Minimizing infection by maximizing skin and wound care
The COVID-19 pandemic has exacerbated the challenges of skin and wound care as the virus has added a significant new burden to clinical staff members. Guidance from the U.S. Centers for Disease Control and Prevention (CDC)1, other regulatory bodies and industry associations on the risks of spreading SARS-CoV-2 between people elevated hand hygiene practices as a top priority.
At the same time, clinical teams still struggle with the fight against surgical site infections (SSI) and hospital acquired infections (HAI), some of which have increased during the pandemic.2 Wound care has also remained a high priority as clinicians care for bedridden “long hauler” COVID-19 patients who run the risk for pressure injuries.
Medical supply, equipment and solution manufacturers have responded with a broad array of products to address the needs of clinicians as they struggle to manage the workload of caring for both individuals with COVID and non-virus patients.
Sustainable sanitizer
The COVID-19 pandemic has made everyone realize the importance of sustaining good hygiene practices, from healthcare providers to consumers. Hand sanitizer sales in the U.S. rose more than 620% in 20203, as individuals and organizations strived to stem the spread of SARS-CoV-2 infections. As use of these products skyrockets, the question arises - what impact are they having on users and the environment?
“As the world reopens after the COVID-19 pandemic, it is important that people have access to a hand sanitizer that they can trust to protect them against germs without the use of any toxic chemicals,” said Deborah Chung, North America Marketing Manager, Healthcare – Professional Hygiene, Essity. “The Tork Alcohol Gel Hand Sanitizer is an efficient and sustainable solution to promote hand hygiene. It comes in a variety of formats, such as pump bottles and in a dispenser/refill system. These can be mounted on a wall or used with a stand, providing greater access to proper hygiene.”
This product is also one of the first two hand sanitizers in the market to receive a Green Seal certification. Green Seal, a non-profit authority on safer and more sustainable products, tested the product formula for carcinogens, reproductive toxins, skin irritants, phthalates, parabens and contaminants. To receive a Green Seal certification, a product must also meet uncompromising performance standards, use ingredients that do not pollute waterways and use eco-friendly packaging materials.
“This recognition not only proves our ongoing commitment to hygiene but also to more sustainable solutions,” Chung added.
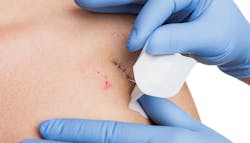
Protecting IV catheter sites
The skin acts as a protective barrier against foreign organisms. Therefore, when the skin is bypassed during central venous catheter (CVC) or peripherally inserted central catheter (PICC) insertion into a blood vessel, there is a risk for systemic infection.5
PrevahexCHX is the first and only pure chlorhexidine dressing cleared by the FDA with complete antimicrobial protection throughout the transparent areas of the dressing. PrevahexCHX contains no acids, salts or binders, which allows it to activate on contact with the patient’s skin providing site protection on day one through day seven. PrevahexCHX provides rapid efficacy against multi-drug resistant organisms both underneath and several millimeters beyond the perimeter of the window.
Increased demand for wound care
According to the U.S. National Institutes of Health, chronic wounds or wounds that are slow to heal, affect 6.5 million people in the U.S.6 As Annette Brüls, CEO, Medela, describes, there are many factors that are increasing the demand for wound care – from an aging population with chronic conditions to the COVID-19 pandemic.
“The demand for advanced wound care is anticipated to increase due to the rise in the geriatric population and the incidence of diabetes, obesity and chronic conditions, particularly in disadvantaged populations affected by COVID-19,” explained Brüls. “However, many trends that emerged in 2020 offer promise. We expect to see more advancements in digital tools, such as telehealth and educational apps, and increased efforts to ensure coordination of care across settings. Hospital leaders will select industry partners based on their ability not only to assist them in controlling costs, but also to deliver a better patient experience, improved outcomes and greater operational efficiency.”
Clinicians face significant challenges in preventing wounds, most notably pressure injuries, when caring for critically ill COVID patients, according to the National Pressure Injury Advisory Panel (NPIAP). In its recent position paper, NPIAP describes how clinicians struggle to adhere with the standard care protocol of turning critically ill patients from side-to-side when the patients are suffering from respiratory distress:
“For the COVID-19 patient with acute respiratory distress syndrome, prone positioning is often used for many hours and/or days and ‘turning’ is limited to microshifts and changing the position of the head, arms and upper body according to ‘swimmer position’ protocols. In certain situations, it is not only challenging but sometimes not possible to reach an angle allowing adequate reperfusion of skin and soft tissue while maintaining adequate oxygenation, hemodynamic status and a safe airway for patients.”7
Advances in Negative Pressure Wound Therapy (NPWT), which uses suction, tubing and wound dressing to remove excess exudate and any infectious material that may be present in the wound, can help heal complex wounds, reduce healing time and improve quality of life for patients.8
A peer-reviewed poster published at the Symposium on Advanced Wound Care (SAWC) Fall 2020 demonstrated how the Medela Invia Liberty is innovating the standard of care for NPWT.8 The device contains a double lumen technology called Intelligent Pressure Control and Dynamic Exudate Removal, which ensures the prescribed pressure is consistently delivered at the wound bed while reacting to fluctuations in fluid volume or viscosity to more efficiently clear fluid and prevent blockages.
