The ups and downs of SPD from 2022 to 2023
The average annual salary of Sterile Processing Department (SPD) professionals is up 3% this year at $69,217, compared with $67,096 in 2022. What is surprising is a 14% drop in survey respondents reporting a yearly pay increase (56% in 2023 down from 70% in 2022). Those reporting the receipt of bonuses in 2023 held steady from 2022, at 24%.
These results and others from the 2023 Healthcare Purchasing News SPD Salary Survey provide insights into not only compensation, but also job security, certification, continuing education, and shifting roles and responsibilities. SPD professionals commented on their individual experiences and offered their thoughts on the field and its future.
Fluctuations in salary by title, males still lead in pay
While there were no dramatic shifts in salary by role from 2022 to 2023, there were some slight ups and downs, likely because of changing demographics of survey respondents from year to year.
The total number of SPD professionals taking part in the survey rose, at 378 respondents compared with 177 in 2022. Looking at the titles of those who participated this year, there were 8% fewer Lead SPD Technicians and 5% fewer SPD Technicians/Coordinators compared with last year. Other shifts in respondents by title were up or down by 4% or less.
When looking at reported pay by title, the survey data showed average annual increases for SPD Supervisors ($61,267 up from $58,863), Surgical Instrument Technicians ($57,034 up from $55,055), SPD Managers ($88,210 up from $86,756), SPDTechnician/Coordinators ($52,566 up from $49,083) and SPD Directors ($140,674 up from $139,867).
Decreases were found among the average annual salaries of SPD Educators ($64,586 down from $65,500), Lead SPD Technicians ($39,321 down from $41,176), Certified Medical Device Reprocessing Technicians ($44,485 down from $45,833) and OR Liaisons ($51,345 down from $52,500).
Again, this year those respondents identifying as male earned more than those identifying as female: $79,240 compared with $66,209, respectively, with 2% of those surveyed choosing not to disclose their gender.
“I feel like our profession is severely underpaid for the knowledge, material and extensive memory retention we are needed for daily/weekly duties,” said Sean Weir, CRCST, CIS, CHL, Sterile Processing Educator, UPMC. “We need to know microbiology, infection prevention, anatomy, chemistry, and then the vast instruments out there. The world needs to understand that this field is no longer a ‘entry level’ job and more a career-oriented profession that is not a glorified dishwasher. It is a shame that the healthcare market is being paid less than those at fast food restaurants or retail, we are aiding in the saving of one’s life one tray at a time.”
“I have found many SPD Techs need training around negotiation, especially when they’re new hires and often don’t understand there is a pay scale and the opportunity to ask for higher pay,” said Nicholson.
She noted another major issue in SPDs: staff members being asked to take on responsibilities beyond their title and paygrade. She stated:
“A Lead SPD Tech may be asked to perform to the level of Supervisor, a Supervisor to that of a Manager, and a Manager to that of a Director. This is problematic when they don’t get compensated for that higher level work and don’t have that higher level title or pay grade to carry onto their next employer.”
“Over the years, we have seen so many challenges and staffing/pay/recognition have always been high on the list of concerns voiced by our professionals; however, we continue to fight, lead and work with our leadership to make these challenges better and not just talking points.”
“I will always be that positive warrior for change, and that change happens through action,” Berg added. “When we are feeling all the pressures and not feeling appreciated, and even when we are understaffed and underpaid, we must not only show up but prove our value and worth. That is when we will start to see sustaining, positive change. It will be teamwork, education and documentation that will open doors for our profession.”
The impact of education and location on SPD salaries
As in past years, the higher the level of education reported by SPD professionals, the higher the annual average salary. Those with post graduate degrees (2% of respondents) reported taking home an average of $92,289 per year, this was down from $103,384 in 2022.
SPD professionals who had earned bachelor’s degrees (13% of respondents) reported an average annual salary of $76,074, down from $81,354 last year. Among respondents with associate degrees (26% of respondents), average salary was $59,245, down from $66,519 in 2022. SPD professionals with high school as their highest level of education reported annual average pay of $57,234, up from $56,310 last year. Looking at the demographic data, there were fewer survey respondents reporting a high school level education compared with last year (32% down from 46% in 2022).
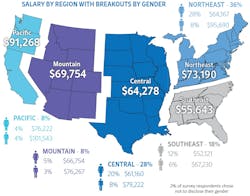
Geography played a role in compensation once again in 2023, with each region showing pay increases over 2022. SPD professionals from the Pacific states had an average annual salary of $91,268 (up from $86,916), the Northeastern states $73,190 (up from $70,000), Mountain states $69,754 (up from $67,148), Central states $64,278 (up from $62,974), and Southeastern states $55,643 (up from $53,541).
