While this year marks the 20th anniversary of the Needlestick Safety and Prevention Act (Pub. L. 106-430) being signed into law, sharps injuries are still a significant threat to healthcare workers. According to the Centers for Disease Control and Prevention (CDC), hospital-based healthcare personnel experience approximately 385,000 needlesticks and other sharps-related injuries each year, putting them at risk for exposure to bloodborne pathogens such as hepatitis B (HBV), hepatitis C (HCV) and human immunodeficiency virus (HIV).1
The advancement of sharps injury prevention devices has reduced the number of injuries over the past two decades, with the greatest reductions occurring in the categories of disposable syringes and winged steel needles (butterflies). Although injuries still occur when using devices designed for safety, with many occurring before the user activates the safety feature.2
Manufacturers continue designing new sharps devices for greater ease of use, effectiveness and safety. In this article, we provide insights from some of these companies on recent design advancements, and highlight new products aimed at protecting healthcare workers and patients.
The evolution of sharps safety regulations, standards and guidance
Regulators, manufacturers, industry associations, healthcare organizations and individual health practitioners all recognize the risks of using sharps devices. Over the past 20 years, various groups have taken action to help protect healthcare workers and patients against sharps injuries and potential pathogen exposure.
OSHA’s Bloodborne Pathogens Standard
In 2000, in response to the growing problem of accidental sharps injuries in healthcare and other occupational settings, Congress mandated a modification to OSHA’s Bloodborne Pathogens Standard (29 CFR 1910.1030) to provide greater detail around OSHA’s requirements for employers to identify, evaluate and implement safer medical devices. This included requirements for employers to maintain sharps injury logs and involve non-managerial healthcare workers in evaluating and choosing devices.3
While OSHA’s original 1991 Bloodborne Pathogens standard included the requirement for employers to implement safer medical devices, the revised 2000 standard, which took effect on April 18, 2001, further clarified the definition of “engineering controls” related to safety devices. OSHA defined these controls as those “that isolate or remove the bloodborne pathogens hazard from the workplace,” including sharps disposal containers, self-sheathing needles and safer medical devices, such as sharps with engineered sharps-injury protections and needleless systems.
Furthermore, employers must train employees with occupational exposure to blood and other potentially infectious materials (OPIM) on the proper use of all engineering and work practice controls; and provide personal protective equipment (PPE), such as gloves, gowns, eye protection and masks.
American Nurses Association (ANA) Position Statement
In 2012, more than a decade after the revision of OSHA’s Bloodborne Pathogens Standard, the American Nurses Association (ANA) and 18 other nursing and health care organizations endorsed a new position statement “aimed at moving the debate about sharps safety forward and prompt further, tighter legislation.”4
The International Healthcare Worker Safety Center at the University of Virginia developed the statement, entitled, “Moving the Sharps Safety Agenda Forward in the United States: Consensus Statement and Call to Action,” which described five key areas to further reduce the risk of sharps injuries to healthcare workers.5
1. Improving sharps safety in surgical settings: Recommendations include developing a site-specific sharps safety policy for the OR mandating the availability, training and use of specific sharps safety devices and implementation of risk mitigation strategies outlined by the American College of Surgeons (ACS) and the Association of peri-Operative Registered Nurses (AORN).
2. Understanding and reducing exposure risks in non-hospital settings: Recommendations include the collaboration of professional organizations and medical product distributors for non-hospital care settings in making sharps safety a priority; and ensuring the availability of appropriate devices and educational and training materials targeted at workers in these settings.
3. Involving frontline healthcare workers in the selection of safety devices: Recommendations include employers enlisting frontline workers in regular and systematic assessment of the devices currently in use in their institution, to ensure such devices are appropriate and, in OSHA’s words, “eliminate or minimize employee exposure” to the “lowest feasible extent.”
4. Addressing gaps in safety devices: The need for continued innovation: Recommendations include professional organizations partnering with device manufacturers to assess and prioritize device needs for specific clinical applications; and manufacturers partnering with surgeons and surgeon’s groups to develop suture- and scalpel-safety designs that both reduce risk and are comfortable and intuitive for surgeons to use.
