Maintaining normothermia in the surgical patient — keeping core body temperature consistently above 36° C (96.8° F) — demands diligence, adherence to best practices, and choosing temperature management products that are well suited to patient and procedure.
Today, much of the focus is on finding ways to keep patients warm — and the discourse can get quite heated. In fact, the assorted views and opinions about which methods are most effective and safe, including those populating the pages of medical science journals, seem so polarized one wonders which way to go.
What everyone does seem to agree on is that unintended perioperative hypothermia (UPH) is still a problem that healthcare facilities want to resolve — and for good reason. An estimated 20 percent of surgical patients experience UPH, which increases the risk of morbid cardiac outcomes, surgical blood loss, transfusions and surgical site infection (SSI). When patients get cold the potential snowball effect isn’t hard to imagine.
“Warming in general needs extra attention,” said Scott Augustine, MD, founder of Augustine Temperature Management. “Despite active warming, rates of hypothermia are much higher than clinicians understand. Clinicians need to understand that the amazing benefits that normothermia contributes to improved surgical outcomes do not occur without effective warming.”
Methods vary
Byron L. Burlingame, MS, RN, CNOR, a Senior Perioperative Practice Specialist with the Association of periOperative Registered Nurses (AORN), says a number of active and passive approaches can be used to achieve normothermia and that the process may start at the preoperative stage and end at the point of discharge. Active warming methods, he said, might include increasing the ambient temperature and/or employing one or more of the following devices:
- radiant warming device
- forced-air warmer
- water-filled mattress
- circulating water garment
- warmed IV and irrigation fluids
- electric warming blankets
- carbon fiber blankets
- resistive polymer blankets
- electric heating pads
- plastic garments
- thermal exchange chambers
- negative pressure warming systems
Passive warming methods include use of cotton blankets, surgical drapes, plastic sheeting, and blankets or garments made of reflective composite fabric (e.g., space blankets).
“It’s important to not assume one warming system will work for every patient,” asserted Burlingame. “The choice of warming systems depends on the patient and the procedure.”
Some manufacturers suggest otherwise and say warming systems are available that will allow users to achieve normothermia successfully in many cases.
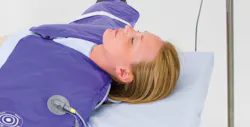
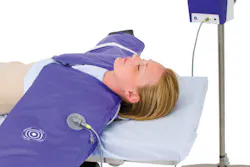
“It is important to have a versatile warming system that can be used effectively for all different types of procedures and patient positions,” said Augustine, referring to his company’s HotDog product, a conductive warming system consisting of mattresses and blankets made with a ThermAssure fabric that uses low-voltage electricity to create heat above and beneath the patient simultaneously. Augustine said warming a patient with the HotDog system costs between $2 and $3. “Simultaneous under-body warming and over-body is critical because warming effectiveness is a function of surface area,” said Augustine. “Surgeries that have a lack of surface area available to warm have higher rates of hypothermia and require special attention. Under-body and over-body warming simultaneously will always be more effective than under-body or over-body warming individually.”
Burlingame did point out that “during some procedures only certain parts of the body are able to have the contact required with the warming device. Example: A patient is having a procedure in which the majority of their body is exposed. They would benefit from an under-body warming device rather than one that is applied over the top of the body.”
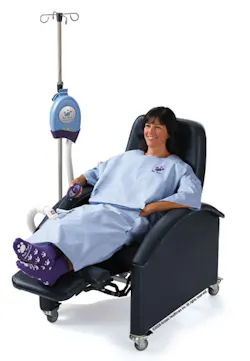
Kent Ellis, Principal, Pintler Medical, maker of another patient warming and pressure reduction system, says effective temperature management hinges on warming as much of the body’s surface area as possible. “Successful warming is about interface; if the skin is broadly infused with warming then the outcomes are better,” asserted Ellis, who expressed great confidence in his product’s capabilities. “Pintler warms and delivers pressure reduction to every patient every time. No airborne exhaust or new cleaning technique is required. This really is a care provider-designed product. It is what you want your mom to have during surgery.”
