Integrating dynamic sourcing in hospital supply chain purchasing
In the ever-changing world of healthcare, the costs of medical supplies and equipment fluctuate, impacting business and financial operations. In order to best keep pace with the marketplace, hospitals and health systems, consequently, should look toward creating greater flexibility, transparency, and decision making around supply chain pricing, sourcing, and purchasing.
Nearly all other industries view their supply chains to be mission critical to the financial success of their organizations. Hospitals, however, have proven this to be contrary to their operational strategies, which is reflected in their inherent lack of resources and their decision to outsource many supply chain functions, especially sourcing.
For hospitals and health systems to most effectively and efficiently address this spend, they need to take control of their supply chains by deploying sourcing technologies and analytics as part of a dynamic sourcing model. Shifting from a traditional static contracting model, which many systems use today, to a dynamic sourcing model that facilitates periodical pricing negotiation, could result in securing best available market pricing from contracted and non-contracted suppliers and improving budget goals and financial outcomes.
Pandemic supply chain plight and opportunities
The COVID-19 pandemic has brought transparency to the adverse effects of not viewing supply chain as a mission-critical element to financial success. In many cases, hospital supply chains failed to provide adequate support from the onset of the pandemic, including their outsourced partners, such as distributors and group purchasing organizations (GPOs). And to make matters even more challenging, many hospitals decided to double down on this strategy by furloughing supply chain resources.
COVID-19 has shined a bright light on the critical importance of hospital supply chains, which likely has leadership strongly desiring to change their current supply chain landscape and is causing a degree of uncertainty as to an appropriate and a viable solution.
How the dynamic sourcing model works
First and foremost, hospitals need technologies in place that provide real-time visibility into current market pricing for supply purchases made across GPOs and peer organizations. This visibility is vital to ensuring that hospitals are paying the lowest possible price available based on their spend volume and market share. Transitioning to a dynamic sourcing model is the most logical and stable method for hospitals and health systems to instill continuity within their supply chains.
Technologies that capture last price paid from closed receipt invoices, representing thousands of hospitals across every GPO and self-contracting integrated delivery network (IDN), provide full pricing transparency. The fastest way to cost savings is to pay the appropriate market price from incumbent suppliers. Paying current competitive market pricing for medical, surgical, and pharmaceutical supplies leads to greater procedure margin and sustainable cost control. The best of the best likely have access to five to eight percent in cost savings through simply paying the lowest available qualified price, where most hospitals likely have access to north of 12 percent available cost savings.
Five Myths
- Suppliers provide most competitive market pricing to GPOs.
- Long-term, committed contracts deliver the most competitive market pricing.
- Available benchmark pricing data and technology offered by GPOs and third-party vendors ensures alignment with most competitive market pricing
- Suppliers ensure pricing parity throughout a health system.
- Focusing on product utilization versus product pricing is the fastest way to cost savings.
VIP products in hospital care
Hospitals buy millions of products to take care of patients. Similar to the auto industry, hospitals need to give greater scrutiny with regard to purchasing supplies. They need to become more competitive and engaged in their supply chain operations, as well as pursue fair market pricing.
The slowest way to cost savings is to convince medical staff members to use products they do not want to use. Physician preference items (PPI), purchased services, and specialty drugs, respectively, continue to be the three largest non-labor operating expenses. These three areas also offer the greatest opportunity for cost savings, mostly due to the fact of how these items are being procured and managed.
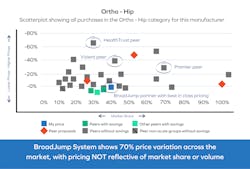
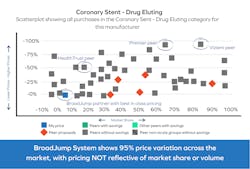
More often than not, especially with PPI, suppliers do not provide their most competitive pricing to GPOs, since they believe they will need to provide lower pricing to hospitals to receive market share and volume commitment. This market pricing strategy, deployed by most suppliers, creates market pricing variation in many product categories, and therefore requires constant monitorization of current market pricing provided in numerous categories.