5. Enhancing education and training: Recommendations include employers providing instruction on an annual basis for all potentially exposed clinicians and other workers (including service workers and purchasing agents) on the appropriate use and disposal of safety devices that are available in their facility. Employers, professional educators, manufacturers and employee representatives should collaborate to develop training strategies that can be widely applied when new devices are introduced, so that frontline healthcare workers know how to properly use and dispose of them.
U.S. Pharmacopeia (USP) General Chapter <800>
According to the CDC, about eight million U.S. healthcare workers are potentially exposed to hazardous drugs (HDs), including those used for cancer therapy, some antiviral drugs, hormone agents and bioengineered drugs. While the CDC notes that inhalation and skin contact or absorption are the most likely routes of exposure, unintentional ingestion from hand to mouth contact and unintentional injection through a needlestick or sharps injury are also possible.6
In 2019, the U.S. Pharmacopeia (USP), developed a general chapter specific to the handling of HDs, USP General Chapter <800> Hazardous Drugs—Handling in Healthcare Settings, which is designed to further minimize the risk of exposure to HDs through safe handling practices.7
USP 800 includes responsibilities of personnel handling hazardous drugs; facility and engineering controls; procedures for deactivating, decontaminating and cleaning; spill control; and documentation. As of December 1, 2019, USP recommends those facilities handling HDs comply with these revised standards.
In its February 7, 2020 regulatory advisory, the American Hospital Association (AHA) voiced its support for implementation of the USP 800 standards:
“Protecting health care personnel from harm resulting from occupational exposure to environmental hazards is a top priority for hospitals and health systems, and implementation of these standards will play a critical role in keeping providers and the patients they treat safe.”8
Sharps injuries: Still a significant risk
Even with stricter standards intended to reduce sharps injuries among healthcare workers over the past 20 years, a significant number of injuries still occur in U.S. hospitals.
In the latest EPINet Report for Needlestick and Sharp Object Injuries, 34 U.S. hospitals reported 1,175 injuries between January 1, 2018 and December 31, 2018.9 Those sharps products most associated with injuries were suture needles (290 injuries/25% of total reported) and disposable syringes (282 injuries/24% of total reported).
The vast majority of cases occurred with a contaminated sharps item (1,055 injuries/90% of total reported), with 63 percent having visible blood on the device. Most injuries occurred in operating rooms (OR)/recovery areas (44%) followed by patient rooms/ward (22%). In the majority of cases (70%) the injured worker was the original user of the sharp item, and the injury occurred during use (55%).
Sharps injuries still occur when healthcare workers use devices designed for safety. Among the injuries reported to EPINet during 2018, 34 percent were caused by a needle or sharp medical device with a safety design (e.g. shielded, recessed, retractable, or blunted needle or blade). When asked if the safety mechanism was activated at the time of injury, 32 percent of those reporting said the safety feature was either partially (23%) or fully (9%) activated.
New products designed for greater safety
Like all areas of healthcare, sharps injury-prevention devices continue to evolve with more advanced features, and to address previously unserved application areas. Below are some of the latest technologies and products intended to improve healthcare worker and patient safety.
B. Braun’s catheter systems
The ACCEL Valved Safety Centesis Catheters and Procedure Kits are designed to help clinicians comply with recommendations for preventable medical error reduction, sharps safety and infection prevention. The centesis needle is a safety engineered device with an automatic needle safety shield that is most effective for needlestick injury prevention. It is integrated with a fluid/air stop, self-sealing valve located in the catheter hub for automatic containment of patient drainage fluid and reduced risk of pneumothorax after needle removal. This provides a safe, closed catheter system during clinical use.
The ACCEL 600mL, 1,000mL and 2,000mL Evacuated Drainage Bottles are shatterproof, light weight, clear plastic bottles that provide containment of bio-hazardous fluids. These bottle are safe and secure, luer lock, needle-free access.