Conductive v. convective
One of the more publicized and heated arguments going on right now is between forced air warming (FAW) manufacturer 3M Health Care and Augustine, which is somewhat ironic since Augustine also invented 3M’s Bair Hugger patient warming system more than 25 years ago. He says the system, despite being the most widely used patient warming method today, is not the best or safest way to prevent hypothermia.
“A study of nearly 60,000 patients who were warmed with forced-air at the Cleveland Clinic showed that hypothermia was common and prolonged—with nearly 50 percent of patients hypothermic two hours after induction,”1 said Augustine. “With hypothermia rates that high, all warming protocols need to be re-evaluated — because 50 percent hypothermia is simply a failure.”
He also contends that FAW puts some surgical patients at risk of developing SSI, particularly those undergoing orthopedic and cardiac procedures. “Forced-air warming systems are a proven vector of airborne contamination and have been linked to higher infection rates in total joint surgery,” Augustine said. “Any patient receiving implanted foreign material is at increased risk of infection from airborne contamination and should be warmed with an air-free system.”
Although some research supports the idea, some also fails to confirm a direct correlation between FAW and infection.
For example, the authors of a study published in The Journal of Bone & Joint Surgery concluded: “Forced air warming significantly increased the number of airborne particles over the surgical site compared to the radiant warming or the control, both of which showed similar results. Bacteria require particles to transport them, and although we are unable to confirm if any of the particles were transporting bacteria, the significant increase in the number of particles that we found in this study at the surgical site is of concern.”2
Al Van Duren, Director of Scientific Affairs and Education for 3M’s patient warming business, upholds the safety and reliability of the Bair Hugger product line. “The dominance of the Bair Hugger system is the result of decades of basic physiologic and clinical research coupled with a deep and ongoing partnership with our customers,” he asserted. “We were the first to recognize the importance of jet impingement and its accentuation of convection. The Bair Hugger brand has been the source of every major innovation in this field. 3M has produced a compendium of more than 170 research papers in which the Bair Hugger system was used. The compendium is a comprehensive book that includes citations without regard to outcome and includes a brief summary of each paper with URL links to paper abstracts.”3
Now facing dozens of lawsuits from orthopedic surgery patients who claim the Bair Hugger caused them to develop serious deep-joint infections, 3M continues to challenge studies or competitor claims linking SSI to FAW. “Researchers John P. Abraham, PhD, Professor of Thermal Sciences at the University of St. Thomas, and Jennifer A. Wagner, PhD, Prism Environmental Health and Safety Solutions, recently released the results of a study, which found that the Bair Hugger system did not disrupt clean operating room airflow and did not move air from the floor to the surgical site,” stated an online article posted by 3M in July.4
Making a choice
Strongly opposing studies and opinions have the potential to confuse healthcare providers and purchasing managers who just want accurate, dependable information.
“There is a vast amount of conflicting evidence in the literature, so it’s common that [clinicians] talk about how to best keep the patient warm and how to do it safely,” said Burlingame.
So how do end-users make sense of the competing data?
Burlingame referred to AORN’s guideline for preventing unintentional hypothermia, which was updated last November. “As stated in the guideline Recommendation III.a.1: ‘The method of warming should be selected based on the planned procedure, patient positioning, IV access sites, and warming equipment constraints (e.g., access to the surgical site, skin surface area contact).’ When a facility is looking at device options they should look at the needs of their patients and from that determine the devices needed. In many situations more than one device may be required. The nurse now has the ability to choose the product that is best for the patient and not just the one product that is available. In this, it’s good news we have these alternatives.”
Van Duren said facilities need to scrutinize the research that’s presented very carefully and be mindful of any conflict of interest statements which could indicate bias. “The best way to make sense of the clinical literature is to become a critical reader of it,” he said. “Also, don’t be misled by poorly drawn (or missing) graphs or statistically significant findings that have no clinical relevance. Probably the biggest mistake in the patient warming clinical literature is the failure to analyze temperature data correctly — many studies compare end-of-procedure temperatures in groups of patients without correcting them for the very large differences in procedure times for the patients.
