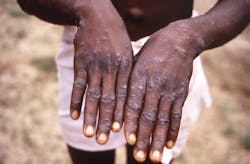
Monkeypox outbreak reported in nine states
There is a current identification of monkeypox clusters in several countries that do not have endemic disease and involving patients with no direct travel history to an area with endemic monkeypox suggests person-to-person community spread, according to latest Morbidity and Mortality Weekly Report (MMWR) from the Centers for Disease Control and Prevention (CDC).
Close contact with infected persons or fomites (e.g., shared linens) is the most significant risk factor for Monkeypox virus infection in human monkeypox outbreak.
Monkeypox virus is spread through close, often sustained skin-to-skin contact, but the initial appearance or occurrence of lesions in the anogenital area observed in the current outbreak differs from the typical appearance or occurance beginning on the face, oral mucosa, and hands and feet, then spreading to other parts of the body in a centrifugal distribution.
The high proportion of initial cases diagnosed in this outbreak in persons who identify as gay, bisexual, or other MSM, might simply reflect an early introduction of monkeypox into interconnected social networks; this finding might also reflect ascertainment bias because of strong, established relationships between some MSM and clinical providers with robust STI services and broad knowledge of infectious diseases, including uncommon conditions. However, infections are often not confined to certain geographies or population groups; because close physical contact with infected persons can spread monkeypox, any person, irrespective of gender or sexual orientation, can acquire and spread monkeypox.
The following measures can be taken by the public to prevent infection with monkeypox:
1) isolate ill persons from uninfected persons;
2) practice good hand hygiene and use appropriate personal protective equipment to protect household members if ill or caring for ill persons at home (e.g., a surgical mask, long sleeves and pants, and disposable gloves); 3) use an Environmental Protection Agency–registered disinfectant with an emerging viral pathogens claim that is found on EPA’s List Q for disinfection of surfaces.
Patients should also avoid contact with pets and other animals while infectious, because some mammals might be susceptible to monkeypox. Persons with symptoms of monkeypox, including unexplained lesions, should contact their health care provider for an evaluation and should avoid close contact with others, including intimate or sexual contact, until they are evaluated or receive testing.
CDC urges healthcare providers in the United States to be alert for patients who have rash illnesses consistent with monkeypox, regardless of a patient’s gender or sexual orientation or a history of international travel or specific risk factors for monkeypox. Clinicians should contact their local or state health department if they suspect a case of monkeypox.
There are 110 LRN laboratories available and equipped for rapid diagnostic testing of emerging pathogens across the United States; currently 68 test for orthopoxviruses. The prolonged interval from rash onset to positive test result was reflective of delays in clinical suspicion of an unfamiliar illness; all patients had results within 0–2 days after specimens were collected. During this outbreak, a positive test result for an Orthopoxvirus at an LRN laboratory is presumed to be monkeypox and is actionable for antiorthopoxviral treatment, and by public health authorities to initiate isolation, contact tracing, monitoring, investigation, and PEP of exposed contacts. PEP with smallpox vaccines remains available from the strategic national stockpile for eligible exposed persons.
As the source and spread of this outbreak are being investigated, it is crucial to assess all possible modes of transmission and identify risk groups, as well as institute appropriate public health preventive measures. CDC is providing guidance on case definitions, identification of contacts, clinical management, and infection control and prevention within health care facilities and the home, creating resources for disseminating information on monkeypox, and supporting laboratory testing infrastructure domestically and globally.
Monkeypox, a zoonotic disease for which the animal reservoir is unknown, is endemic in several Central and West African countries. There are two clades of Monkeypox virus, West African, and Congo Basin, the latter causing more severe illness. The last United States monkeypox outbreak was secondary to imported small mammals from Ghana in 2003; however, since monkeypox reemerged in Nigeria in 2017, isolated cases outside Africa have been reported either among persons with recent travel to Nigeria or among secondary contacts of persons with travel-associated cases.
Patients with monkeypox typically experience a febrile prodrome 5–13 days after exposure (range = 4–17 days), which often includes lymphadenopathy, malaise, headache, and muscle aches; this prodrome might depend on the nature of exposure. The prodrome is followed 1–4 days later by the onset of a characteristic deep-seated, vesicular or pustular skin rash with a centrifugal distribution (Figure); the lesions are well circumscribed and often umbilicate or become confluent, progressing over time to scabs. The rash can be disseminated. Some recent cases have begun atypically, with lesions in the genital and perianal region and without subjective fever or other prodromal symptoms. For this reason, cases might be confused with more commonly seen infections such as varicella zoster or sexually transmitted infections (STIs) (e.g., genital herpes or syphilis). The case-fatality ratio for the West African clade of monkeypox is reported to be 1% and might be higher in immunocompromised persons.
A person is considered infectious from the onset of illness until all lesions have crusted over, those crusts have separated, and a fresh layer of healthy skin has formed under the crust. Human-to-human transmission occurs by direct contact with infected body fluids or lesions, via infectious fomites, or through respiratory secretions, that typically require prolonged interaction. Historically, documented reports of human-to-human transmission have been among household contacts and shared housing inhabitants (e.g., in prisons), and healthcare providers who have had close, sustained contact with a patient or patient fomites (e.g., bedding).
