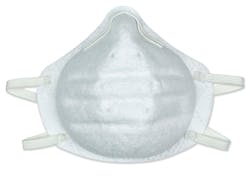
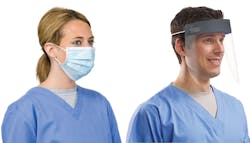
COVID-19 disease, caused by the SARS-CoV-2 virus, has transformed the healthcare supply chain, population health and patient care as we knew it. Infections first struck people in China, then popped up in other countries across the world.
The United States reported its first case in December 2019. Many months passed and infections surged on. This public health emergency-turned pandemic propelled an upheaval in the production of personal protective equipment (PPE) critically needed for staff in hospitals and healthcare facilities to adequately and safely care for patients.
“As has been well reported in HPN and elsewhere, when the COVID-19 pandemic hit, it placed terrific pressure on the supply of PPE, particularly face coverings and gowns,” emphasized Ralph Basile, Vice President of Marketing & Regulatory Affairs, Healthmark Industries Company, Inc. and a Sub-chair of ASTM International committees. “The first indicators of this came in January, when Chinese companies were contacting distributors of PPE outside of China, as there was inadequate supply in China. As time moved along and the virus spread across the globe, supply shortages of PPE were experienced by market after market, country after country. Come March, when the virus became widespread in the United States, this country experienced these shortages.”
Pandemic changes
Basile shared his insights on the trajectory of PPE development this year, ahead of the September 9-10, 2020, ASTM International virtual Workshop on Fast-Tracking Standards Development to address Personal Protective Equipment (PPE) Shortages Due to the COVID-19 Pandemic.1
“Attempts to adapt to the shortage of N95 masks have included efforts to reprocess and reuse these masks that are labeled for single-use and also to acquire alternative masks that have not undergone regulatory review and clearance,” Basile noted.
“Changes have included expanded recommendations/mandates requiring the wearing of face coverings in public places and new entities manufacturing these coverings,” he continued. “Many of these face coverings have limited or have no filtering properties, so they could prove useful for healthcare workers with duties that did not put them at the highest risk of being exposed to COVID-19. During this time, many organizations that had never made masks, face shields, or gowns pivoted and turned their resources to make such PPE. This included existing cut and sew shops, material convertors, 3D production facilities and other such organizations.”
The ASTM International committees aim to meet and “identify the needs and opportunities to either modify existing ASTM standards or to author new ones, to help the industry, regulators and healthcare professionals, based upon the experiences in responding to the COVID-19 pandemic, better prepare and respond to the existing PPE challenges and future ones, should we be faced with a challenge like this again,” Basile explained.
Expanded production
The resourcefulness and ramp-up of PPE remain an ongoing priority for supporting the health and protection of healthcare workers and patients. What are the latest developments in PPE manufacturing and distribution in the healthcare landscape?
Recent examples include:
Dräger opened a new production facility in Montgomeryville, PA, that will manufacture and distribute N95 respiratory protection masks announced the company in a press release.2 “The facility will have three employee shifts throughout the day, operating 24/7 to ensure the mass production and supply of National Institute of Occupational Safety and Health (NIOSH)-approved N95 respiratory protection masks to frontline workers. Additionally, the facility will support Dräger’s recently announced contract with the U.S. Department of Health and Human Services to produce N95 masks in the fight against COVID-19,” the release stated.Disposables versus reusables
As new PPE is produced, many in the industry weigh the pros and cons of items that can be disposed of or can be repurposed after disinfection. How do these PPE items rank in value, effectiveness, comfort and safety for healthcare staff?
“The recent unprecedented demand for PPE has made clear that sole reliance on single-use products is an ineffective supply strategy,” Stewart stressed. “Reusable PPE offers significant advantages with respect to continuous and manageable availability, proven performance, lower cost-per-use, and, in the case of apparel, a documented preference by end users with respect to comfort.”
Pearsall further points to the benefits and challenges of disposable and reusable respirators and face masks.
“PPE, such as disposable N95 respirators and face masks, which are intended to be used one time and discarded after every patient encounter, were designed to be easy to use, save time, improve productivity, and reduce risk of contact transfer of pathogens,” she indicated. “Reusable PPE, for example, elastomeric facepiece respirators or PAPRs, can be an alternative and offer benefits, including easier breathing and potentially higher filtration efficiency depending on the filter selected. Reusables require decontamination after each use. This adds an additional step for reprocessing into the workflow. In addition, they cannot be used in all clinical areas.”
Imms suggests that function, size, fit and accessibility matter with reusable equipment.
