COVID-19 recovery returns IP teams to holistic HAI prevention
At the start of the COVID-19 pandemic, there was a heightened urgency to clean and protect.
With COVID receding, there is still a need for infection prevention. Other infectious agents, such as Clostridioides difficile (C. diff), Candida auris (C. auris) and central line-associated bloodstream infection (CLABSI) did not go away.
With a smaller workforce and a stressed one, what is next? How do we ensure that infection prevention departments have what they need to achieve the highest standards?
Education is key
The biggest change in the post-COVID era is awareness, said Tristan Williams, Chief Technology Officer, Finsen Technologies. “Prior to COVID, infection prevention was focused on healthcare alone and was the preserve of dedicated specialists, now it is a much broader picture with a much bigger number of enlightened stakeholders. In addition to the awareness, there is more education available than previously, and this is enabling more technical and informed discussion. What has remained the same, is the human factor, specifically caveat emptor (buyer beware) as I have personally witnessed large purchases of completely unsuitable devices for the applications they are intended or tendered for.”
Finsen Technologies told Healthcare Purchasing News that Finsen is focusing on education this year, particularly, the importance of proper floor disinfection using UVC. “This has been an aspect that we have found to be often overlooked and a simple process to integrate into everyday processes to optimize infection prevention measures,” Williams said. “Optimization is key; understanding how each process or technology can overlap and streamline your processes, how the data from each technology can integrate with your management system, [and how to] ascertain [whether] the level of support from each supplier is suitable for your needs prior to purchase or integration.”
PDI is concentrating on continuing education for new staff says Holly Montejano, PDI Clinical Science Liaison, MS, CIC, CPHQ, VA-BC. “There are many new nurses and infection preventionists in healthcare currently who may lack the broader skillsets to successfully do their jobs. With time and resources at a premium, educational offerings for these positions are being made available electronically and free of cost in the form of continuing education credits, which is beneficial to both nursing and infection prevention programs. Also, product-specific information available in electronic learning systems for frontline staff supports just-in-time education, as well as product use compliance.”
Accessibility and infection prevention
The use of computers and other data collection devices in healthcare poses a unique challenge to infection prevention efforts, according to Steve Reinecke, MT(CLS), CPHIMS, Chief Scientist and Regulatory Compliance Officer, Proximity Systems. “It is proven that the faster we have access to information in healthcare, the better the outcomes, yet the data collection devices we are using, if not properly disinfected, can inadvertently be a conduit for patients and staff to become ill,” Reineke said. “The computers at nurse’s stations, patient rooms, and mobile carts, along with pumps and patient monitors are used 24 hours a day. They are rarely manually wiped down or disinfected and there is seldom training or documented procedures around the cleaning of these surfaces. Housekeeping, nursing and IT disputes over who is responsible for the computer workstation, pumps and patient monitor cleaning, with these surfaces being some of the dirtiest places in healthcare, contribute to the prevalence of healthcare-associated infections (HAIs) that lead to morbidity, mortality and excess healthcare expenditure.”
Sarah Simmons, DrPH CIC FAPIC, Senior Director of Science, Xenex, emphasizes the issue of efficacy in new products, especially during the pandemic. “New products flooded the market during the pandemic, and many of them made wild claims about efficacy. I am hopeful that hospital decision-makers now have the time to ask for and review peer-reviewed articles about any technology they are considering,” she said. “Ask the manufacturer to provide you with multiple peer-reviewed and published studies validating the efficacy of that specific device or system in a hospital setting that proves the technology works. Anecdotes and posters are not enough. If the technology hasn’t been proven effective in multiple peer-reviewed studies, then it hasn’t met the bar of an evidence-based solution.”
GOJO says that communication is key. “Showing healthcare facilities our control over key raw materials and components, walking them through our approach to redundancy and partnerships, and being open not just about what we can do but how, has been extremely helpful to our hospital partners,” said Jaimee Rosenthal, Acute Healthcare Market Director, GOJO Industries.
“Open communication about our ability to satisfy their needs for these critical infection control products lets healthcare facilities focus on what’s most important – the health and safety of their staff, patients, residents and visitors,” she said.