The ACCEL Connection Sets kink-resistant tubing provides a safe and secure luer lock connection containing biohazardous fluids during drainage. Closed male luer sets provide for a safe and secure closed system during evacuated bottle exchanges.
“The safety of our clinicians and the patients they serve drove our development of these products due to the prevalence of needlestick injury,” said Valerie Shively, Marketing Associate, B. Braun Interventional Systems. “With our products, we aim to manage the risk of bloodstream infections, maintain a sterile field, and reduce waste and control costs by having all components together in one convenient kit.”
Cardinal Health’s needleless cannula technology
The Cardinal Health Monoject SmarTip needleless cannula addresses all three of these factors:
- Clinician safety: Needleless plastic cannula helps prevent accidental needlesticks.
- Patient safety: Anti-coring design reduces vial coring and the chance of drawing particulate matter along with medication.
- Efficiency: A 16g flow rate allows for quick and easy draws, even for viscous fluids.
- User acceptability: SmarTip is designed with side aspiration eyelets, which make it easier to access all medication in a vial without having to manipulate the cannula when drawing up.
IntegriMedical’s needle free injection technology (NFIT)
“Needle free injections technology (NFIT) is the emerging innovation to address the risks associated with needlestick injuries (NSI),” said Lois Wedlock, Director Clinical Excellence, Needle Free Solutions and Training. “This technology eliminates all NSI because there is no needle, it is more comfortable to the patient and easy for the healthcare professional to administer the injection. The shields, sheaths and retractors still have a needle; therefore, NSIs can still occur. The NFIT has zero NSI incidents.”
Wedlock points out how NFIT technology could help with wide-spread administration of a future COVID-19 vaccination. She states:
“The new mRNA candidate vaccines require more force and technique than a needle and syringe can offer. NFIT ensures a consistent dose is administered at the proper depth of penetration every time and reduces the incidence of repetitive stress injury to the healthcare professional. The supply of needles and syringes may be scarce with the expected vaccinations being administered in the coming months and having another option may offer relief to the supply chain.”
“Furthermore, with the current pandemic, healthcare cannot afford to have distracted workers wondering about their own health status with NSI, whether it be an overworked nurse injecting a patient who accidently gets stuck, to a housekeeper getting stuck from a needle while handling the bed linens,” Wedlock added.
Mölnlycke’s double-gloving system
While double gloving with synthetic gloves are an evidence-based solution that can effectively decrease pathogen transmission and have become the standard of care in many hospitals, there have been cases where wearers suffer skin sensitivities to the accelerators used to manufacture them. Therefore, to be accepted, the system design must take into account staff desire for comfortable fit, good tactile feel and skin sensitivity needs.
“For the OR, securing the best double gloving system is critical and usage is driven by comfort, quality and a culture of safety,” said Calabrese. “Using a just culture model, staff shares accountability and control for best practices, such as double gloving. This approach takes a step beyond dogma and places the outcomes for safety on education and actual practice using a synthetic double-gloving indicator system.”
The new Mölnlycke Biogel PI UltraTouch S double-gloving system, made with a skin-friendly formula, is designed to reduce the risk of Type IV allergic contact dermatitis. The best-in-class puncture indication system ensures breaches are spotted quickly.
One medical center reported a 31 percent decrease in needlestick injuries among staff members from 2018 to 2019 using a two-fold focus: Gain double gloving acceptance using an indicator glove and transition to a latex-free environment. 11
Owen Mumford’s safety pen needles
“First generation safety pen needles have played a significant role in the protection of health workers by reducing the risk of needlestick injuries,” said Lee. The use of safety pen needles has helped to reduce the occurrence of needlesticks each year, which results in reduced exposure among health workers and patients to disease from contaminated sharps, however, problems still exist. In response, Owen Mumford developed the next-generation safety pen needle that offers dual-protection covering both ends of the needle, protecting both the patient and the healthcare professional.”