Data drives pricing comparison, competitive negotiation and costs savings for healthcare organization
Mosaic Life Care1, for example, is one healthcare organization that has integrated technology to help monitor current marketing pricing and keep costs down in their supply chain operations. Mosaic is nationally recognized for quality, value and patient experience in traditional healthcare and wellness support for residents in the St. Joseph, MO region. Their services include family care, urgent care, emergency care and a large variety of specialty care, therefore their staff must always have access to standard and specialty medical equipment.
As PPI typically account for a high percentage of supply chain expense, Mosaic wanted an easy, efficient way to monitor medical-surgical product pricing in order to ensure that their pricing was competitive across all vendors and to speed up the negotiation process for new product contracts.
Mosaic employed BroadJump’s AutoPricer and PriceChecker solutions to better understand their supply chain expenses. They were able to track current medical-surgical pricing to discover savings opportunities through pricing of peer facilities with similar spend, volume and market share, as well as analyze quotes and proposals to negotiate lower pricing. In the first month using these solutions, Mosaic realized more than $400,000 in savings without changing one SKU or affecting current clinical practice. Using BroadJump’s real-time repository of expense data from facilities across the nation, they were able to determine realistic opportunities with pricelist-to-pricelist comparisons. The supply chain team was able to reduce costs across several PPI, resulting in significant savings.
“I have personally used BroadJump at two different health systems now, and both times the results were outstanding,” said Sean Poellnitz, BS, CHRM, Vice President of Supply Chain, Mosaic Life Care. “As a Supply Chain Executive, BroadJump gives us the ability to forecast and bring home the real savings that we promised our CFO.”
GPO contract and spending
The traditional hospital sourcing model uses long-term GPO contracts for high dollar purchase volumes and multi-source contracts for PPI. This model, in turn, creates a pricing disadvantage and reduced operating margins since non-labor expenses represent nearly fifty percent of a hospital’s operating budget.
GPO contracts typically apply to about 35 percent of a hospital’s non-labor expenses. These contracts generally carry a three- to five-year term with fixed tier-level pricing, which often do not offer best market pricing from the onset of the contract. These lengthy contracts unintentionally trap hospitals into unfavorable product pricing positions, with very limited resources to negotiate better pricing, thereby causing one to miss out on years of savings opportunities. It is quite possible for a newly negotiated GPO contract to have out-of-market pricing as early as 90 days after the contract start date.
The remaining 65 percent of non-labor expenses commonly are purchased outside of GPO contracts and ideally need to be locally negotiated contracts in order to secure competitive pricing. The larger portion of this spend, representing as much as fifty percent, falls within the following three areas: PPI, purchased services, and specialty drugs, respectively. Unfortunately, most hospitals and health systems do not have adequate technological, analytical, or human resources to be able to most effectively address this spend.
Sourcing strategy, efficiencies and savings
The dynamic sourcing model, used by Mosaic Life Care and other organizations, is a best practice for hospital supply chain management. This model, ultimately, opens the door for numerous potential benefits and efficiencies in business operations and financial outcomes, including:
- Promotes periodical pricing negotiation with suppliers.
- Ensures one is paying the best available market pricing at the point of purchase.
- Virtually eliminates the need for requests for proposals (RFPs).
- 4. Reduces supplier negotiation time by as much as 70 percent.
- Delivers seven to 10 percent in annual supply savings year over year.
- Reduces annual supply spend by as much as 15 percent.
The healthcare landscape and marketplace will continue to evolve and affect hospitals and healthcare systems. Now is the time for them to take the next step and adopt the dynamic sourcing model as part of their mission-critical supply chains. Their sourcing teams, undoubtedly, need more tools, insights and resources in order to be operationally and financially successful. This can be realized through implementing technology, data and transparency into supply chain management.
“BroadJump simply represents a game-changing sourcing intelligence platform that enables us to craft creditable sourcing strategies for medical-surgical product negotiations.”
—Mosaic Life Care’s Vice President of Supply Chain,
Sean Poellnitz, BS, CHRM
1. Mosaic Life Care saves $400,000 in less than one month with BroadJump’s solutions without changing one SKU or affecting clinical practice, https://www.broadjumpllc.com/insights/success-stories-and-papers/mosaic-life-care-saves-400000-in-less-than-one-month-with-broadjumps-solutions-without-changing-one-sku-or-affecting-clinical-practice/?utm_source=hpn&utm_medium=link&utm_campaign=successstory&utm_content=mosaiclifecare