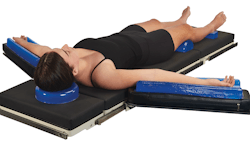
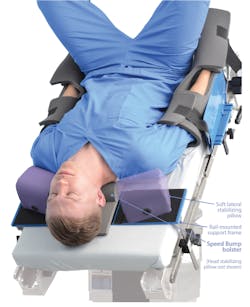
Keeping pressure off the patient
Repositioning a patient sometimes requires a shift of mere inches. But making sure a patient is repositioned frequently and precisely enough to prevent pressure injuries demands time, consistency, and a lot of physical strength on the part of nurses and other healthcare workers.
A patient may weigh several hundred pounds, yet be very fragile medically. And repositioning a patient, even one of average size, poses risks of injury to both patient and nurse.
Fortunately, there are options available. A wide spectrum of devices and small-to-medium tools can help adjust a patient’s weight to prevent pressure ulcers, or keep the body stationary while the patient is under anesthesia. Innovation in these medical products has continued to flourish through the COVID-19 pandemic. In 2020 the global patient positioning market was valued at $1 billion, and is expected to see modest growth over the next decade, according to a market research report by Fact.MR.
Given an increase in Intensive Care Unit (ICU) patients due to COVID-19-related hospitalizations, a national upward-trending Body Mass Index (BMI), pent-up demand for postponed surgeries, and many other moving parts to our healthcare picture and economy, the need for such innovation is clear.
“While many hospital-acquired conditions (HACs) have decreased, pressure injuries remain a stubborn exception,” says Michelle Daniels, Encompass Group Vice President of Product Strategy, Development and Administration.
An Agency for Healthcare Research and Quality (AHRQ) study from 2019, states that the rate of pressure injuries in 2017 was 23 for every 1,000 patient discharges.
The Joint Commission Center for Transforming Healthcare, reported in October 2020, a collaborative project to address hospital-acquired pressure injuries (HAPI) has resulted in more than a 60% reduction in a common but preventable issue that claims over 60,000 U.S. lives each year.3 The report also mentioned that AHRQ information estimated 2.5 million patients suffer from hospital-acquired infections each year.
Customized by technology
The prevention of pressure injuries has evolved in recent years and technology has led the way. Encompass recently announced the issuance of a patent for its Airisana Therapeutic Support Surface.
Airisana, Daniels says “does five therapies, all in one surface.”
The device was developed by a wound management advisory team made up of clinicians, Wound, Ostomy, and Continence (WOC) nurses, physical therapists, respiratory therapists and chief financial officers (CFOs).
The group set out three years ago to develop a device based on what patients and healthcare workers actually need, Daniels says, “not what the market was telling them they need.”
Airisana, according to promotional literature, uses, “pressure redistribution, alternating pressure, low air loss, immersion/envelopment and lateral rotation,” in order to adjust the placement of pressure against the patient’s body. It does this by way of an algorithm that randomizes patterns of pressure applied by the device.
A repeating pressure therapy pattern will stop working after a while, Daniels explains. Clinicians have found that a patient’s body, over time, will begin to adapt (involuntarily) to the pattern. Eventually, it fails to respond to the therapy.
The introduction of a random sequence, she says, is effective and unique.
“We really started this at the bedside,” she says. “We didn’t want to just create something that was the same as — but slightly different from —what already existed.”
Airisana is produced domestically, she said, and was designed specifically to be compatible with equipment made by other companies.
“Many surface systems require bed frame integration. With Airisana, you can use the current frame,” Daniels said. “We’re not trying to reinvent a hospital’s entire existing systems.
Weighty challenges
As the resident population in the U.S. continues to grow heavier, so, on average, do hospital and longer-term-care facility patients.
According to the Centers for Disease Control and Prevention (CDC), the prevalence of obesity in U.S. residents was 30.5% in the years 1999-2000 and had risen to 42.4% in 2017-2018. During the same span of time, the prevalence of severe obesity increased from 4.7% to 9.2%.4
Models and designs of many patient positioning devices have had to be created or adjusted accordingly.
Encompass, for instance, offers a bariatric patient option Airisana product with a weight capacity of up to 750 lbs, according to Daniels.
“Growing patient size means having to reposition more and more,” says Daniels. Airisana’s features help prevent staff injury. “It means three clinicians aren’t required to move a patient,” she said.
AliMed’s product portfolio of both reusable and disposable positioners includes some that are specially made to assist extra-heavy patients, including positioning straps for bariatric surgery, and a medical bariatric table-width extender.
Senior Product Manager Christian Baker says AliMed’s new AliBlue Gel positioners were designed, “to offer the same premium pressure relief as other comparable products on the market, while offering a more cost-competitive price point.”