Then and now; Lessons learned
Montejano, PDI, quoted an article from the Journal of Infectious Diseases entitled, “History of infection prevention and control,” stating: “The acute care setting saw the inception of the infection control professional in the 1950s because of a nationwide healthcare-associated Staphylococcus aureus epidemic.”1
“Now, infection preventionists wear many hats within a facility, working with internal stakeholders to ensure policies and procedures are being followed to keep patients safe and infection free,” Montejano continued. “The pandemic has highlighted issues that arise when these programs are not in place, particularly along the continuum of care, such as long-term care facilities. Given the collateral damage the pandemic has caused (in terms of HAI increases, staff shortages, staff burnout), infection prevention programs are an imperative healthcare initiative that helps provide patient safety guidance and ensures compliance with best practices,” Montejano said.
Doe Kley, Senior Infection Preventionist, Clorox Healthcare, stresses the importance of learning from the past and applying it to future practices. “Early in the pandemic, before much was known about COVID-19, inside and outside of healthcare facilities implemented extreme cleaning and disinfecting. This subsided as we learned more about the virus and how it is transmitted. However, it is important to apply the lessons learned and is an opportune time for Infection Preventionists (IPs) and Environmental Services (EVS) to continue to collaborate and assess if the cleaning and disinfection procedures they have adopted throughout the pandemic still serve the facility’s needs and meet regulatory requirements,” she said.
Kinnos CEO, Jason Kang, maintains that having a documented and formalized infection prevention program is critical because it requires a coordinated approach across multiple departments where each stakeholder understands their role and the right products and processes to implement.
Kinnos notes that their Highlight for Bleach Wipes are experiencing an elevation in demand. The company claims that the additive for bleach wipes tackles the key pain points of quality, training and patient engagement.
“Respectively, these demands have been driven by labor shortages and high staff turnover rates, rising HAI rates, and COVID impacting patient perception of cleanliness and safety in healthcare facilities. Post-COVID, we have seen an emphasis on initiatives around patient safety and engagement. While our Highlight product has been used to achieve significantly better disinfection quality scores, as a result of COVID, hospitals are now also using Highlight to engage with patients and improve HCAHPS scores,” Kang said.
Protect your staff
Staffing shortages are very real and placing a continued strain across all healthcare personnel, said Peter Veloz, Chief Executive Officer, UVDI. “Products that are simple to train on and use are critical; products that fit into workflow versus disrupting it. Fundamentally, the challenge remains the same; Infection Preventionists and Environmental Services are tasked with ‘doing more with less.’ So, the critical question for manufacturers is for product design to enable efficiency while still delivering effective performance. The UVDI-360 Room Sanitizer can be operated in just a few taps on its large, multilingual, color touchscreen – or remote control – and can disinfect a typical-sized patient room in just 10 minutes,” he said.
Labor shortages can cause lapses in proper hand hygiene protocol, said Deborah Chung, North America Marketing Manager, Healthcare, Professional Hygiene, Essity. “According to survey results from a 2021 survey conducted by Essity, 90% of respondents believe that increased cleaning and sanitizing is important in hospitals and healthcare facilities. Additionally, 84% of respondents reported intending to continue the enhanced hygiene practices they adopted during the pandemic, which provides evidence that boosted hygiene habits developed due to COVID are not going away. This makes access to trainings like the Tork Clean Hands Training, that support hand hygiene compliance, more important than ever.”
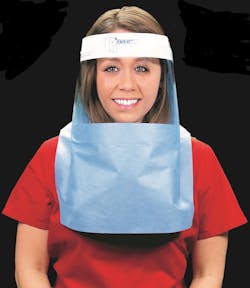
Protecting staff from infection with proper personal protective equipment (PPE) is also important. Onyx Medical manufactures a face shield called Drape-U, to protect wearers from splash exposure.
“Most departments are at risk from exposure to COVID or other aerosolized pathogens. As an AJIC study2 details, standard shields without barrier fabric do not protect well enough against splash exposure,” said Roger Machson, Owner, Onyx Medical.
HAIs did not go away...
Candida auris is on the rise, according to Maryalice St Clair, Chief Commercial Officer, Halosil. “Although clinical cases are still limited to a relatively few number of U.S. states, IPs are well aware that this infection is a growing threat. And of course, our long time nemesis C. diff is still an HAI that continues to be a cause of concern for IPs.”