“Reusable devices have considerations for cleaning and reprocessing,” he noted. “Looking for simple and compact devices that minimize the time and effort for staff are important to implementation and ongoing care. It is important to consider that disposable N95 masks must be fitted correctly to be effective. One major risk for users and employers after fit testing, is that if the hospital cannot source the correct brands on an ongoing basis, staff will not have access to their mask type without retesting. With positive pressure reusable respirators, there are no ongoing issues with stock or model availability – your wearers always have access to reliable, high-level protection.”
Another consideration is the choice between disposable or reusable clothing, notes Zediker.
“There have been several articles written that illustrate the risks associated with home-laundered scrubs and the resilience of pathogens,” Zediker said. “Specifically, a study done in the Journal of Hospital Infection by Tammelin concluded that disposable, polypropylene scrubs are more effective in reducing airborne bacterial counts when compared to reusable options.”3
VanHee urges that all guidelines be followed when cleaning or disinfecting any reusable items.
“Cleaning and disinfection of reusable PPE (or single-use PPE in emergency situations) is a vitally important, but often underappreciated component of PPE use,” he explained. “Although best practices dictate that single-use PPE should never be reused, supply shortages have required significant adaptation of PPE reuse practices. No matter the type or PPE, strict adherence to cleaning and disinfection protocols that have been validated by the PPE manufacturer and/or the manufacturer of the disinfection equipment is fundamental to the safe reuse of PPE. It is of particular importance to stay up-to-date on FDA emergency use authorization (EUA) for any approved disinfection protocols being used for single-use PPE.”
Planning and preparation
In light of this pandemic, it is clear that hospitals and healthcare providers must be vigilant in their pursuit of PPE to ensure the safety of staff and patients. What are the best practices for existing and future PPE evaluation, sourcing and other decision making and planning?
Planning:
Pearsall brings forth the need for effective knowledge and tools for supply chain decisions and implementation.
“A best practice for planning PPE supply needs is to understand changing protocols and how that drives utilization changes and product selection all the way down to the SKU level,” she expressed. “While much of our pandemic preparedness has historically been centered around the expectation of a flu pandemic, we’ve learned that the threat also exists from other viruses with different, potentially unknown modes of transmission. Healthcare providers need greatly improved tools for the complex challenge of planning, sourcing, procuring and stocking the proper PPE with the appropriate levels of protection for whatever the threat may be. This is a tremendous need that supply chain technology could help with in the future.”
All plausible constituents should be integrated into planning, explains Zediker.
“Do not forget about the ancillary population(s) (salespeople, contractors, consultants, etc.) that will need to be factored in,” he described. “Then look at channel partners that focus on these groups as a solution outlet. For example, RepScrubs is solely focused on the extensive visiting vendor population. We can support planning efforts by eliminating the cost and quantity requirements that a hospital has for that population. We do this by taking on the workload and inventory and shifting the cost of providing those products to visiting sales professionals.”
Past planning should guide the planning for future emergency events and needs, says VanHee.
“The COVID-19 pandemic has proven that contingency planning for emergencies is of utmost importance,” he stated. “The real challenge is to balance the worst-case inventory scenario with appropriate budgeting and inventory holding costs. When modeling and testing inventory planning protocols, historical information and references should be used to develop the model and evaluate the impact.”
Evaluation:
With PPE at the forefront of the pandemic, care and safety, it should be scrutinized closely, urges VanHee.
“Historically, PPE may not have required high-level product evaluation, but it has become increasingly important to have an effective product evaluation process in place for PPE,” he expressed. “PPE evaluation should consist not only of the characteristics of the products, but also the characteristics of the manufacturer. Evaluation of the manufacturer should ensure both product quality and appropriate quality systems that meet ISO standards for the manufacture and distribution of healthcare products.”
Stewart recommends making evaluations according to suppliers’ length of time in the market and connection to the healthcare-specific industry.
“Evaluation of PPE should be based upon not only the documented performance of the products, but also the track record and credibility of the supplier,” he said. “To the extent possible, healthcare organizations should endeavor to source products from suppliers with longstanding and reliable records of manufacture, distribution, and sale of the specific PPE to the institutional healthcare marketplace.”
Zediker suggests checking out what’s new in the market and adhering to guidelines.
“I would always recommend examining new technologies, ensuring cost effectiveness, cleanliness, and efficiency,” he indicated. “Also, many Risk or Infection Prevention departments have specific protocols that they require team members to follow. I would recommend knowing and following those guidelines.”
Sourcing:
Supply should be sourced from manufacturers who are reliable, authentic and regulated, sums up VanHee.
