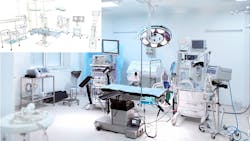
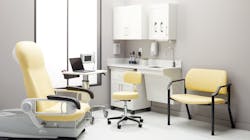
Might cross-functional, multipurpose rooms be standard operating procedure?
Designing and equipping rooms for multiple purposes may just be a universal strategy and tactic after all.
At home you can convert a bedroom to a den or even an office to accommodate work-from-home capabilities that grew in popularity during the COVID-19 pandemic. Churches remove stationary pews to enable the sanctuary to accommodate concerts, theatrical and physically demanding youth events. Colleges and universities convert common areas to dormitory rooms when student numbers surpass available living arrangements.
Even hospitals – particularly during the pandemic – converted waiting areas to exam and treatment rooms and intensive care units to accommodate patient overload. In fact, a number of healthcare provider refits and retrofits include multipurpose rooms to be used as demands dictate, switching between exam and treatment rooms to imaging and even outpatient surgery suites.
As healthcare provider organizations continue to struggle with intensified cost containment pressures post-pandemic, they need and welcome the convenience and flexibility that multipurpose rooms can offer, particularly if they can pivot their functionality, service and use rather quickly.
Boon and/or boom?
Observers contend that designing and operating multipurpose rooms within a hospital or outpatient facility not only can be a boon to those facilities and their patients but should lead to a boom in development.
Kurz lists a plethora of benefits emerging from the simple premise of making efficient use of limited resources. “A better patient experience is the result when fewer transfers are needed between different examination and procedure rooms,” Kurz indicated. “There is less risk to patients, comfort is improved, and patients are more confident in the continuity of care. Multiple procedures can be performed on the same day – one hospital visit, one sedation, one hospital stay for recovery – further reducing risk and stress to patients.
“A more efficient health facility emerges when interdisciplinary clinical needs are met in a single room,” she continued. “The CT system can be used for diagnostics, for example, when not in use for interventions. The versatility encourages a more efficient workflow, medical staff can seamlessly transition from task to task in the same room to minimize downtime, and physical space is used more efficiently to reduce operational costs. The result is a faster return on investment.”
“A more confident treatment plan is delivered when doctors and radiologic technologists have access to multiple sources of imaging information all in one room. CT angiography is a good example. And with access to multiple imaging capabilities and resources, doctors can develop new treatment techniques that expand minimally invasive options,” she added.
Multipurpose room design can be a strategic and tactical benefit based on real estate, according to David Horn, AIA, ACHA, director, Corporate Project Development, Surgical Solutions, STERIS. “The design of multipurpose spaces is a sound decision particularly for rural hospitals, landlocked urban hospitals and in preparation for a mass catastrophe or pandemic,” Horn noted. “The flexible nature of these spaces allows facilities to utilize a single or group of spaces more efficiently and effectively clinically and operationally. Additionally, the saved square footage of a combined/shared use space makes financial sense and allows facilities to effectively use underutilized and highly coveted hospital space.”
“Outpatient clinics are the primary target for standardizing exam and/or treatment rooms to leverage multiple types of providers that cover varying clinical specialties,” Redding recommended. “Many times, exam and/or treatment rooms in outpatient clinics are severely underutilized because there isn’t enough patient volume for a particular clinical specialty to justify the cost of building and operating the specialty clinic. Creating multi-disciplinary rooms makes sense clinically and financially but it can be challenging operationally to ensure the rooms have the right equipment and supplies for the particular specialty. Outpatient clinics are exploring options to create an exchange model for equipment and supplies to enable the quick transition of the room(s). Additionally, there are opportunities to standardize equipment to reduce usage variability and increase the availability of the right equipment.”
Redding further explains that certain specialties may be more amenable to multipurpose use than others.
“Creating a standard surgical procedure room is on the forefront of hospital architects but it doesn’t naturally translate into the same benefits as the exam and treatment rooms,” he said. “The reason is [that] each surgical specialty can have significantly different needs when it comes to supplies/implants and their specific equipment. The sheer volume of supplies and equipment requirements will create operational inefficiencies and most likely financial implications because it may take longer to turnover a reason and require more physical space to accommodate the movement of the necessary supplies, implants, and equipment.”
Timmerman points to several options for multi-purpose use that include the exam room, consultation space and options for telehealth.
