From IV drips to container ships
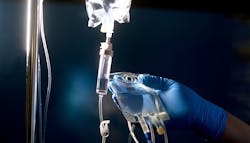
During the earliest months of COVID-19’s incursion into the U.S., a dramatic shortage of both clinician time and personal protective equipment (PPE) created a new hospital practice: Moving intravenous infusion pumps out of patient rooms and into hallways.
The hallway move allowed nurses to check patients’ solution levels, medication dosing, and to change IV bags without donning and doffing new PPE sets each time. And, of course, reducing in-person patient checks minimized clinicians’ risk of exposure to the virus.
But making the change from bedside to hallway required a key fix.
“They needed longer tubing; they needed an extension line,” said Steve Weber, Director of Marketing Vascular Access & IV Systems at B. Braun Medical.
Creating a new – albeit fairly simple -- product that B. Braun hadn’t made before would normally take six to eight weeks from conception to market, Weber said. But company leaders, in an effort to quickly fill a critical void in hospital systems, took an all-departments-on-deck approach. B. Braun’s engineering, regulatory, operations, manufacturing, marketing and sales departments became part of the expedited process.
“All those players had to come together,” Weber said. “It required us to challenge some of our own internal systems, but we got it to inventory in just two weeks.”
B. Braun was able to help alleviate a shortage and create a new product for itself in one move, in spite of COVID-related challenges.
To manufacture the product, worker masking had to be instituted, and barriers had to be erected to make sure operators could maintain a proper distance from one another. Producing just about anything during a pandemic, after all, requires a lot of new considerations.
B. Braun’s reach, which includes operations on every continent but Antarctica, helped make the project possible.
“We have good access to supply (of materials) and we have good supply chain relationships,” Weber said. It didn’t hurt either that the company has manufacturing plants in the U.S., and that they are strategically spread out: Allentown, PA, Irvine, CA and Daytona Beach, Fl.
Michael Schiller, Senior Director of Supply Chain for the Association for Health Care Resource & Materials Management (AHRMM) would like to see this kind of flexibility from manufacturers, vendors, buyers and everyone else on the supply chain. He and other industry leaders have studied fundamental issues laid bare by COVID, and are making recommendations for industry-wide change.
“We have a geographic concentration of manufacturers – no doubt about it,” he said, pointing to one key source of trouble for the industry. “How do we best diversify? Bringing all manufacturing to the U.S. is unrealistic and not possible.” Right now, interests lie almost entirely in Asia. “But how do you build an infrastructure in other places to manufacture these products? It’s very complex.”
Now, as the Delta variant is waning and operating rooms are scheduling patients once again, the after-action review has begun. Schiller and other supply chain leaders have observations, studies and takeaway messages to share about the industry’s responses to COVID-19. They have identified and deconstructed some of the root causes for medical supply shortages, tallied the exorbitant human and financial costs that have resulted, and built a series of recommendations for the healthcare supply chain moving forward.
“When you peel those layers of the onion back, there’s a lot to this,” he said.
Surviving and thriving
Thus far, individual businesses have been working with the hand that COVID has dealt them. Each has had to make decisions based on individual strengths, resources, immediate circumstances, and both short and long-term predictions.
“Surgery centers were down for most of 2020, so we focused our priorities differently,” B. Braun’s Steve Weber said. “We weren’t going to build every product that we usually do.” This allowed the company to invest resources elsewhere.
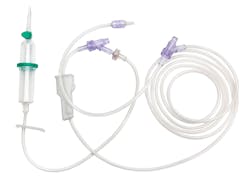
B. Braun recently debuted its CARESAFE IV Administration Set. The system includes a unique, optional AirStop feature. A version of the product has already been successful in Europe.
When an IV bag is empty, “air can eventually get into the IV tubing line if the clinician doesn’t stop the infusion,” Weber said. “It’s all a timing game.” The clinician must take time to remove the air so it doesn’t get into the patient. “They’re constantly checking and then having to get the air out if it gets into the IV line.”
The product is designed to remove risks to the patient.
“The AirStop prevents air from getting into the IV line,” Weber said, “so it helps streamline the workflow for nurses and helps keep patients safe.” And employing the device, he said, “helps stressed clinicians so they can stop worrying about the IV and focus on value-added care.”
At ivWatch, a smaller and very different kind of enterprise, Jaclyn Lautz, Ph.D., Chief Operating Officer, said her company made an unexpected move in response to the marketplace effects of COVID. Like Weber, she said her company was spared many of the woes visited upon the industry due to the fact that it manufactures products here in the U.S.
“This mitigated most of the supply chain and manufacturing issues hitting the market hard during this time,” Lautz said.
The unique product for which her company is named uses technology to monitor a patient’s IV site, “to catch infiltration and extravasation events early,” she said.
According to a description of the product, ivWatch employs, “a miniaturized biosensor that uses visible and near-infrared light to measure changes in the optical properties of tissue near the IV insertion site.”
The sensor is placed next to the peripheral IV site on the patient’s wrist, forearm, hand, foot or scalp, etc. There, the ivWatch technology continuously measures volume changes to the tissue fluid. When it detects changes indicating that IV fluid is leaking and pooling in the tissue, it prompts an alarm that can be both heard and seen.
