Ensuring safety in the surgical suite
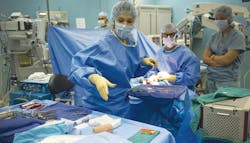
Operating Room
One of the greatest ironies of the operating room (OR) — where patients go for life-saving procedures — is its potential to also be one of the most dangerous, sometimes deadliest places inside a healthcare facility. Hazards of all types are waiting to happen to both patients and staff if proper safeguards aren’t always in place. For example, administering the wrong medication or dose, leaving foreign objects inside of patients, using faulty equipment, dirty equipment, missed recalls, needlestick and scalpel injuries, wrong site/patient/procedure errors, wearing the wrong PPE or not enough, accidental fires, surgical smokes inhalation … and that’s just the short list of what can go wrong.
Those and other complications are discussed continuously. Research is performed, articles and books are written, guidelines get updated, best practices are adopted, new technologies are developed, and clinicians try to do better.
What follows is a sampling of various solutions healthcare facilities can use to help prevent a variety of safety breaches. Healthcare Purchasing News asked these vendors two questions: How does your solution make a direct impact on improving OR safety and why is it a good investment for supply chain to consider?
First step: Follow the IFU
Following a manufacturer’s instructions for use (IFU) is a fundamental safety step and most OR and sterile processing technicians are dedicated to the process. However, significant obstacles can get in the way. IFUs can be difficult to understand. Lack of time needed to follow every step in the IFU is another challenge. Poor collaboration or understanding between the OR and sterile processing department regarding who is responsible for what can also throw a wrench into the process. Sometimes the IFU is missing entirely, especially when using loaners.
oneSOURCE offers healthcare facilities current IFU documents via subscription to a comprehensive database intended to simplify the IFU process, foster compliance, and maintain accreditation effortlessly. “The need for our databases is driven by CMS regulations mandating that healthcare SPD, OR, HTM and Infection Prevention departments follow the IFU for patient safety. We provide the necessary tools professionals and facilities need to avoid typical failures such as improper cleaning, wrapping or loading in the sterilizer; incorrect reassembly of the device; and use of an incorrect sterilization process,” said Heather Thomas, Chief Marketing Officer, Vice President of Sales and Marketing at oneSOURCE. “Improperly cleaned instruments and/or medical devices have been linked to adverse patient outcomes as well as death. When facilities have access to a robust tool like oneSOURCE it arms them with the resources required to keep patients safe 24/7 and can assist them in avoiding fees for readmission due to HAI lawsuits associated with fatal results in addition to expensive citations from accrediting bodies. We are launching databases for Facilities Maintenance and Tissue & Implants later this year to meet the patient safety compliance needs for OR and Facilities Maintenance departments.”
UDI & OR safety
UDI adoption remains challenging for most hospitals. In recent surveys by Healthcare Purchasing News, among the 43 percent of organizations stating they have not adopted the use of UDI in their supply chain data, respondents often cited there is “a lot of work involved and a lack of time to dedicate to the process.” While the importance is recognized, capturing UDI data has remained a significant hurdle for provider organizations.
SteriTrack’s Pat Cairn, COO and Michael Schiller, CMRP, VP, Healthcare Engagement, explained how SteriTrack UDI scanning solution delivers on patient safety, recall management, and regulatory compliance.
Everyone knows a recalled surgical instrument poses an immediate danger and should be removed from inventory but everyone knows also that it doesn’t always happen that way — not without a system in place that can assist with the myriad challenges of staying on top of the many surgical products that could lead to injury and death.
“The Tractus platform allows a clinician to specify anatomic regions involved in a procedure and the ability to document the exact location of each implant. Once scanned, UDI data resides within the patient’s clinical record where the patient can be correctly notified in the future if a recall occurs,” Schiller added. “This capability provides the most accurate and effective UDI documentation process and, is critical in eliminating potential data entry errors that could occur when manually entering the UDI information. Almost as important as notifying a patient of a recall is avoiding an inaccurate recall notification, as a result of UDI data being entered incorrectly. Tractus scanning technology eliminates risks of documentation errors resulting from manual data entry, which are reported at an average error rate of 30 percent.