“In a traditional exam room workflow, patient weight and height are captured manually in the hallway,” she explained. “A triage nook may be used as a semi-private space designed to assess and capture vital signs. The nook may also be a space where weight and height are taken. Optional equipment could include a wheelchair scale, a sink for proper hygiene and storage supplies. The patient is then escorted to the exam room and directed to a side chair or exam table for capturing additional health data. Most of these steps can be accomplished within the exam room if the exam room is designed appropriately.
“In a connected in-room vital signs workflow, the patient is directed to the exam chair to support proper positioning for blood pressure measurement,” Timmerman continued. “Weight, temperature, pulse, and blood pressure are captured via an integrated scale in the exam chair and a connected, automated vital signs device. All patient-related health information can be discussed during the process while the patient sits on the exam chair. All vital signs data can then be imported directly into the [electronic medical record], saving time and eliminating manual transcription errors. Studies have shown you can save 69 seconds per patient during the vital signs acquisition process by simply bringing all vital signs capture to the point of care.”
Still, Timmerman cautions that there are instances when a multipurpose room may be less than ideal. “For example, there may be a desire to share a space for procedures as well as primary care exams. However, the equipment for exams can be vastly different than the equipment needed for procedures,” she countered. “An exam chair is designed to support primary care functions such as vitals acquisition while a procedure chair is designed to promote access, versatility and a large range of motion. The average length of a procedure is [reported to be] 50 minutes, so a procedure chair needs to be designed for proper ergonomics for the physician and comfort for the patient. Procedure workflows can include a procedure zone designed for efficiency along with a consultation zone in one shared space.”
"On the pro side, multipurpose rooms are “nimbler, promoting efficiency, potentially lower operating costs and potentially increase revenue by reducing bottlenecks by transitioning rooms as needed,” Fitzgerald noted. “They may create more flexibility and may also result in the availability of more resources. A reduction in transfers from one unit to another can potentially reduce errors that sometimes happen during handoffs. Nimbleness can encourage flexibility and enable providers to adapt quickly to changing patient needs.”
On the con side, however, multipurpose rooms may create the “need to purchase more equipment up front to support each room, and sterility for some surgical procedures and certain laboratory tests could be challenging or impossible,” she cautioned.
Vizient’s Wallen argues that effective use of multi-purpose rooms can improve utilization based on flexibility and adaptability. In fact, one key to understanding and implementing cross-functional rooms is to recognize the difference between flexibility and adaptability as they represent two ways to improve utilization.
“Flexibility is the ease in which space can be utilized for various tasks and activities without the need to modify the space,” Wallen said. “In general, larger, contiguous, and more repetitive environments – settings for repeated tasks – yield greater flexibility. Additionally, if repetitive spaces are standardized to meet the optimal use, the space will be more flexible.” Wallen lists examples of repetitive rooms or spaces that may serve multiple functions that include:
· patient intake spaces
· pre- and post-op rooms
· exam/treatment rooms
· medication prep rooms
· clean supply rooms
· soiled holding/utility rooms
“Adaptability is the ease at which space can be quickly and easily modified to meet changing needs,” he continued. “This could include a change in staffing, equipment, technology, supplies, etc. Spaces that are modular and allow subsets to be created easily to account for changes in need are more adaptable. To the extent possible, standardizing repetitive spaces to meet the most complex need of the space is desirable. This is not to say that all rooms should be capable of providing care or support the highest levels of acuity, however it is saying that adaptability will provide the ability to change the utilization of the space based on higher acuity when needed.”
Aesthetic alikeness
Once a healthcare organization embraces the concept of cross-functional, multipurpose rooms the next step involves elements that facilitate workflow. One option may be to ensure that these rooms look and feel the same or similar when it comes to layout, equipment and supplies on site. Reviews are mixed.
Siemens’ Kurz sees many benefits with familiar aesthetics. “It’s not merely an aesthetic choice to build multipurpose rooms that look and feel alike, with uniformity between equipment and supplies,” she said. “It’s a smart strategic decision that assures significant clinical, financial, and operational advantages that contribute in real ways to quality patient care and the facility’s reputation.
“Technologists and doctors are a patient’s first line of defense in every procedure,” Kurz continued. “Their familiarity with the many systems in a multipurpose room is essential to a successful outcome. Deploying a common user interface enables staff to more easily reach a high level of efficiency when it matters most and avoid procedure-specific adjustments. We’ve seen firsthand how this allows providers to focus more on the patient and less on learning a new setup. Facilities benefit from streamlined training that saves time and money, and patients benefit from faster procedures because staff can more easily assimilate within the room.”