“The COVID-19 pandemic has highlighted the need for reliable and compliant sourcing for not only PPE, but for healthcare products in general,” he shared. “Recently, issues with counterfeit facemasks, respirators, and other PPE have been brought to the attention of the general public, but this is not a new problem.”
Zediker emphasizes sourcing should be based on timespan and diversity of manufacturing.
“Look for longevity (five years or more) of suppliers,” he noted. “Look for folks who were delivering value prior to the panic. Ask for samples of everything you buy. If you can’t wait for your current supplier, then you need someone who has a relentless focus on worldwide sourcing.”
Manufacturing safety and product support also can be helpful with sourcing, according to Imms.
“For reliability on quality and approvals, hospitals should be sourcing from manufacturers that have a track record in workplace safety, specifically, working within a healthcare setting, and can support with training and technical advice,” he said. This will save time and costs and build a relationship with the providers that will assist with supporting your team at the front lines.”
PPE Product Spotlights
References:
1. ASTML International: Workshop on Fast-Tracking Standards Development to Address Personal Protective Equipment (PPE) Shortages due to the COVID-19 Pandemic - VIRTUAL WORKSHOP: https://www.astm.org/SYMPOSIA/filtrexx40.cgi?+-P+MAINCOMM+F23+-P+EVENT_ID+4079+-P+MEETING_ID+147253+sympotherinfo.frm
2. Press Release No. 83 / August 24, 2020 Page 1 / 1: Dräger increases N95 respiratory mask production with new US facility: https://www.draeger.com/Library/Content/us-mask-facility-pr-83-en-us-final.pdf
3. Tammelin Study: https://pubmed.ncbi.nlm.nih.gov/23694760/
PPE projections for the next pandemic
How can healthcare providers, supply chain and logistics departments and manufacturers begin to prepare for the next major health crisis and PPE needs? Industry professionals shared their predictions with HPN.
“From our experience this year, we expect to see seismic shifts in a few areas: Telemedicine is having perhaps the fastest revolution in the history of healthcare. The very important role of infection control and infection preventionists is taking center stage, not just in acute care but across the spectrum of care. There will be more attention to the global supply chain for pharma manufacturing, but also for critical supplies, such as PPE. There will be a renewed focus on resilient supply chain and an appetite for adding near-shore manufacturing to a diversified manufacturing base. We many also see healthcare providers having closer scrutiny of the quality and performance standards for their PPE, with end users possibly even conducting their own testing to confirm compliance.
The next few years should hopefully usher in a new era of renewed innovation for PPE. A greater appreciation of the vital, irreplaceable role of PPE as a last line of defense should spur renewed investment in finding better solutions to protect our healthcare professionals and their patients. The last 20 years have seen little innovation in healthcare PPE, as there has been more emphasis on cost reduction. It’s been a while since we had significant advancements, like past inventions of electrostatic filtration media or fluid-resistant nonwoven gowns or nitrile gloves.”
Allison Pearsall, Honeywell Safety Products
“Many lessons can be derived from the experience of the past six months. Among these are the need to have in place a system of products that can be trusted for performance and a supply chain that assures a continuous stream of availability in the quantities necessary. We are of the opinion that recyclable, multi-use PPE provide the best options. Accordingly, preparation for future, similar demand surges requires the establishment of a system for processing reusable PPE products that is connected with a manufacturing/supply network that can scale upward as required to meet demand. Current ongoing advancements in material science, novel woven and knitted fabric structures, and fabric finishing technology will enable and inform the development of products that enhance market acceptance and preference for reusable PPE options.”
Richard Stewart, Standard Textile
“I believe we will see a diversification of manufacturing of goods across the board. The pandemic has highlighted an issue and the world is responding.”
Bryan Zediker, RepScrubs
“Long-term planning to include contingencies and redundancy are critical in the diversification of the supply chain. That should include pre-approval and pre-certification of facilities, such as Kitex, who have the ability to scale up quickly.”
Donnie Hodge, Kitex USA
“There have been a multitude of lessons learned in every aspect of preparedness; from how healthcare providers and facilities use and source PPE, to how manufacturers produce and distribute it. Many manufacturers learned the importance of flexibility in production capacity in 2020. The ability to ramp up production on critical items has been crucial to success in the COVID-19 pandemic. Manufacturers will need to continue to focus on identifying key product categories (PPE, disinfectant chemistries, etc.) that require more flexibility in production capacity.”
Brandon VanHee, Key Surgical LLC
About the Author

Ebony Smith
Ebony Smith was previously Managing Editor for Healthcare Purchasing News.