Cutting time without cutting quality
For a New York City academic medical center, one minute of operating room (OR) time costs $150 according to a recent study.1 While the cost may be lower or higher for other healthcare organizations based on size and geographic location, time is money and healthcare providers can’t afford to waste it.
There are many factors that increase the time it takes to turnover an OR. There is the set-up and breakdown of equipment and medical supplies used in a procedure. Transitioning the patient out of the room at the end of the case takes staff time and effort. Then there is the time and labor necessary to clean and disinfect the wide range of potentially contaminated surfaces in the OR post-procedure.
Now more than ever, with health systems and hospitals attempting to recoup elective surgery revenue lost during the pandemic, OR teams need products and solutions to increase turnover efficiency in a safe and effective manner.
Education
Understanding what factors contribute to prolonged OR turnaround times is a first step in addressing them. Stephanie Nilan, Sr. Manager, Brand/Product Marketing, Healthcare Safety Solutions, Ansell, says the company recently introduced a new complimentary clinical program aimed at improving OR turnover efficiency and efficacy.
“AnsellAdvisOR is comprehensive, safety-focused program, conducted by experienced Ansell clinicians, including a baseline assessment of current practices, turnover time and cleaning effectiveness, a gap analysis against standards, and detailed recommendations for process improvements,” said Nilan. “The program is completely customizable and is tailored to meet the needs of any facility.”
COVID-19 pandemic challenges in staffing surgery centers and healthcare facilities may lead to the potential of suboptimal cleaning and disinfection of some ORs, according to Larinda Becker, Executive Director of Marketing - Infection Prevention, Diversey.
In response, the company has launched Diversey TurboTurn, a program to help OR teams improve the quality and efficiency of room turnover, for which Diversey has achieved the Association of periOperative Registered Nurses (AORN) Seal of Recognition. Becker describes how it works:
“The program begins with an assessment of goals and practices of the facility, then collaborates to optimize the selection of the right products, processes, etc. to address. We then work through a complete implementation plan to train and provide tools for success and validation. We have seen this not only reduce turnover time, but also improve the quality of cleaning and disinfection results.”
The program includes in-person and on-demand virtual training and Continuing Education Credits (CEUs) courses for staff members. Managers receive administrative dashboard training and work with Ecolab to customize reporting to best serve their needs and drive standardization. The training and cleaning processes in this program have been given AORN’s Seal of Recognition.
Cleaning and disinfection
In an AORN special report, AORN Guidelines in the Era of COVID-19, the organization defines the OR environment as “the area surrounding the patient, the patient themself, as well as any equipment or devices that we use on the patient.”2
“What can happen is when a healthcare worker touches that environment—in other words, the inanimate objects and the patient—then the pathogens are on their hands, and then their hands can transfer those pathogens to other surfaces or even to themselves (e.g., if they rub their eyes, nose, or mouth),” says Karen deKay, MSN, RN, CNOR, CIC, perioperative practice specialist and author of AORN’s Guideline for environmental cleaning.
Cleaning and disinfecting the OR environment is a tremendous responsibility that takes considerable time and labor even outside of a pandemic environment. Below are some ways equipment and supply manufacturers have innovated to boost productivity in this area.
Easy to clean surfaces
One way to reduce infection risk is to integrate ease of cleaning into the design of OR equipment. Smooth surfaces are far easier to disinfect versus those with edges, gaps and seams, which can harbor dangerous microbe, as cited by the Healthcare Surfaces Institute.3
A study published in the June 2020 edition of the American Journal of Infection Control compared an anesthesia machine with a conventional design (GE Aespire 7900) to one with a redesigned work surface (Dräger Perseus A500) for cleaning effectiveness.4
Both conventional and redesigned anesthesia machines were contaminated with fluorescent gel prior to set up and use in hip or knee surgeries. Following the cases, anesthesia residents cleaned the machine surfaces using disinfectant wipes in accordance with cleaning instructions provided to them. Researchers used fluorescence to compare cleaning effectiveness of both machine designs before and after set-up and use.
While the number of sites cleaned overall did not differ between the conventional and redesigned anesthesia machines, the redesigned work surface with smooth manual bag arm featured improved resident cleaning with surface disinfection wipes.
Cleaning between cases
Pressured with cleaning ORs in a rapid manner between patient cases, staff members tasked with this responsibility sometimes miss or inadequately disinfect high-touch surfaces and equipment. For between-case cleaning assurance, Diversey offers its UV-C disinfection device, MoonBeam3.