Equipment access represents a positive feature, according to Kurz. “The ability to use various equipment for all rooms is a clear cost-saving feature,” she indicated. “It’s uncommon in a traditional setting to share equipment or find compatibility between systems when rooms are not shared. The importance of uniformity, or at least finding commonality and uniformity across systems, is a smart way to minimize a room’s downtime, particularly during service or equipment repair. The reward for keeping maintenance costs low is clear.”
Workflow efficiencies must be apparent, according to Olympus’ Fitzgerald. “Consistency in rooms enables [healthcare practitioners] to move from room to room and use equipment without added training, which could increase speed to care,” she said.
STERIS’ Horn emphasizes the patient benefits. “The design/layout of these spaces should provide a comfortable environment for the patient while balancing the clinical needs of the caregiver in terms of workflow and circulation,” he noted. “Furthermore, from a consumer’s perspective, it's important to the space looks finished and not ad hoc to help instill comfort and confidence in the patient receiving treatment.”
For Midmark’s Timmerman, patient perception may be a prime motivator. “It is possible to design a functional space without discounting aesthetics,” she said. “In fact, aesthetics can have an impact on how a patient perceives the quality of the care being provided. Cluttered areas and supplies strewn across the exam room can appear unprofessional, unorganized, and even dirty. Therefore, it’s critical to balance functionality and aesthetics.
St. Onge’s Redding ponders the mobility and transportation challenges that cross-functional, multipurpose rooms might cause. “In theory, having the same equipment and supplies throughout every room are preferred, but unfortunately, with specialty specific equipment and supplies, operationally it may result in inefficiencies to continually move equipment and supplies based on the clinical need,” he noted. “Without a doubt, the room configuration can be consistent, but what ultimately is utilized for patient care will force some segregation of rooms. There is a fine line with balancing clinical flexibility and room availability without introducing considerable inefficiencies.”
Vizient’s Wallen stresses the need for standardization as the key ingredient for success. “Standardization is one of the most effective quality improvement concepts, yet it is infrequently and inconsistently utilized across most organizations,” he said. “Embracing the concept of standardization requires the full development, documentation and application of best practice(s) to ensure their sustainability. In turn, sustained best practices will promote safety, efficiency, quality and high reliability of both operations and outcomes. Standardization should be broadly applied to foster synergy between workflow design (standard work processes) and facility design (standard workspaces).”
But Wallen acknowledges at least three roadblocks can stymie standardization efforts:
· “Overcoming the fear that standardization will stifle flexibility and innovation. While it is true that standardization is chiefly intended to reduce variation, it has at its core the expectation of ongoing improvement and evolution of best practices.
· “Recognizing that ‘similarization’, e.g., a mirrored layout of a repetitive room versus an identical layout, is not standardization. True standardization sets a definitive specification and utilizes metrics to measure adherence to the expected performance or condition. Allowing the ‘similar’ introduces an unacceptable level of variation and process confusion.
· “Embracing a framework through which standardization is defined. Developing standards through consensus requires a facilitated scientific approach and the participation of a multi-disciplinary team of key stakeholders. It requires time and resources to be dedicated to accomplishing clear objectives.”
The lack of standardization may lead to ineffective processes, unexpected outcomes, poor quality, diminished safety, and increased cost, Wallen insists. But the benefits of standardization extend far beyond mitigating these consequences by providing advantages that bolster organizational performance. Wallen anticipates that standardization will serve to:
· “Define the ‘normal’ and establish a guide or reference to allow variations in process or conditions to be quickly identified and remedied.
· “Reduce compliance risk associated with human factors by making the right work easier to do and the wrong thing difficult to choose.
· “Reflect best practice targets and set expectations for performance metrics and ongoing improvement.
· “Decrease staff /employee fatigue by removing workplace confusion and replacing it with activities that are well defined, intuitive, and predictable.
· “Promote high reliability by replacing less efficient and effective informal methods with thoughtfully designed and consensus driven guidelines.”
Aesthetic difference
Delineating specialties in a cross-functional, multipurpose room has benefits, too, experts say. “Building specialized multipurpose rooms to have distinct and unique specializations is a smart strategy that benefits patients, positively influences a facility’s bottom line and boosts the facility’s overall reputation in the community,” Kurz encouraged.
