Healthcare delivery varies widely by location of care, condition, clinician, treatment and patient. There is no “one-size fits all” approach. This also applies to the type of medical equipment and supplies used in the course of care.
Pandemic-related supply chain clogs have re-ignited intense examination around the benefits and challenges of embracing reusable versus disposable items in the healthcare setting. In many cases, the choice between the two really comes down to the application.
Some manufacturers have taken a middle path and developed equipment that features both reusable and disposable components. Others offer the same product type in both reusable and disposable versions so customers can choose what works best for them.
Let’s look at some different applications of reusable, disposable and hybrid products in the delivery of patient care, the rationale for taking various approaches and considerations for their safe and effective use.
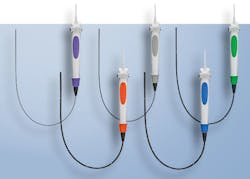
The shift to single-use scopes
In June 2021, the U.S. Food and Drug Administration (FDA) issued new recommendations for healthcare providers on reprocessing bronchoscopes, stating:
“Consider using a single-use bronchoscope in situations where there is increased risk of spreading infection (for example, multidrug resistant microorganisms, immunocompromised patients, or patients with prion disease) or when there is no support for immediate reprocessing of the bronchoscope.”1
Olympus launched its first single-use endoscope in 2021 with a line of premium single-use bronchoscopes, and the company is working hard to bring single-use products to the market where they make the most sense, explains Kenneth Daignault, VP, Single-use Strategy and Development, Olympus.
“Our leadership in endoscopy allows us the ability to develop a portfolio of endoscopes with the goal of providing the right scope, for the right patient, in the right situation,” he says.
“Customers and potential customers have given Olympus a view into the most important attributes that an endoscope should have, which include reliability, maneuverability, ergonomics, workflow features and more,” Daignault added. “Olympus has and will continue to align our offerings to these critical needs and best-in-class attributes to complement our reusable endoscope portfolio with solutions that can fit the need of every specific case. This is leading us to introduce more breadth and balanced portfolio offerings such as single-use endoscopes, which gives our customers access to the best tools for each procedure, site of care and individual patient needs.”
Disposable valve improves endoscope cleaning efficacy
The current multi-society best practice guidelines for gastrointestinal (GI) endoscope reprocessing steps recommend standard manual cleaning followed by high-level disinfection (HLD) and note how “pre-cleaning should commence in the procedure room per protocol, which is typically done by the staff already in the room.”2
An important step in the “pre-cleaning” process, or as the updated version of ANSI/AAMI ST91 now calls it, “pre-treatment,” is for staff in the procedural area to flush the endoscope’s air and water channels. There are two types of air/water cleaning adapters available to perform this flushing step - reusable and disposable. The choice comes down to what is specified in the endoscope manufacturer’s instructions for use (IFU).
The authors of a June 2021 Infection Prevention in Practice (IPIP) article state, “re-usable valves (air/water and suction) used in endoscopes are multi-component, structurally complex devices; as such, cleaning and disinfection are extremely difficult.”3
The Association for the Advancement of Medical Instrumentation (AAMI) and the American National Standards Institute (ANSI) have recommended using disposable adapters for this reason, as specified in ANSI/AAMI ST91:
“Processing of certain reusable endoscope components such as air/water and suction valves … require(s) the same level of inspection, cleaning and high-level disinfection or sterilization as the endoscopes themselves. Providers should therefore “consider the use of single-use, disposable valves.”4
The Society of Gastroenterology Nurses and Associates (SGNA) points to literature that suggests “reusable buttons and valves be reprocessed and stored together with the endoscope as a unique set for tracking purposes.”5
“The Ruhof adapter also eliminates the time-consuming chore of keeping adapters and endoscopes together throughout reprocessing and storing,” Costelloe commented. “By eliminating the need to clean and track reusable adapters, Ruhof makes it easier for cleaning staff to follow reprocessing protocols and gives them more time to focus on each step.”
Ruhof’s adapter is specifically designed for use with Olympus GI endoscopes (excluding Olympus echo-endoscopes that utilize a balloon channel).
Reusable air-purifying respirator reduces PPE waste
As we experience another COVID-19 pandemic winter, and the emergence of the highly contagious Omicron coronavirus variant, clinicians, patients and the general public continue donning personal protective equipment (PPE), most notably face masks, in an attempt to stem virus spread.
The environmental impact of healthcare workers wearing disposable masks during the nearly two years of the pandemic is substantial. A study conducted by researchers from Massachusetts General Hospital, Brigham and Women’s Hospital, the Massachusetts Institute of Technology (MIT) and Columbia University, modeled the impact of various healthcare worker mask usage patterns before and during the pandemic.
“According to their analysis, if every healthcare worker in the United States used a new N95 mask for each patient they encountered during the first six months of the pandemic, the total number of masks required would be about 7.4 billion, at a cost of $6.4 billion. This would lead to 84 million kilograms of waste (the equivalent of 252 Boeing 747 airplanes).”6
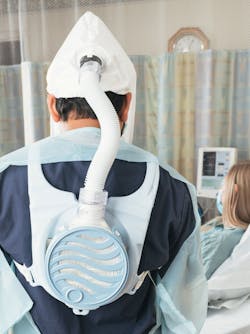
While traditional PAPRs are waist-mounted, the SALUS-HC features a shoulder-mounted design that enables healthcare professionals to experience a full range of motion. It also features sound-dampening motor technology, single button operation and a carriage release hook, which allows the carriage to be removed easily from the wearer’s side and away from their breathing zone.
The Bullard hood is constructed of DuPont Tychem 2000 – smooth glossy and easier and more effective to clean, and therefore reusable. To clean, thoroughly rinse the loose-fitting hood with clean, fresh water and allow to air-dry.