Becker says MoonBeam3 is a portable, powerful solution that disinfects quickly, reliably and responsibly. She notes how it is cost-effective and designed for fast disinfection of public and high-risk areas. The system offers three individually-adjustable arms that can be positioned at almost any angle, optimizing disinfection energy to allow dosing of both horizontal and vertical surfaces, in just three minutes.
“Many facilities are using MoonBeam3 to provide the added disinfection for the staff and patients, to reduce the risk from variability and comprehensiveness of cleaning,” she added.
To improve the efficiency of OR disinfection, SteraMist has launched SteraPak, a mobile disinfection system that the user wears like a backpack. The SteraPak contains SteraMist (iHP) technology which creates natural disinfection by using a low 7.8% hydrogen peroxide solution. It passes through a cold plasma arc creating hydroxyl radicals that penetrate the interior of pathogens to inactive viruses and kill bacteria spores on contact.
“Providing a quick disinfection with no ‘wet’ contact time and classified as only an irritant, provides reassurance that SteraMist disinfection is far superior to toxic and damaging chemicals. It can be used on sensitive equipment, including electronics, without leaving any residue and byproducts behind,” she added.
SteraMist is the first EPA-registered hospital-healthcare disinfectant system and solution. It is registered and listed for pathogens such as C. diff spores, Norovirus, Ebola, Avian Flu, coronavirus and more.
Nightly terminal cleaning
As Alice Brewer, Director of Clinical Affairs, Tru-D SmartUVC, explains, the use of UVC light for end-of-night terminal cleaning helps ensure the OR is as germ-free as possible for the following day, without adding to turnover time between patients.
In a study published in the American Journal of Infection Control, Tru-D was shown to reduce bioburden on anesthesia workstations. In the study, UVC disinfection greatly influenced bioburden reduction regardless of room size and exposure type. All trials, compared with the controls, exhibited a bioburden reduction of more than 99%. The research team went on to suggest that the Tru-D technology is an important supplement to the manual cleaning process.5
“Halosil’s touchless system saves labor, ensures no surface is left unreached as is often the case with manual or electrostatic spray methods, and does not expose staff to harsh chemicals. Hydrogen peroxide based HaloMist disinfectant is fogged using the HaloFogger to achieve an EPA registered sporicidal kill on all treated surfaces without wetting. So the no-wipe, no rinse residue free treatment has excellent compatibility with surfaces and sensitive electronic equipment in the OR.”
Kits, packs and trays
Another solution to OR turnover challenges is to have everything needed, pre-packaged, all in one place. Ansell’s STAT-PAC Room Turnover Kits help improve OR turnover efficiency by providing all of the items needed to set-up the OR for the next procedure including table linens, patient straps, positioners, bags, mops, wipes and more.
“Having these items conveniently packed together reduces the amount of time spent gathering supplies during room turnover,” said Nilan. “The cost per OR minute ranges from $29 to $80,6 so hospitals are always trying to find ways to reduce turnover time without compromising cleaning effectiveness.”
Nilan notes how Ansell’s STAT-BLOC disposable linens further enhance the OR turnover process by providing both complete barrier protection to help reduce the amount of strike-through contamination to the OR table, as well as antimicrobial protection to help ensure a clean patient surface is maintained.
“Studies show that even when using disposable, impervious linens, bacterial migration can occur from the OR table to the patient surface of the linens, however, with antimicrobial linens bacterial migration is prevented,” said Nilan while citing the results of a bacterial migration study.7 “Our STAT-BLOC linens with AMT Antimicrobial Technology are proven at least 99% effective against MRSA, E. coli, CRE and COVID-19.”
The program offers industry benchmark analytics and a turn-key conversion process supported by an expert clinical OR assessment team. Benefits include pack efficiency improvements and optimization, waste reduction and cost savings.
Owens & Minor’s SurgiTrack is a comprehensive clinical supply delivery service that delivers ready-to-use custom surgery packs directly to the OR. SurgiTrack improves efficiencies and lowers costs, ultimately helping to reduce OR turnover time.
Fewer instruments in the room
One way to reduce the amount of time required for OR turnover is to reduce the number of instruments in a case. The greater the number of instruments and trays, the longer it takes OR staff to set up, count items (before and after the procedure) and prepare them for the Central Service/Sterile Processing & Distribution (CS/SPD) department (e.g., pre-treatment, safely storing items for transport, etc.).