SPD professionals in urban areas (41% of respondents) reported the highest average annual pay in 2023 at $75,123 (up from $73,224), followed by those in the suburbs (35% of respondents) at $72,093 (up from $68,500), and rural areas (24% of respondents) at $58,821 (up from $53,075).
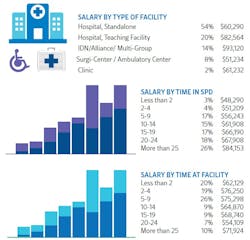
With regards to facility type, SPD professionals working for IDN/alliance/multi-group institutions earned the highest at $93,120 annually (up from $89,148), followed by teaching hospitals at $82,564 (up from $79,535), standalone hospitals at $60,290 (up from $58,070) and surgicenters/ambulatory centers at $51,234 (up from $52,261).
SPD feeling secure, but are staffing shortages behind it?
The survey findings indicated that SPD professionals are feeling more secure in their jobs, with 94% feeling “very or somewhat secure,” compared with 85% in 2022. Average annual salary increased by time in the SPD profession, with those with 25+ years of experience earning an average of $84,153 and those with less than 2 years $48,290.
Several of the SPD professionals interviewed for this article cited staffing shortages as a major challenge to the profession. Could it be those in the profession are feeling more secure because there is less competition and more opportunities?
“For the 40 locations I oversee, there are over 75 SPD vacant positions, some with a department of 12-15 and of that eight are travelers,” said Weir.
“We are not alone with these concerns and questions about what is next, how we can find more help, and how we can retain qualified staff,” said Berg. “With a lot of jobs in healthcare facing critical shortages, the challenge will be how we stand out and get the assistance we need.”
“The short answer is continuing to do the great work we can by providing outstanding processing of medical devices,” Berg added. “Do not give anyone a chance to doubt our work or dedication - and keep us in the positive light with hospital leadership so they are more inclined to support well-functioning and productive departments.”
Fewer staff members, greater errors
“Overtime hours have always been desired, however, now they are demanded,” said Jelks.
According to Jelks, there has been an increase in tray errors in many level one trauma facilities, which she credits to “fatigued technicians who work excessive amounts of overtime to the point of exhaustion - losing their normal focus skills.”
McGlynn said she has seen more SPD technicians leaving their jobs and “searching for better accommodations and culture,” including adherence to industry standards, stating:
“We all have a higher awareness to changes in the standards. It’s not so much of putting off changes, but more planning on how to implement new guidelines. More people in SPD are buying into change, which makes our jobs more efficient and foolproof. This is creating a circle effect, for our new and veteran techs being educated to new standards and have better expectations for ourselves.”
An aging workforce
Over half (52%) of survey respondents were age 51 or older, and among those, 18% were between the ages of 61-70. Nearly half (45%) fell into the 31-50 age range, while only 1.5% were between the ages of 21-30.
Kim Hughes, BA, CRCST, CHL, CIS, Central Processing Manager, Good Samaritan Hospital, Vincennes, Ind., said the aging workforce and high turnover have played a role in her department’s staffing challenges, stating:
“There are quite a few of the staff that are at retirement age and when they retire, we lose that experience. Currently, when we do hire, we must understand that a lot of the ones hired will stay approximately a year and then move on. In SPD it takes about a year to feel comfortable in what you are doing and not be overwhelmed. Even if staffing is not a concern, the work is rigorous and physically hard on the body and there are safety concerns which one must always be aware.”
Hughes added: “Yes, we have had staffing challenges but the staff that are here are dedicated! One had thought of retiring last year but didn’t want to leave us any shorter at that time. (Who else would do that?) I think the staff who are working through the shortages are some of the hardest working and caring. The shortages are hard, but I am very thankful for the people who are here.”
Travelers can both help and harm
Today’s environment of mandatory overtime is driving some SPD technicians to leave the “traditional role in hospitals to take on contract work and or travel assignments,” according to Jelks.
“They can work so many weeks at a time then take off one or two weeks in between the 8– to 13-week assignments and get paid twice as much,” said noted. “Although contract work positions have a downside, such as full-coverage healthcare insurance and desired work location, it is still today a very desirable for technicians working above 40 hours per week to make surgery ends meet.”
Weir said while “travelers are a great way to fix a short-term staffing shortage” it is not a sustainable solution, stating:
“My issue with travelers is simple, they are not invested employees of the location and just want to work their 6–13-week contract and move on. Hospitals across the world cannot survive with this current model. We need invested workers to improve the locations and improve patient care, but then that goes back to paying better.”
Nicholson said the opportunity to travel changed her life and she encourages other SPD professionals to pursue a travel career, stating:
“I was working for a hospital in my hometown making minimum wage when we hired a traveler, and she told our team about opportunities to advance our education and careers. One by one we each took steps to become certified and take on travel positions. As a young person, I found myself traveling across the country, which really set off my career. In those first three years, I doubled my income each year.”