“With respect to comparative studies in patient warming, pay close attention to things like the selected operating temperature of the devices — in some studies conductive warming systems are operated at a higher temperature than the forced-air systems, or the number of devices used per subject — two conductive blankets compared to a single forced-air warming blanket,” Van Duren cautioned. “Admissions like these suggest an intentional or unintentional bias on the part of the investigators that will be noticed only by critical readers.”
Augustine suggested facilities take a hands-on approach to finding out what works. “Compare the technologies for yourself! Do an evaluation of your current warming outcomes and compare that with products that you evaluate,” he said. “Understand that there will always be some amount of hypothermia, but it should be less than 10 percent of patients rather than over 30 percent. Clinicians will be surprised to learn that what they’re currently doing to combat hypothermia is not nearly good enough.”
Ellis believes previous healthcare reimbursement policy influenced the popularity of forced air systems. “FAW was validated during a time of ‘Cost-Plus reimbursement’ [and] that era has ended,” said Ellis. “When making a decision on patient care and safety that ideal setting is simplicity and the use of a single approach that is provided to every patient, not just a percentage of the population. FAW’s history is utilization in cases over one hour, this is due to the old ‘Cost-Plus” reimbursement era. Procedures under one hour were not reimbursed as FAW was not effective. While in the same vein we know that most thermal loss is in the first hour. We are in an arena now where the “old practices” of Cost-Plus reimbursement and Cost-Plus care have ended. Fixed cost is being used as leverage by Medicare to drive compliance to quality of care measurements. This is new for many, including surgeons.”
Looking ahead
So what does the future hold for patient warming?
Burlingame couldn’t say for sure, noting that while AORN monitors changes and developments constantly, he wasn’t aware of anything new as of late.
Van Duren said the dramatic decreases in surgical duration for many common procedures will drive changes in the way patients are warmed. “As surgical times decrease, there simply isn’t time to re-warm patients to normothermia intra-operatively, so there will be considerably more emphasis on pre-warming and ways to make it easier and more efficient,” he said. (See Pre-warming as a prerequisite.)
Convinced FAW is on its way out Augustine highlighted select statements made by the Centers for Disease Control and Prevention (CDC) concerning the relationship between heater-cooler units and bacterial transmission during cardiac surgery. “The CDC-published Emerging Infectious Diseases Journal, while noting that research has not yet been done to definitely link forced-air devices to specific infections, concluded: ‘Our evidence also highlights the risks associated with devices that generate airflows in the operating room and that were not part of the original operating room air management design. Until more detailed evidence is available regarding this issue…devices that generate drafts should be banned from the operating room.’5 The research is showing that air-free warming is safer for high-risk locations. It’s time to be proactive before you are forced to be reactive,” he said.
Ellis feels similarly. “Conductive warming will capture the OR suite due to simplicity and economics. Clinicians are seeking safe and consistent performance,” he said, noting that those held responsible for keeping patients in normothermia is changing too. “Patient warming is moving with some speed from the world of Anesthesia to Nursing. During the Cost-Plus reimbursement era Anesthesia was given thermal regulating and FAW. In the next five years thermal regulating and quality will be owned by Nursing.”
See sidebar: Pre-warming as a prerequisite
References
1. 1. Sun, Z., et al., Intraoperative Core Temperature Patterns, Transfusion Requirement, and Hospital Duration in Patients Warmed with Forced Air. Anesthesiology. 2015. 122(2): p. 276-285.
2. https://bdhmedical.nl/website/wp-content/uploads/2013/09/JBJS_publicatieFEB2012.pdf.
4. 3M Bair Hugger System Research Compendium: http://safety.3m.com/Compendium.
5. Sommerstein R, Rüegg C, Kohler P, Bloemberg G, Kuster SP, Sax H. Transmission of Mycobacterium chimaera from heater—cooler units during cardiac surgery despite an ultraclean air ventilation system. Emerg Infect Dis. 2016 Jun [date cited].
About the Author

Valerie J. Dimond
Managing Editor
Valerie J. Dimond was previously Managing Editor of Healthcare Purchasing News.