But she contends that several caveats must be addressed. “It is important that every room design caters to the planned procedure mix that will be executed in that room,” Kurz noted. “In other words, each room design must be tailored to the client’s unique needs, particularly for any unique procedures that are more complex or rare.
“Each room design should be evaluated for its ability to switch rooms at any time, with built-in adjustments that allow the room to be transitioned for specific disciplines that require a unique setup,” she continued. “From the start, room design must be forward-thinking and accommodate future needs. If a clinical specialty is in the long-term plan, the room design must account for it. Naturally, a surgical room won’t be equipped like an [interventional radiology] room. The needs are vastly different, and the room design should match the need.
“Infection control can’t be overlooked,” Kurz insisted. “Surgical rooms demand special planning considerations to secure a sterile environment. Think about floor and ceiling construction, boom use for overhead displays, shields, OR lamps and laminar airflow.”
Fitzgerald further illuminates the footprint demands for cross-functional, multipurpose rooms. “Multipurpose rooms must be designed and planned with higher ceilings, large doors, larger and open floorplan, outlets, lighting and ceiling-mounted monitors to accommodate different uses,” she noted. “This can result in added costs. Specialty rooms, meanwhile, only have the product they need.”
Redding agrees. “The clinical requirements for an exam room versus a surgical suite are vastly different and the sheer size of equipment to support surgeries are prohibitive and non-functional in a smaller footprint,” he said. “Additionally, it is imperative to understand the number of resources that will be interacting with the patient throughout their patient encounter. In some areas like surgery, the number of resources is significant and space mobility is key to providing a safe and workable environment. I do believe there are plenty of opportunities to standardize room size and configuration for a similar clinical setting. Creating a standard room size and configuration across the clinical settings may be prohibitive clinically, financially, and operationally.”
Timmerman recognizes the motivations for uniform room configurations. “There may be a very good reason to configure rooms differently depending on the purpose of the room,” she said. “The requirements of an exam room are different than the requirements of the procedure room. The important design element is to standardize the workflows so that the needed supplies and equipment are available at the point of care and there is flexibility built in to allow for elements such as consultations or telehealth.”
Wallen understands the decision challenges, too. “Design variation must be minimized,” he noted. “However, it may be required in some cases. For example, depending on the procedure or treatment, a particular multi-functional room may require different equipment and supply set-up. To maximize utilization of the space, a support room for staging and exchanging equipment and supplies should be immediately adjacent to the procedure/treatment room.”
Horn encourages healthcare organizations to be practical. “Some specialties make sense to combine, like surgery and imaging for example, as the rooms often require significant square footage,” he said. “Alternatively, exam, treatment and lab service combined spaces provide a one-stop-shop model for patients improving patient outcomes and satisfaction.”
Vendor consolidation
Once a healthcare organization chooses to design cross-functional, multipurpose room, whether each looks similar or distinct, the next decision centers on the necessary equipment and supplies and whether that gear should be acquired from a single vendor or multiple vendors. Think standardization versus specialization.
Much depends on contracting agreements and negotiations. “The benefits of designing and outfitting a multipurpose room with a single vendor outweigh the drawbacks in measurable ways,” Kurz indicated. “Of course, health facilities must carefully consider their specific needs, negotiate favorable terms and actively manage the vendor relationship to ensure seamless implementation. For Siemens Healthineers, the imperative is to engage in each project as a partner invested in the facility’s success.
“The single-vendor option lets facilities leverage economies-of-scale cost savings at the point of sale. And it simplifies procurement,” she continued. “Instead of dealing with multiple vendors, facilities can negotiate a single and comprehensive contract. This saves time and resources, and it makes acquisition of equipment more efficient. With one vendor, hospitals can be certain that equipment and systems are seamlessly integrated and compatible. The result: Less downtime and better overall system reliability in the room. There is consistency between systems and consistency in the room design. And in addition to enhancing aesthetic appeal, this consistency ensures the layout is optimal for workflow efficiency and infection control. And regarding service, support, and troubleshooting, a single vendor option means a single point of contact, so operational concerns are easier to manage.”