PDI contends that the diversion of resources and lack of colonization screening during the pandemic has allowed Candida auris to flourish across the continuum of care, according to Montejano.
“One of the biggest challenges facing infection prevention is the uptick in healthcare-associated infections (HAIs) due to shifting priorities during the pandemic. As infection prevention resources had to be diverted for COVID-19 patients and product availability was problematic due to supply chain issues, this unfortunately led to some evidence-based best practices falling to the wayside. As a result, infection prevention initiatives suffered. Now, many facilities are taking a back-to-basics approach with their HAI prevention bundles, revisiting compliance with the interventions included in those bundles via education and auditing,” she said.
A newer element to the CLABSI and surgical site infection (SSI) prevention bundles includes nasal decolonization she continued. “This intervention using an iodophor-based product has been shown to be beneficial in HAI prevention research and is included as a recommendation in both the Centers for Disease Control and Prevention (CDC) Strategies to Prevent Hospital-onset Staphylococcus aureus Bloodstream Infections in Acute Care Facilities3 as well as the updated AORN Skin Antisepsis Guideline.”4
Williams from Finsen warns us to “keep an eye on the changing landscape,” stating, “chlorine resistance is becoming a real concern with multiple papers illustrating this (especially for C-Diff) and this highlights that manual cleaning alone is simply not enough anymore for healthcare facilities and anti-microbial stewardship is an imperative responsibility for us all.”
Karen Hoffmann RN, MS, CIC, FAPIC, FSHEA, [Nuvo Surgical] recommends using a ultraviolet germicidal irradiation (UVGI) system to purify air. “Rather than relying on the least effective control measure, i.e. appropriate wearing of masks, healthcare facilities should implement more effective administrative engineering control like better ventilation that can protect everyone in the room continuously.”
Kalvin Yu, MD, FIDSA, Vice President of U.S. Medical Affairs, BD, stressed the importance of having resources to battle antimicrobial resistance (AMR). “Capabilities that aim to identify the most appropriate and timely use of antimicrobials with the goal of containing and reducing AMR are more important than ever – particularly as health systems manage seasonal healthcare needs in tandem with COVID-19.
Priority capabilities should include:
- Supporting infection control guidelines through products and services designed to help clinicians improve patient outcomes through the standardization of care.
- Expanding diagnostic testing to classify infections and guide therapies – helping clinicians to implement effective antimicrobial stewardship interventions.
- Advancing medication management through a connected medication management system with technologies, analytics, and surveillance tools to ensure the appropriate utilization of medications,” he said.
During this ‘return to normalcy,’ Infection Preventionists cannot simply return to normal. Rather, they must champion the best practices that define their trade. According to Alice Brewer, Senior Director, Clinical Affairs, PDI, “Back to basics does not mean that Infection Preventionists are not doing their jobs or have forgotten how. It is an understanding that we need to shift away from the emergency or pandemic mindset and resume routine evidence-based interventions and strategies. Now is the time to return to best practices and seize the opportunity to evaluate new products, technologies, and procedures to help combat rising rates of HAIs and ensure we are prepared for potential future outbreaks.”
Veloz, UVDI, reminds us that, “We have emerged through the pandemic’s darkest days, let us remember that brave healthcare professionals continue to selflessly work every day to keep us all safe from the threat of antibiotic-resistant organisms and infections. Their commitment is steadfast and it is more important than ever to thank them.”
Vendor listings & product spotlights
References:
1. Torriani, Francesca, and Randy Taplitz. “History of infection prevention and control.” Infectious Diseases (2010): 76.
2. Ofstead CL, Hopkins KM, Smart AG, Brewer MK. Droplet dispersal in decontamination areas of instrument reprocessing suites. Am J Infect Control. 2022 Feb;50(2):126-132. doi: 10.1016/j.ajic.2021.10.023. Epub 2021 Dec 2. PMID: 34865859.
3. https://www.cdc.gov/hai/prevent/staph-prevention-strategies.html. Accessed May 9, 2022.
4. https://www.aorn.org/about-aorn/aorn-newsroom/periop-today-newsletter/2021/2021-articles/ssi-prevention-bundle. Accessed May 9, 2022.
About the Author
Erin Brady
Assistant Editor
Erin Brady is Assistant Editor for Healthcare Purchasing News, an Endeavor Business Media publication.