AliBlue Gel Positioners are made of 100% polyurethane-based viscoelastic gel, aid in pressure redistribution and include an 18-month warranty against manufacturing defects.
Baker said the company has heard from a lot of happy customers about the gel line.
“They have been thrilled with the feel, along with the crisp clear blue appearance of the positioners and have appreciated that AliMed has these in stock during a time of increased supply disruptions,” he said.
A lighter alternative, AliLite Positioners, are up to 50% lighter than comparable gel-only positioners, according to the company’s website. The hybrid material in those products are easier to carry and maneuver, a feature that helps prevent staff injuries.
“These are aimed, Baker said, “at helping healthcare facilities decrease their overall spend on surgical procedure supplies.”
COVID impact
The respiratory distress suffered by COVID-19 patients has placed a new spotlight on the use of prone positioning and small positioning readjustments to prevent pooling of lung secretions, and encourage circulation.
“Pulmonary hygiene,” says Daniels of Encompass Group, “is a very hot topic right now.”
Katherine Gunn, Senior Director of Clinical Operations at Wellsense, has found this to be the case, as well.
“COVID-19 exposed and highlighted the biggest gap in the pressure injury prevention spectrum— the inability to see pressure,” said Gunn. That guesswork, she says, made the business of treating hospitalized COVID-19 patients harder.
“Hospitals were contacting us for a solution because their prone patients were acquiring pressure injuries,” she said. “Proning became a critical adjuvant therapy for improving ventilation in COVID patients.”
“Proning already increases the risk of acquiring a pressure injury by greater than 29%, and these patients were often in this position for longer than Q2,” Gunn said. “Many staff members were not familiar with placing patients in this position.”
The Wellsense solution was an advanced pressure visualization system called VŪ.
“With the VŪ, caregivers can see the effect that head-of-bed (HOB) and foot-of-bed (FOB) adjustments have on pressure and they can adjust inflation settings based on what is appropriate for each patient,” Gunn said.
The device provides visual feedback on the effectiveness — or ineffectiveness — of the pressure-reducing interventions being employed, she explained. A healthcare provider (HCP) can see, for instance, “when a pillow is appropriate for offloading or when a wedge is required.”
“Once the VŪ was implemented, there was no guessing where the high pressure was located or wondering if positioning devices were correctly placed,” Gunn said. “Staff could leave the bedside, confident in their actions, knowing the patient was in a position of low pressure. They could continuously monitor this pressure from outside the room and conserve PPE, as well.”
Historical pressure reports also are available for each VŪ patient, which facilities use, Gunn says, “for education, goal setting and root cause analysis.”
Patients too can access the information, which can improve health outcomes and reduce costs.
“PI reductions achieved with our customers during COVID-19, with the highest-risk patients is a testament to the necessity of pressure visualization in the PI prevention spectrum,” Gunn said.
Secured for surgery
During surgery, even healthy patients are at risk for pressure injuries and falls.
Dan Allen, founder of D.A. Surgical, has made it his business to track emerging trends in surgery, and create products for those surgeries. Most devices the medical products entrepreneur creates are meant to keep anesthetized patients safely positioned on the surgical table, even when placed at a steep angle.
Perhaps best known as creator of the surgical stirrup that bears his name and for a boot-style stirrup now ubiquitous in operating rooms, anatomy and gravity, he says, are two intractable realities that drive most of his work.
Early in his 40-plus years of observing surgery, Allen says he saw just how vulnerable surgery patients are when they are under sedation.
If not well-secured, he says, “They could slide off the (surgery) table and suffer horrible injuries.”
Sliding, Allen says, is the primary problem his inventions are designed to prevent.
“Sliding should be a ‘never’ event,” Allen said.
Allen’s chief interest these days is in positioning products related to robotic-assisted laparascopy procedures.
“The unique technology used by the surgical robot creates unintended consequences in regard to patient positioning,” according to D.A. Surgical.
Another of the products in the series protects a patient’s face from swinging robotic arms.
In addition to potentially being struck in the face, there is risk of a “meat hook” restraint.
“When patients slide even ‘just a little bit,’ while in Trendelenburg position, it is the (fixed) trocars that end up restraining the patient on the table,” Allen says.
“Fixed robotic trocars,” his website warns, “create a serious potential for patient risk as it can cause incisional tear, post-operative hernia formation, and increased post-operative pain secondary to over-stretching of the anterior abdominal wall.”
Along with these restraints Allen has developed numerous disposable foam pillows to keep every part of the patient’s body positioned safely for surgery.
Some call Allen’s products “innovative,” or “inventive,” but Allen takes more of a tinkerers view.“ I make lots of little problem solvers,” he says.