STERIS removes over 3,000-5,000 instruments from active inventory for its typical customers in the first set of service lines at a hospital, which results in a substantial reduction in sterile processing burden and meaningful overall efficiency improvements.
For those instruments used in a case, rapid turnaround by the CS/SPD team is often reliant on proper pretreatment of soiled items by OR staff post-procedure. Delays in transporting soiled instruments from the OR to the CS/SPD department are not uncommon, and instrument sets may sit for hours before being decontaminated in a high-volume facility. Without pretreatment, bioburden is left to dry and harden on instruments, making it more difficult and time-consuming for CS/SPD staff to clean them.
“This highly concentrated enzymatic formula provides a thick layer of dry-resistant precleaning gel that effectively breaks down and lifts protein-based bioburden from all instruments, scopes and non-porous surfaces,” comments David Willoughby, Vice President, Marketing & Business Development, Medtrica Solutions.
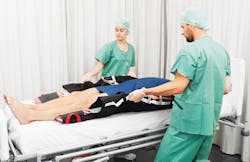
Patient transfer
When considering all of the factors that influence OR turnover time – the space, the equipment, instruments - efficiency often comes down to the human element – the OR team and their workflow. At the end of a procedure, OR staff members must transition the patient but do so in a manner that protects both the patient and the caregiver.
The Mölnlycke Tortoise Turning and Positioning System is designed to make it easier for staff to move patients safely into position with less physical exertion – and it’s proven to reduce caregiver back injuries related to patient turning and repositioning. The Tortoise can be used to transfer hospitalized patients from the OR back to bed for those who will continue to use the Tortoise over the course of their hospital stay.
The Tortoise system includes a positioning mat with a low-pressure air chamber designed to adapt to the patient by positive air displacement. The low-friction mat is fitted with ergonomic handles on both sides, helping caregivers to maintain proper body mechanics as they turn the patient. The system is equipped with Mölnlycke Z-Flo Fluidized Positioners, which allows staff members to achieve and maintain the right therapeutic position for each individual patient.
Conclusion
In today’s value-based care environment, health systems and hospitals face the constant struggle of providing the best care and outcomes to the patient while maintaining a profit margin large enough to remain viable.
As the revenue-generating heart of any healthcare organization, the OR should be the target of initiatives aimed at boosting procedural volumes in a safe manner. OR teams, value-analysis committees, supply chain professionals and other stakeholders have an increasingly varied selection of choices when it comes to product and solutions to help in these efforts.
References:
1. Improving Operating Room Turnover Time in a New York City Academic Hospital via Lean, The Annals of Thoracic Surgery, January 7, 2019, https://www.annalsthoracicsurgery.org/article/S0003-4975(19)30002-5/fulltext
2. AORN Guidelines in the Era of COVID-19, AORN Journal, March 1, 2021, https://aornjournal.onlinelibrary.wiley.com/doi/10.1002/aorn.13331
3. Healthcare Surfaces Institute, https://www.healthcaresurfacesinstitute.org, accessed January 11, 2022
4. Eli Schmidt, Franklin Dexter, Jacob Herrmann, Joshua D. Godding, Brent Hadder, Randy W. Loftus, Assessment of anesthesia machine redesign on cleaning of the anesthesia machine using surface disinfection wipes. American Journal of Infection Control, Volume 48, Issue 6, 2020, 675-681. https://www.sciencedirect.com/science/article/abs/pii/S0196655319308521
5. Nottingham, M., et al (2017). Ultraviolet-C as a means of disinfecting anesthesia workstations. American Journal of Infection Control. 45(9):1011-1013.
6. What does one minute of operating room time cost? Journal of Clinical Anesthesia, 2010, https://ether.stanford.edu/asc1/documents/management2.pdf
7. Clinical Relevance Testing Report: An evaluation of bacterial migration from a contaminated surface to a patient surrogate with the use of a variety of table covers, Palm Medical Solutions, April 9, 2015, https://www.ansell.com/-/media/projects/ansell/website/image-teaser/stat-bloc/clinical-abstract---bacterial-migration-from-contaminated-surface-to-patient-surrogate_versionb.ashx?rev=7110dbaf4e6347b894977c5a8c70634e&hash=476EDB135600AE53E2606AE037DF20B6
About the Author
Kara Nadeau
Senior Contributing Editor
Kara Nadeau is Sterile Processing Editor for Healthcare Purchasing News.