“Data capture of the UDI still hasn’t been widely adopted by hospitals. It would offer many patient safety advantages such as in the event of product recall and enhance the acuracy of patient records regarding the products used on them,” continued Schiller.
“While minimal regulation exists today to propel providers to capture UDI data, there is tremendous benefit recognized in recording the UDI data for implants and supplies used during the course of a procedure, building a comprehensive patient clinical record within the EHR and moving healthcare organizations closer toward understanding the total cost of care, improving patient care and patient outcomes.”
Sharps
Sharps safety has been a top priority for decades and it’s paid off in many ways with better practices and technologies to support it. But it remains slow-going in some areas, and according to the Centers for Disease Control, approximately 385,000 needlesticks and other sharps-related injuries happen to hospital-based healthcare personnel each year.
“Since the Needlestick Safety and Prevention Act was signed into law in November 2006, sharps injuries in nonsurgical settings dropped by almost a third, while injuries increased by 6.5 percent in surgical settings,” said Adeline Yi, Senior Manager, New Business Development, Medipurpose. “ORs face even greater risks than other departments, with the potential for scalpels to cause deeper and more serious wounds. Yet nationwide, the conversion to safety scalpels has been very slow as surgeons and surgical techs are unhappy with the limited safety scalpel options currently out in the market. During the development of our Anzen Safety Scalpel, we worked closely with surgeons and surgical techs to design a product to meet those needs: Reusable, metal-handle that provides surgeons with the weight, balance, and feel they are used to in a traditional scalpel; pushing on the slider moves the blade in a out of the cartridge (intuitive to use, like a box cutter); safety catch that prevents the blade from being extended when the cartridge is not mounted on the handle (prevents accidental sharps injuries during loading of the blade); and cartridge lock feature that prevents cartridge from being removed when blade is not fully retracted (prevents accidental sharps injuries during unloading of the blade).
Added protection
Adding to the sharps safety effort are surgical glove technologies that not only protect transmission of pathogens from hands to patient but will protect surgeons from injuries.
“Surgical glove protection is a primary factor that works to prevent sharps injuries, minimize risks associated with latex allergies and surgical site infections (SSIs),” said Judith Seltzer MS BSN RN CNOR, Clinical Director, National Accounts, U.S. Surgical Division, Mölnlycke Health Care. “Double-gloving is proven to reduce risks of sharps injuries and exposure to bloodborne infections by 71 percent. Data research reveals that on average, only 10 percent of glove punctures are noticed during surgery. At least 60 different bloodborne pathogens can be transmitted to healthcare workers due to accidental exposures with HIV, Hep B and Hep C accounting for most of the risk.
Smoke & fire
The Association of periOperative Registered Nurses (AORN) has done much work in recent years to raise awareness of the health and safety problems associated with surgical smoke inhalation. And some states are now passing laws requiring hospitals and surgical centers to implement strategies for reducing exposure, which makes sense. The National Institute for Occupational Safety (NIOSH) says surgical smoke contains toxic gases, vapors and particulates, viable and non-viable cellular material, viruses, and bacteria — all of which can cause a host of health problems, including asthma.
“This all-in-one design enables healthcare facilities to stock all needed sizes and styles in each room without having to make any investment in depreciable capital equipment that often costs many thousands of dollars,” Swift continued. “Additionally, healthcare facilities continue to transition to fully disposable systems to reduce cross contamination risks and mitigate the severe financial consequences associated with treating HAI’s. ONETRAC LX is the logical next step in this effort.”