Nicholson added that it is not just young, single SPD professionals who are benefiting from the travel trend but also more experienced individuals and those with families.
“I see moms and dads traveling to make money to send back home. But there are disparities when you compare travel opportunities for nurses with those for SPD. For example, nurses are typically provided room and board as part of their travel contracts and even the opportunity to fly home on weekends to stay connected with their families. Most SPD travel positions don’t offer these benefits.”
The need to nurture the next generation
Those interviewed cited the need to educate students, down to the high school and even grade school level, on the sterile processing profession to help recruit and cultivate the next generation of professionals.
McGlynn said one positive side effect of the current SPD staffing shortages is that “more hospitals are actively creating training programs, reaching out to younger individuals through grade schools and even up to college levels.”
“The industry as a whole needs to promote the field more heavily in 10th and 11th graders as a career path, reach out to community colleges and figure out to get a program started, not just a “read the book” course but a true hands-on approach,” said Weir.
Certification levels hold steady, with higher pay reported
When asked if they were certified, 92% of respondents said “yes,” which was on par with last year at 91%, and the same percentage of SPD professionals said they were in the process of becoming certified at 5% in both 2023 and 2022. Respondents who were already certified reported the highest average annual pay at $69,120, followed by those in the process of certification at $60,254.
When asked if their employer required certification, the response was similar to last year at 69% saying “yes” (70% in 2022). Those reporting employers without certification requirements was only slightly higher (28% in 2023, 26% in 2022). Additionally, 3% said their employers were considering instituting certification as requirement, compared with 4% last year.
When asked whether their employers give them higher levels of compensation for obtaining certified education units/points, only 14% said ‘yes.’
“I believe that decision makers who control the financial resources fail to see the true value or equity in this role,” said Perkins. “Although SPD does not generate income directly, they do so indirectly. And this department can be a preventative measure to avoid negative patient outcomes. As a rule, healthcare facilities with better wages will attract better professionals and thereby strengthen the facility’s ability to court preferred physicians.”
“I believe there must be public advocacy for this position,” he added. “The last thing we would want to happen are national strikes from this department. And contrary to some popular belief, sterile processing roles, or experienced processing roles, are not easy to backfill. It would be a disaster if a national strike was to ever happen, and it would ultimately paralyze our healthcare system, nationwide.”
Respondents certified by the HSPA dropped to 67% in 2023 from 76% in 2022, which could be a leveling off from a 7% jump from 2021 to 2022 (69% to 76% from one year to the next). Those certified by the Certification Board for Sterile Processing & Distribution (CBSPD), fell as well at 25% in 2023 down from 28% in 2022, whereas in 2021, 28% of respondents reported being CBSPD certified.
“Lately it has been increasingly difficult to find a location to take the certification exams,” McGlynn commented. “In some cases, there is only one location in a major metropolitan area. Globally this is also an issue as some SPD Professionals outside the US are required to travel into the country to take their exams. There must be a better way to offer exam by proxy.”
Association for the Advancement of Medical Instrumentation (AAMI) certifications were up at 23% in 2023, from 21% in 2022, as were those for the Association of Surgical Technologists (AST) at 10% in 2023 from 7% in 2022. Respondents with Association of periOperative Registered Nurses (AORN) certifications held steady from last year at 8%.
Shifts in reported specific certifications varied slightly from last year:
• Certified in Healthcare Leadership Strategies (CHL): 32% in 2023 up from 31% in 2022
• Certified Sterile Processing Distribution Technician (CSPDT) 20% in 2023 up to 23% in 2023
• Flexible Endoscope Reprocessor Certification (CFER): 19% in 2023 up from 17% in 2022
• Certified Surgical Technician (CST): 12% in 2023 up from 10% in 2022
• SPD Technician Certification: 10% in 2023 up from 7% in 2022
• Certified Registered Central Service Technician (CRCST): 66% in 2023 up from 69% in 2022
• Certified Instrumentation Specialist (CIS): 30% in 2023 down from 32% in 2022
• Certified HSPA Instructor: 2% in 2023 down from 6% in 2022
• SPD Manager Certification (CSPDM): 4% in 2023 down from 5% in 2022
According to Hughes, staffing shortages have made it harder to find the time and resources for SPD departments to train new staff members and provide opportunities for current staff to advance in their education. She stated:
“When there are shortages in staff, it is a challenge to train new staff, to get education to all staff, to encourage staff to participate in meetings or associations and to not become burnt out. All those things are necessary to have a well-trained proactive staff, but we are focused on getting the needed instruments ready for cases because the patient is our first priority.”