“Getting an IV is still one of the most common procedures performed in a hospital, and even the most perfectly placed IV can fail,” Lautz said. “With the current workload for clinicians, they need all the support they can get with things like technology that will help improve patient outcomes.”
But like many businesses whose operations slowed due to COVID-19, ivWatch has used some of its manufacturing capabilities to produce something for which the pandemic has generated high demand: respirator masks.
“Overseas, counterfeit N95s were flooding the marketplace. We knew we could leverage our supply chain connections and internal expertise to make a difference,” Lautz said.
The company converted some of its machinery at the company’s Newport News, VA facility to this new crisis-born enterprise.
“We are currently in the final stages of our NIOSH application and certification,” Lautz said. The product was third-party tested, she said, by Nelson Labs and Pacific Biolabs.
Sharing smart
At yet another point along the supply chain, Charlotte Perkins, Vice President of Supplier and Portfolio Management at Owens & Minor, said her company has had its own view of the landscape.
“Demand for IV catheters is increasing slightly at a time where there are minor shortages,“ she said. “We anticipate this being a short-term challenge and have been working with our customers to offer alternate products if needed.”
“We have only recently seen minor supply chain challenges with IV solutions,” she said, “compared to some other categories that were more directly affected due to COVID-19.”
Perkins said that what sets Owens & Minor apart from other companies grappling with COVID-19’s financial effects is tight control and visibility over their supply chain. They have been able to supply customers with PPE, she said, “because we already have vertical integration of our supply chain for these critical products through our Americas-owned and operated manufacturing facilities.”
Owens & Minor has a product that Perkins said speaks to the company’s focus on communication and transparency. Her clients can subscribe to alerts, via the SMART Card (Supplier Metrics & Accountability Report Tracker).
“By subscribing to these alerts, healthcare facilities and systems gain access to weekly supplier snapshots and updates,” she said. The updates, “keep them aware of supplier constraints or disruptions.”
“We have a unique viewpoint regarding the state of the market, demand trends and the issues healthcare facilities may be experiencing related to outside factors, like COVID-19,” Perkins said.
Cause and effect
A “perfect storm” created by COVID, according to Schiller, actually began with some storm clouds that formed months earlier, thousands of miles away.
Annual Chinese New Year celebrations shut down business in that country for two weeks, and 2020 was no exception. Manufacturing there all but ceased.
“Then you began to see COVID spike there -- in the very same places where PPE products were manufactured, thereby reducing manufacturing output further,” Schiller said. Meanwhile, COVID was beginning its destructive journey around the world, ramping up demand for PPE everywhere. The same was true for many other medical products that are manufactured, or partly manufactured, in other Asian countries.
Weber said that even with B. Braun’s many global resources, not everything was smooth sailing when looking to produce IV tubing.
Storms that left Texas in a deep freeze back in February and tore up its coastline during hurricane season put Tyvek, the polyethylene product made by DuPont, in short supply. The material is used in making everything from HAZMAT suits to packaging materials. Tyvek could no longer be made in Texas, so that all-important resource became tough to access.
“So now, even the availability of packaging materials is strained,” Weber said, “not because of the pandemic but because of natural disasters.”
“That impacts what you produce, and the ripple effects go all the way to end users,” he said.
Some of the results can be seen in long lines of hulking container ships waiting outside of U.S. ports. The bullwhip effect, as supply tries in vain to catch up to demand, is not a pretty sight to anyone in the industry. A computer chip shortage, stemming partly from shortages of raw material, caused downstream shortages in many products that require the use of that chip, including medical devices like IV pumps.
All those product shortages have links to manpower shortages.
“Products might be sitting on a boat in San Francisco or San Diego, but there’s not enough people to unload them,” Weber said.
When they do manage to offload containers, “then you’re waiting for trucks to move the products because there’s a shortage of drivers.” Schiller said.
To mitigate the effects of the next pandemic, or cascade of disasters like those of the past two years, healthcare and supply chain leaders will need to embrace change in a number of areas. he said. A national, clinically acceptable products list should be developed, and a more open system that uses existing supply and distribution infrastructures. That way, resources can be allocated and shared when necessary.
“We need to improve transparency, but once the system is transparent, how do you manage human behavior?” he asked. For instance, when production and PPE inventories finally improved after devastating shortages, “Some hospitals spent tens of millions building PPE inventory so they wouldn’t run out again, Schiller said. Stockpiling can create shortages all over again.
Other changes Schiller urges for the system’s future health:
Hospitals will need to examine their purchasing habits. ...Single source contracts for a particular product may result in some cost savings, but might not be best in the long run.
“Let’s move away from where we’re ordering just in time so we’re all lean and mean,” he said. “If I’m looking to build redundancy and reduce risk in the supply chain, I’ll need more than one vendor, or a list of clinically acceptable substitutes.”
But there are always caveats.
“All these decisions and changes will come at a cost,” Schiller said. And the point person – the supply chain leader – will have a role that’s far more complex than it had been, pre-COVID.
“I need to have more visibility upstream – see what’s going on with manufacturers,” he said. “What’s going on logistically? What’s going on politically? I have to have a global picture now. I need to be much more strategic.”
In the meantime, Schiller’s keeping his eye on the future. “When the next spike occurs,” he said, “it starts all over again.”