Data-driven cleaning
Environmental services (EVS) professionals play a critical role in reducing infectious disease spread in healthcare facilities. During the pandemic, guidance has been issued to enhance cleaning protocols, while at the same time, protect EVS from contracting the virus.
In June 2021, U.S. Occupational Safety and Health Administration (OSHA) issued its Emergency Temporary Standard for COVID-19, under which healthcare facilities must provide protections to workers. This includes supplying personal protective equipment (PPE), screening everyone who enters the facility for COVID-19 and giving workers time off for vaccination.9
In March 2021, The Association for the Health Care Environment (AHE) published its new Health Care Environmental Services competency model, which it describes as the “first interactive competency model tool for health care environmental services professionals, including technicians, supervisors, managers and directors.” Competency areas include cleaning and disinfection, linen handling, infection prevention, waste handling, safety, communication, patient focus and customer service, and emergency preparedness and response.10
Cleaning and disinfecting healthcare facilities for patient care during a pandemic has been an overwhelming challenge. To help EVS managers efficiently and effectively maintain safe and hygienic environments, Essity now offers a data-driven cleaning approach called Tork EasyCube.
The system uses real-time data, letting EVS managers know when and where to act most urgently. Users can track real-time data on consumption levels of hygiene solutions such as toilet paper, hand towels and skincare. They can also track the number of visitors that have entered a given space to help make sure the proper cleaning effort is executed based on the facility’s desired thresholds.
“Seeing where and when a new refill is necessary or when a cleaning round needs to take place helps avoid unnecessary checks,” said Chung. “Tork EasyCube leads to 24% fewer cleaning rounds, 20% less cleaning hours, 30% more customer satisfaction and bathrooms being stocked 99% of the time.”
“The use of real-time data helps eliminate over (and under) cleaning as it lets you transition from static cleaning rounds to needs-based cleaning. It also helps reporting, analytics and KPI tracking,” Chung added.
Tork EasyCube currently offers three different levels of data-driven cleaning: software solution, people counters and connected dispensers. Customers can pick which level best suits their needs based on the size of their facilities, number of sites and complexity of their operations.
Looking ahead
While COVID-19 has topped media headlines for the past 18 months, other significant dangers that have long existed still pose substantial risks to patient care and safety. As the threats from HAIs, SSIs and chronic wounds continue on top of SARS-CoV-2 spread, the burden on clinicians, EVS professionals and other healthcare stakeholders grows.
Fortunately, some of the same processes, practices and interventions that are effective against COVID-19 are also helpful in the fight against nosocomial infections. If the pandemic has taught us anything it is to wash our hands, protect our airways and be vigilant when it comes to initial symptoms and worsening conditions.
Continuing to apply those lessons, even when (or if) COVID ever leaves the scene, will help provide broad protection against illness moving forward.
References:
1. Hand Hygiene Recommendations, Guidance for Healthcare Providers about Hand Hygiene and COVID-19, CDC, May 17, 2020, https://www.cdc.gov/coronavirus/2019-ncov/hcp/hand-hygiene.html
2. COVID-19 Pandemic, CLABSI, and CAUTI: The Urgent Need to Refocus on Hardwiring Prevention Efforts, UroToday, February 21, 2021. https://www.urotoday.com/recent-abstracts/pelvic-health-reconstruction/urinary-tract-infection-cautis/128157-covid-19-pandemic-clabsi-and-cauti-the-urgent-need-to-refocus-on-hardwiring-prevention-efforts.html
3. Panic buying? Not anymore. Suddenly there’s a surplus of hand sanitizer, USA Today, April 9, 2021. https://www.usatoday.com/story/money/2021/04/08/hand-sanitizer-deals-donations-surplus-panic-buying-pandemic/7120815002/
4. The Role of Antimicrobial Transparent Film Dressings in the Prevention of Catheter-Related Bloodstream Infections, Prevahex, https://prevahexchx.com/case-studies/Role%20of%20Antimicrobial%20Transparent%20Film%20Dressings%20in%20the%20Prevention%20of%20CRBIs_Garcia_2021.pdf
5. Chronic Wounds Affect 6.5 Million in U.S., Intermountain Health, April 25, 2017. https://intermountainhealthcare.org/blogs/topics/live-well/2017/04/chronic-wounds-affect-65-million-in-us/
6. Unavoidable Pressure Injury during COVID-19 Pandemic, A Position Paper from the National Pressure Injury Advisory Panel, https://cdn.ymaws.com/npiap.com/resource/resmgr/white_papers/Unavoidable_in_COVID_Pandemi.pdf
7. New Data Demonstrates Medela Innovates the Standard of Care for Negative Wound Pressure Therapy (NPWT), Medela, November 10, 2020, https://www.medela.com/company/news/news/new-data-demonstrates-medela-innovates-the-standard-of-care-for-npwt?utm_source=hpn&utm_medium=digitalad&utm_content=whitepaperinnovation&utm_campaign=awarenessnpwtinnovation
8. OSHA Sets COVID Safety Rules for Health Care Workers, WebMD, June 14, 2021, https://www.webmd.com/lung/news/20210614/osha-sets-covid-safety-rules-for-health-care-workers
9. EVS Competency Model, AHE, March 2021, https://www.ahe.org/evscompetencymodel
About the Author
Kara Nadeau
Senior Contributing Editor
Kara Nadeau is Sterile Processing Editor for Healthcare Purchasing News.