Timmerman highlights the single vendor versus multiple vendor options as well. “There are certainly challenges that go along with vendor selection and management,” she said. “There are pros and cons to having multiple vendors, and there are pros and cons to having a single vendor. A single vendor may be easier to manage, but there may be concerns with continuity of supply. Having multiple vendors can be difficult to manage, but the supply chain may have less risk. Therefore, it’s likely that the vendor strategy may change based on the criticality of the equipment being sourced.
“Ultimately, vendors need to partner with their customers throughout the entire design journey. Ideally, a partner for critical solutions will have the expertise to help develop design solutions that are rooted in research to help achieve the desired goals and improved outcomes. They should have the knowledge and expertise that starts with the design process, through installation, and all the way through servicing the solution,” she concluded.
“Generally, multiple vendors can complement one another based on their respective offerings,” Horn assured. “Assuming each vendor is respectful of their competition, the space, patient and end user can all benefit from the various capabilities of a variety of vendors.”
There is one way to supersede the single-versus-multiple quandary, according to Fitzgerald, that hinges on information technology. “The design doesn’t need to involve a single vendor, but the equipment needs to be interoperable,” she insisted. “That way you can wheel in what you need and plug it in, not only into the electricity but also into the care delivery system, such as monitors, image capture, smoke evacuation, gasses, etc.”
How do you equip a cross-functional, multipurpose room?
If a healthcare organization wanted to convert or set up an existing room as a multipurpose room, what are some of the key pieces of equipment and furniture – mobile or stationary – that should be included, depending on which specialties it wanted to incorporate (e.g., medical exam, treatment, imaging, laboratory, surgery)? Five executives from leading equipment, furniture and service companies share their recommendations with Healthcare Purchasing News.
“Once you have a workflow design that allows for flexibility, there are some key equipment solutions that might build in additional flexibility.
“Mobile treatment cabinets and procedure carts can be used to assist in supply access and storage within the exam room, as well as serve as an additional work surface positioned left or right of the caregiver. They also allow for sturdy room-to-room maneuverability and can be customized for specific workflows and procedures, offering an optimal platform for supporting the delivery of care and making the most of available space.
“Mobile workstations are designed to strengthen patient-caregiver interaction by supporting a seamless experience at the point of care. Mobile workstations allow clinicians to make the most of their space while maintaining their focus on the patient. They can also be easily moved from room to room or within the room.”
Tracy Timmerman, senior marketing manager, Midmark
“Building or converting a multipurpose room requires careful planning and consideration of the specialties the facility plans to incorporate. Room conversions often come with tight room constraints, so prioritizing how the available space is allocated is important.
According to Kurz, key equipment and furniture that should be used includes:
• Imaging system(s)
• A table system that caters to the planned procedure mix, with adjustable height and patient positioning capabilities
• Shielding (ceiling mounted, table mounted, mobile)
• Lights
• Ceiling supply units (gases, surgical, monitor)
• Machines: Heart lung machine, endo, microscope, ablation
• Carts and tables: Anesthesia, instruments, trash
• Injector
• Working station for running nurse
• Cabinets for drapes, needles, tubes
• Wall monitors
• Laboratory equipment: lab benches, microscopes, centrifuges, storage for reagents and samples.
• Exam room furniture: Chairs, workspace, seating for patients/family members
Felicia Kurz, senior vice president, Advanced Therapies, Siemens Healthineers North America
“For exam/treatment/inpatient rooms, consideration should be given to facilities for a ventilator, electrical/medical gas services, continuous patient monitoring and air pressure relationships to adjacent spaces (i.e., negative pressure rooms in the case of COVID).”
David Horn, AIA, ACHA, director, Corporate Project Development, Surgical Solutions, STERIS
“Handwashing accommodations, flexible lighting levels, standardized location and availability of documentation technology, supply carts for unique set up and vitals/assessment tools.”
Thomas Wallen, AIA, principal, Vizient
“As health systems explore how best to leverage multi-disciplinary rooms, the focus will be on mobility of equipment to enable changes in the delivery of patient care. This includes sizing the room to accommodate larger equipment, including door size and access to the room from a corridor. The room should be ‘plug-and-play’ to reduce the need to rearrange the room leading to additional inefficiencies.”
Tom Redding, senior managing director, Healthcare, St. Onge
Pairing up procedural specialties: Which makes the most sense and why?
