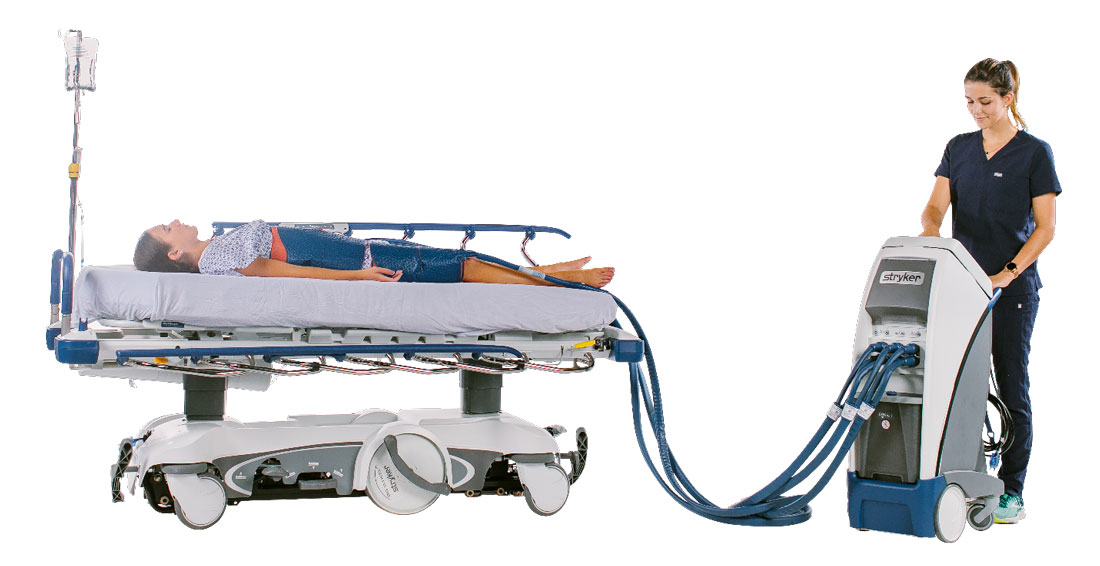
Altrix Temperature Management System from Stryker
Altrix is a Precision Temperature Management System which can be used throughout the care continuum. It offers three unique modes to meet the needs of both low and high acuity Temperature Management. Altrix can be set to manage water temperature alone, or to precisely manage patient temperature within 0.1oC by checking and responding to patient temperature every few seconds for Targeted Temperature Management. Altrix is simple for caregivers to use, highly critical with current nursing shortages and travel nurses, safe for patients by offering non-adhesive disposables to promote skin integrity and helping to protect the air around patients by preventing the aerosolization of microbes, and it is efficient for the facility due to its versatility of modes and disposables to meet the ever-changing TM needs throughout the hospital.
About the Author
Rick Dana Barlow
Senior Editor
Rick Dana Barlow is Senior Editor for Healthcare Purchasing News, an Endeavor Business Media publication. He can be reached at [email protected].