SPD professionals reporting 10 or more continuing education courses/lessons each year dropped from last year, at 80% in 2023 down from 88% in 2022, as did those who indicated they participated in 20 or more courses/lessons, 39% in 2023 down from 44% in 2022.
McGlynn’s advice to current and next generation SPD professionals with regards to furthering their education and careers: “Let negativity go. Follow your own path.” She stated:
“Get involved with your chapters whether you’re new to the field or seasoned. Get your certifications. Hospitals are starting to look into upgrading our pay. Hopefully, that means the certifications will pay off for your efforts. Having a solid foundation from learning and retaining from your certifications will be key for your future. Share your knowledge with everyone. I am sharing all my resources with my co-workers. As a lead, I integrate listening to SPD podcasts during our shift when there is an interesting topic.”
“We must cut the chains off everything that is gatekeeping education and information is the best way to support everyone,” she added. “Information is going to help our SPDs get the equipment we need; being able to show data when asking for support from the C-suite. We should be building our confidence as professionals because we are professionals. Knowledge is going to help the individual build their skillset and become more valuable to their department.”
Reporting, processes and technologies
When looking at hospital reporting structures and which functions report directly to the SPD department heads in their facilities, there was an 11% jump in survey respondents that said GI/Endoscopy reports to the head of SPD (41% in 2023 up from 30% in 2022).
There was a 4% increase across the board for storeroom, medical equipment cleaning/disinfection, and central transport reporting to the SPD department head compared with the 2022 survey results. Conversely, there was a 3% decrease in respondents who said decontamination and case carts reported to their department heads.
When asked if their facility had changed its methodology around the use of manufacturer instructions for use (IFU), there was a 9% increase in SPD professionals who reported changes, (25% in 2023 up from 16% in 2022). There was an 8% increase in those stating their facilities had put new measures (process and/or products) in place to further minimize the risk of reprocessing related outbreaks (52% in 2023 up from 44% in 2022).
Survey respondents that said their facilities use track and trace systems for their instruments increased by 3% (65% in 2023 up from 62% in 2022), while reporting use of sterile processing workflow management systems dropped by 7% (46% in 2023, down from 53% in 2022).
As in past years, most respondents use steam sterilization (98%). There was a decrease in those reporting use of hydrogen peroxide (76% in 2023 down from 85% in 2022), immediate use steam sterilization (41% in 2023 down from 50% in 2022), gas plasma (27% in 2023 down from 31% in 2022), and EtO (4% in 2023 down from 11% in 2022).
There was little change in those using Cidex OPA (31% in 2023 down from 32% in 2022), glutaraldehyde (12% in 2023 up from 10% in 2022), peracetic acid (25% both years), UV-C (2% both years), and ozone (2% both years).
Complex technologies prompt demand for advanced SPD solutions
“As the world of technology becomes more and more complex so does the advancement of instruments,” said Weir. “Some instruments we are tasked to clean take an hour to just do the manual cleaning process, tie that in with the other 30-110 cases a day and it is just plain crazy. 3D printed models are being used more and more and their IFUs are so complex that we still need to reference them each time we get them in and sterilize them.”
With regards to the growing complexity of surgical technology and its impact on SPD professionals, Jelks offered the example of reprocessing robotic arms, commenting on how it requires “a very labor-intensive process of inspecting and decontaminating.”
“Robotic arms have a short life span, and technicians must be mindful of expiration indicators prior to and after reprocessing,” said Jelks. “Departments without proper disinfection machines and equipment for reprocessing arms will have a harder time prioritizing and completing trays due to the amount of work it takes to manually reprocess robotic arms.”
McGlynn feels growing education among SPD professionals has prompted them to increasingly demand of decision makers the technologies they need to perform effective and safe instrument reprocessing. She stated:
“I have noticed a shift in the way funds are being invested into our departments. Ideally, we want every SPD to have all the bells and whistles to provide top notch care every time an instrument is reprocessed. In the past, you would not even bother asking for a borescope because most techs were not even aware of what a borescope is. Now, they are more educated enough to ask the hospital to provide one so they can properly follow the IFU. It seems to me companies are trying to keep the staff they have which means equipment needs to be fixed and updated.”
In her work, Nicholson provides financial education to SPD managers to help them navigate the complex process of yearly budgeting and capital requests in the hospital so they can make their case to leadership on what their department requires in terms of staffing and equipment.
She pointed to the increase in mass shootings in the U.S. and how hospitals presented with multiple victims may not have the instrument sets required to care for all of them, stating:
“Before, if there was a shooting, there were maybe one or two people requiring emergency care but now hospitals are being presented with five or 10 victims all at once. In SPD, we may not have enough instrument trays to support care of these patients or find ourselves having to reallocate trays intended for scheduled surgeries to these trauma cases.”