When a healthcare organization looks to convert or set up an existing room for cross-functionality or multipurpose use, the clinicians and administrators have to determine how to choose the optimal procedures to combine – medical exam, treatment, surgical, diagnostic imaging, interventional radiology and laboratory are key options – and then focus on equipment and product contract negotiations. But what might be the procedural specialties that are the easiest to pair up versus the most challenging? Four executives from leading equipment, furniture and service companies shared their combinations.
“The answer may seem obvious, but the easiest and most practical multipurpose room combinations involve the integration of modalities that share similar medical equipment, infrastructure and operational requirements. Success is more easily achieved when you have one discipline and one team working in the room.
“The imaging suite is a good example. X-ray and fluoroscopy machines share similar technology and room requirements. By combining these modalities into a multipurpose room, hospitals can easily reduce physical space and more efficiently deploy resources.
“Another simple combination is the medical exam and treatment room. The modalities share core equipment and supplies. The patient who can seamlessly transition from exam to treatment eliminates a follow-up visit and doesn’t need another room.
“Conversely, finding synergy between divergent modalities is difficult. The challenge lies in the different infrastructure, equipment, and operational requirements between the modalities under consideration. Combining multiple interests and disciplines is not easy; it gets harder with each new imaging system or hygiene level you want to combine.
“Imagine the challenges of building a room that combines medical exams and surgery. The exam room requires a quiet environment for consultation. Surgical rooms demand strict sterilization, special equipment, and space. Building that room will be a challenge because it lacks commonality.
“These complexities can be overcome, but only with meticulous planning that emphasizes effective workflow design and equipment compatibility. The ability to adapt to changing dynamics in the healthcare market – pandemics, demographic shifts, evolving treatment modalities, and more – is a fair measure of a facility’s ability to meet the needs of its community.
“Multipurpose room design has emerged as a viable approach to maximize clinical, financial, and operational efficiency. Embracing the trend gives health facilities a new tool in their delivery of quality care. For many, it’s an empowering cornerstone to continued flexibility and sustainability. Embracing this design philosophy is not just an operational choice; it's a commitment to the future of healthcare delivery.”
Felicia Kurz, senior vice president, Advanced Therapies, Siemens Healthineers North America
“From my perspective, the less specialized, the easier to build in multipurpose use and flexibility. The exam room can be easily designed to include a zone for the exam, a consultation space, and options for telehealth.
“Areas such as surgical, interventional radiology, or diagnostic imaging have very specific purposes. Therefore, those spaces are likely to present more challenges to build in multipurpose use simply due to the nature of the work being performed.”
Tracy Timmerman, senior marketing manager, Midmark
“Creating multidisciplinary rooms have many benefits to an organization but finding clinical commonality is key to the success of leveraging these types of rooms. Ideally, there are nature synergies when considering exam and treatment rooms. The rooms are typically similar sizes but with varying requirements for what ultimately will be utilized in each room. This includes varying supplies and equipment but through creative and innovative thinking there are opportunities to standard equipment and creating an ‘exchange model’ to enable interchangeability.
“There are plenty of opportunities to standard patient care rooms, but not all clinical care is created equal and allows for flexibility given the equipment requirements. The natural example where room standardization is not readily feasible is combining surgical and diagnostic imaging. For example, combining an MRI with a surgical suite will have immediate challenges because the MRI is fixed and requires significant room infrastructure and precautions to handle the magnetic field, and which will not allow for it to be easily moved out of the room to provide space to the surgical care. Additionally, many of the diagnostic imaging areas have expensive control rooms that aren’t necessary for surgical care leading to unnecessary capital expenditure and redundancy.”
Tom Redding, senior managing director, Healthcare, St. Onge
“Flexing a multipurpose room between functions is most easily achieved when the activities, or service performed, are simple rather than complex. An example is an exam room in a clinic, where the same room may be utilized for taking vitals, visiting with the provider, consulting with a dietician or educators, receiving therapy, scheduling follow-up appointments for diagnostics or procedures, and checking out. Flexing rooms where the activities are more complex (surgical suites), may require adapting the room with different mobile equipment, technology, or supplies. It is important to note that in all cases, creating flexibility and adaptability within the design will result in increased utilization. Where more complex activities are performed the cost of building and equipping the room is often higher and may yield a greater return on investment.”
Thomas Wallen, AIA, principal, Vizient
About the Author
Rick Dana Barlow
Senior Editor
Rick Dana Barlow is Senior Editor for Healthcare Purchasing News, an Endeavor Business Media publication. He can be reached at [email protected].