In addition to the waste reduction achieved by using reusable PAPRs versus disposable masks in a healthcare setting, Bullard also calls out the cost savings opportunity. According to the company’s online “Cost in Use” calculator, a healthcare facility with 20 medical professionals requiring respiratory protection could save $109,200 annually by switching from disposable N-95 masks to the SALUS-HC PAPR.7
Two models of patient transfer system for differing needs
The balance between preventing infection and reducing waste is a typical challenge faced by hospitals when evaluating disposable versus reusable products. In some cases, it makes sense for a facility to have two versions of the same product for differing patient needs.
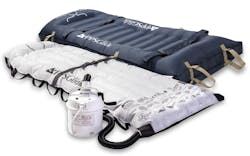
That’s the case with AliMed’s new PPS Glide Air-Assisted Lateral Transfer System, which is offered in both a reusable and disposable option for use anywhere in a facility. The transfer device uses circulating air to move patients with less effort, significantly reducing the amount of pull force required for safer patient transfers.
“This allows for greater operational efficiency,” said Christian Baker, Sr. Product Manager at AliMed. “Hospitals can stock both models and use the appropriate one depending on individual patient needs, such as length of stay or when specific protocols are assigned to different areas of the hospital.”
The PPS Glide Single Patient Use is completely disposable and best for areas where faster cleanup and cross-contamination are a greater concern, such as in the operating room (OR) or emergency department (ED). The PPS Glide Reusable model is best for use on patient floors during longer-term stays where devices are less likely to be soiled and can be easily machine-washed between patients, reducing facility waste. Both options can remain with the patient for the duration of their stay for multiple transfers or as a repositioning aid for boosting, turning or proning.
Reusable PAP system with disposable components reduces cross-contamination risk
Because their bodies, specifically the lungs, are not fully developed, premature infants are at significant risk for respiratory issues, including apnea of prematurity, bronchopulmonary dysplasia (BPD) and respiratory distress syndrome (RDS). In the U.S., there are approximately 18,000 hospitalizations each year due to RDS at a cost of approximately $2.3 billion.8
While equipment for oxygen therapy in the neonatal intensive care unit (NICU) saves the lives of countless preemies, oxygen delivery via invasive mechanical ventilation (IMV) increases the risk for complications, including BPD. Studies have shown that Bubble Continuous Positive Airway Pressure (CPAP) technology, which facilitates oxygen delivery in a non-invasive manner via a mask and nasal prongs, reduces the need for IMV and the risk of BPD or death in preterm infants with RDS.9
Because premature infants are at such high risk for respiratory complications, it is important for neonatal intensive care unit (NICU) teams to do everything possible to reduce the risk for infection. A Bubble CPAP system that features single-use patient components is another way to safeguard these tiny, fragile patients by eliminating the risk for cross-contamination.
The Seattle Children’s Research Institute developed the Seattle Positive Airway Pressure (PAP) plus system, which leverages Bubble CPAP technology and disposable components, including masks and prongs. Produced and marketed by Dräger, the Seattle PAP plus system received FDA clearance in August 2019. Its development was funded by the Bill and Melinda Gates Foundation.
Conclusion
Health systems and hospitals struggle to provide high quality and safe patient care in a cost-effective manner. Medical supplies and equipment represent a large portion of their budgets and play a central role in patient outcomes. Manufacturers recognize this challenge and continue to expand their product portfolios to offer more choices. By assessing infection risk, costs, functionality and patient impact, healthcare teams can select the right product options to meet their goals.
References
1. Flexible Bronchoscopes and Updated Recommendations for Reprocessing Safety Communication, FDA, June 25, 2021, https://www.fda.gov/medical-devices/safety-communications/flexible-bronchoscopes-and-updated-recommendations-reprocessing-fda-safety-communication
2. Management of endoscopes, endoscope reprocessing, and storage areas during the COVID-19 Pandemic, American Society of Colon and Rectal Surgeons (ASCRS), accessed December 28, 2021, https://fascrs.org/getattachment/5ef92409-cade-4928-96cf-91ca53ebad93/GI-Society-management-of-endoscope-fleet.pdf?lang=en-US
3. Infection prevention in endoscopy practice: comparative evaluation of re-usable vs single-use endoscopic valves, Infection Prevention in Practice (IPIP), June 2021, https://www.sciencedirect.com/science/article/pii/S2590088921000111
4. ANSI/AAMI ST91: 2015 Flexible and semi-rigid endoscope processing in health care facilities
5. Standards of Infection Prevention in Reprocessing Flexible Gastrointestinal Endoscopes Webinar FAQ, SGNA, https://www.sgna.org/Portals/0/FAQ_Standards%20of%20Infection%20Prevention%20in%20Reprocessing%20Flexible%20Gastrointestinal%20Endoscopes.pdf#:~:text=Per%20the%20SGNA%20Standards%20of%20Infection%20Prevention%20in,facility%20must%20determine%20their%20individual%20practices%20and%20policies
6. The environmental toll of disposable masks, July 20, 2021, MIT News Office, https://news.mit.edu/2021/covid-masks-environment-0720
7. PAPR vs. N95 Cost in Use calculator, Bullard, https://www.bullard.com/papr-vs-n95
8. Breathing in America, American Thoracic Society, January 2010
9. Behnke J, Lemyre B, Czernik C, Zimmer KP, Ehrhardt H, Waitz M. Non-Invasive Ventilation in Neonatology. Dtsch Arztebl Int. 2019;116(11):177-183. doi:10.3238/arztebl.2019.0177
About the Author
Kara Nadeau
Senior Contributing Editor
Kara Nadeau is Sterile Processing Editor for Healthcare Purchasing News.