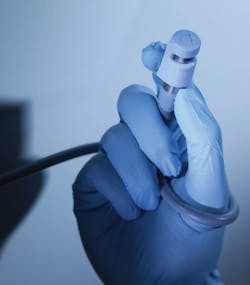
“The GloShield safety cap provides a protective covering for the end of the fiber optic light cable that can reach over 550 degrees Fahrenheit,” explained James K. Rains, PE, CEO, Jackson Medical. “GloShield is designed to prevent Never Events such as OR fires from occurring. This award-winning product is reliable and intuitive, making the hospital safer for patients and staff. GloShield is a simple way to mitigate the risk of ‘never events’ from occurring in the operating room. Of over one hundred first-time users, 94 percent thought that GloShield offers reliable protection and would reduce the risk of fires.”
Keeping tools safe & secure
Workflow interruptions cause stress and stress can lead to mistakes. For example, dropping an instrument on the floor — happens all the time — which leaves surgical teams scrambling for a replacement. Passing needles, electrocautery devices and other potentially hazardous equipment can also lead to cuts, burns and more. Alas, there is a solution.
“Based on firsthand experience, DropStop was designed by the OR Innovations team to solve a common problem facing surgical teams world-wide; costly surgical tools falling off the surgical field, leaving the circulator scurrying to get a replacement, if one is available!” said Alex Duy Bui, Chief Technical Officer, OR Innovations. “This event repeats itself daily in most surgical suites, resulting in hundreds of thousands of dollars annually of avoidable costs and unanticipated time delays. While the initial DropStop design goal was to prevent items from falling off the sterile field, DropStop also addresses other operating room challenges such as; securing the electrocautery holster in a safe, optimized position to minimize risk of patient burns, as well as positioning a suture pack on the user’s sleeve to eliminate risk of needle-sticks which can occur during passing of loaded needle drivers.
Retained surgical instruments
The horror of finding out that a foreign object was left inside of a surgical patient has lasting, far-reaching consequences for everyone involved. The patient, the surgical team, the facility suffers as a result of this “never event” which unfortunately is still too common. Implementing the latest technology is critical to reversing the trend.
“Currently in the United States the No. 1 reported surgical never event to the Joint Commission is retained surgical items (RSIs), of which the No. 1 contributor of RSIs is retained surgical sponges (RSSs) accounting for 69 percent of all RSIs,” said Jason Davies, Senior Brand Manager, Stryker. “[And] 16.3 percent of patients that have a sponge left in them suffer a permanent injury, and it is a mortal event for 4.5 percent of patients. The average malpractice impact to a hospital on a national average is nearly $600,000 per occurrence, and the rate of occurrence of RSSs is between 1:5,000 to 1:7,000 surgeries according to studies. The surgical team currently has a deficit of technology by only using a whiteboard & marker to keep counts on their sponges. It’s estimated that RSSs are left in patients 4,000 times a year in the U.S., or roughly 11 times a day. RSSs are a completely preventable surgical never event that add roughly $2.4B to the U.S. healthcare system
Opioid disposal
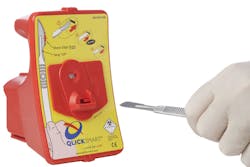
By now everyone is aware of the opioid crisis taking place in the U.S. and elsewhere. Concerted efforts are underway to help defeat the problem — patient advocacy groups, government, professional agencies, healthcare providers, insurers, pharmacist and medical supply manufacturers are all taking steps to help. Schreiner MediPharm’s contribution is providing a safer way to dispose of narcotic pain patches.
The Patch-Safe solution allows a broad use in different hospital settings, since it helps to safely and efficiently dispose of used patches, which is especially important in the hectic environment healthcare professionals have to cope with. Due to its special construction, it secures patches and critical substances reliably. In addition, it is easy and intuitive, which facilitates work in hospital and healthcare settings and helps to optimize processes.”
Editor's Note: There’s another safety issue that doesn’t get nearly the amount of attention or resolve, yet is as unsafe and scary as any other OR hazard – nurses and surgeons with substance use disorders, including those who engage in drug diversion (stealing controlled substances reserved for patients). Read more here.
About the Author

Valerie J. Dimond
Managing Editor
Valerie J. Dimond was previously Managing Editor of Healthcare Purchasing News.