Retractable Technologies’ retractable needle technology
“RTI appreciates and respects the challenges of the healthcare environment,” said Duesman. “The COVID-19 pandemic has illustrated the importance of protecting healthcare workers, as well as the need for a robust, U.S.-based medical device industry. All of our products are designed to allow for safe and efficient use for the caregiver, the patient and the community-at-large. It is important to note that RTI’s safety-needle products prevent both needlestick injuries and reuse, which can contribute to the spread of bloodborne pathogens associated with medical devices.”
RTI’s latest commercially available innovation is the EasyPoint retractable needle. This needle is compatible with luer-fitting syringes and allows for pre-removal activation. It features a unique activation mechanism that eliminates forward motion, allowing users to keep their fingers behind the needle. According to Duesman, the safety and efficacy of activating a safety mechanism before removal from a patient is well established. Pre-removal activation virtually eliminates exposure to a contaminated needle, thereby effectively reducing the risk of a needlestick injury. VanishPoint automated retraction syringes have demonstrated significant needlestick reduction, as compared to manual devices that require removal from the patient prior to activation.
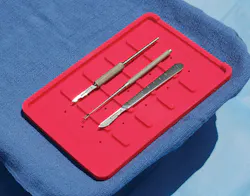
Viscot Medical’s neutral zone trays
“Surgeons are the most likely to get stuck in the OR according to AST-provided statistics, the first scrub is the second most likely,” said Nina Morales, Marketing Associate, Viscot Medical. “Our goal was to create a simple solution that enforced already existing safety recommendations.”
“Soffzone was developed by a surgeon who was frustrated by the lack of safety enhancements in the OR,” explains Morales. “His feedback directly drove the development of this product. The bright red color was influenced by him wanting to keep his eyes on the surgical site but knowing where the sharp was in his periphery vision, and the low profile for complete visibility of the sharp. The size was so he could keep it easily accessible on the mayo stand. Every detail was made with comfort and safety in mind.”
“We recently validated different sterilization methods for the Soffzone and updated the IFU to reflect that,” Morales added. “Many facilities have begun sterilizing the Soffzone in their kits to help drive compliance across the board.”
References:
1. Sharps Safety for Healthcare Settings, CDC, https://www.cdc.gov/sharpssafety/index.html
2. Stop Sticks Campaign, National Occupational Research Agenda (NORA), https://www.cdc.gov/nora/councils/hcsa/stopsticks/sharpsinjuries.html
3. OSHA, https://www.osha.gov/needlesticks/needlefaq.html
4. Safe Needles Save Lives, American Nurses Association (ANA), https://www.nursingworld.org/practice-policy/work-environment/health-safety/safe-needles/safe-needles-law/
5. Moving the Sharps Safety Agenda Forward in the United States: Consensus Statement and Call to Action, American Nurses Association (ANA), https://www.nursingworld.org/~4afba4/globalassets/practiceandpolicy/health-and-safety/consensusstatement-sharpssafety.pdf
6. Safe Handling of Hazardous Drugs, CDC, May 21, 2014, https://blogs.cdc.gov/niosh-science-blog/2014/05/21/hazardous-drugs/
7. USP General Chapter <800> Hazardous Drugs—Handling in Healthcare Settings, USP, https://www.usp.org/compounding/general-chapter-hazardous-drugs-handling-healthcare
8. USP Chapters <797> and <800> New and Revised Compounding Standards, American Hospital Association (AHA), February 7, 2020, https://www.aha.org/system/files/media/file/2020/02/usp-chapters-797-and-800-new-and-revised-compounding-standards-3_1.pdf
9. EPINet Report for Needlestick and Sharp Object Injuries, July 2019, https://internationalsafetycenter.org/wp-content/uploads/2019/07/Official-2018-US-NeedleSummary-FINAL.pdf
10. Occupational Safety and Health Administration Standards, revised Bloodborne Pathogens and NeedleStick Prevention Standard requirements (effective date April 18, 2001).
11. 2020 AORN Bassett Medical Center poster
About the Author
Kara Nadeau
Senior Contributing Editor
Kara Nadeau is Sterile Processing Editor for Healthcare Purchasing News.