Investigation and Results
United Kingdom. The United Kingdom Health Security Agency (UKHSA) announced a confirmed monkeypox case on May 7, 2022, in a traveler returning from Nigeria. On May 14 and 16, UKHSA announced a second unrelated cluster of two cases and a third clustered group of four cases identified at sexual health clinics; the four-case cluster involved persons who identify as gay, bisexual, or MSM.
Massachusetts. On May 4, a Massachusetts resident developed an anogenital rash 3 days after returning from international travel. This rash progressed to vesicles and pustules and spread to the face and trunk; the patient sought medical care four times at outpatient clinics during May 4–12, during which time common causes were ruled out. The patient was hospitalized on May 12 for management of refractory perianal pain from the rash. Prompted by UKHSA’s announcement regarding the recent monkeypox cases, clinicians notified the MDPH and CDC for testing. On May 17, the patient received a diagnosis of confirmed Orthopoxvirus by the Massachusetts LRN laboratory, and CDC confirmed Monkeypox virus West African clade the following day. The local hospital infection prevention team, MDPH, and CDC responded to identify contacts and determine exposure risk, facilitate PEP with one of two orthopoxvirus vaccines (ACAM2000†† or JYNNEOS§§), and provide guidance on infection prevention and control. Outbreak case definitions were created (Table 1). Exposure risk assessment tools used during investigation of a 2021 travel-associated monkeypox case in Texas were adapted to monitor cases and determine criteria for recommending PEP.
New York. On May 4, a traveler returning to New York City (NYC) was evaluated for an oral lesion, and a new painful, perianal rash; the patient was tested and treated for a presumed common STI and sent home. The rash spread, progressing to pustules, and the patient was seen again and treated for a different STI; all testing results were ultimately negative. On May 19, after the announcement of the monkeypox case in Massachusetts, a clinician caring for the NYC patient notified the NYC Department of Health and Mental Hygiene (NYC DOHMH) about the possibility of monkeypox. The patient received a positive orthopoxvirus test result at the NYC LRN laboratory and continued to isolate at home. NYC DOHMH began identifying contacts, determining exposure risk, and facilitating PEP for at-risk contacts.
Other U.S. states. Over the next 5 days from the identification of the NYC case, multiple states received notifications from clinicians about suspected monkeypox cases; on May 23, an incident command structure was created within CDC’s National Center for Emerging and Zoonotic Infectious Diseases to respond to this outbreak. As of May 31, nine states (California, Colorado, Florida, Georgia, Massachusetts, New York, Utah, Virginia, and Washington) have reported 17 patients with confirmed orthopoxvirus infections, which until proven otherwise, are considered to be Monkeypox virus during this outbreak response.
Fourteen patients of the 17 patients reported international travel involving 11 different countries during the 21 days preceding symptom onset, and 16 of the 17 patients identified as MSM. All patients were adults (average age = 40 years; range = 28–61 years), and all had rash onset dates during May 1–27; three patients were immunocompromised. Diagnosis of an orthopoxvirus infection occurred an average of 11 days after rash onset (range = 0–21 days. In addition to skin rash, patients commonly reported chills (12) fatigue or malaise (11), and lymphadenopathy (nine); fever was reported in seven patients (Table 2). Twelve patients reported prodromal symptoms before rash onset such as fatigue, fever, or headache. Among eight patients, the rash started in the genital or perianal area. All but one patient developed a disseminated rash, occurring on the arms, trunk, legs, and face.
Public Health Response
Currently, all patients are clinically well and being monitored by health authorities to determine the end of isolation (i.e., after all lesion scabs have fallen off, and new, healed skin has formed). One patient was treated with tecovirimat, an antiviral agent from the strategic national stockpile with antiorthopoxvirus activity, licensed for smallpox but available from CDC under an expanded access Investigational New Drug protocol.
CDC also facilitated the availability of vaccine PEP to contacts with high-risk exposures (e.g., unprotected contact with the skin or mucous membranes, lesion, or body fluids of a patient) or certain intermediate risk exposures (e.g., being within ≤6 ft of an unmasked patient for ≥3 hours without wearing, at a minimum, a surgical mask). PEP is not recommended for low or uncertain risk (e.g., health care providers entering a patient’s room without eye protection). Eligible intermediate- and high-risk contacts are offered PEP with ACAM2000 or JYNNEOS vaccines.
Contact investigation is ongoing; among the 13 patients who have identified contacts, there are 56 high- 117 intermediate-, and 235 low- or uncertain-risk contacts. Contacts are recommended to be monitored for signs and symptoms consistent with monkeypox (e.g., fever, chills, lymphadenopathy, and rash) for 21 days following last exposure.
Genome sequencing results from virus recovered from the patient in Massachusetts display similarities to other published genomes in this outbreak from Europe (Nextstrain/monkeypox) and are related to the 2017–2018 monkeypox outbreak in Nigeria. As of June 2, preliminary data indicates approximately 800 monkeypox cases have been reported in this outbreak from 28 countries, including the United States.
The current identification of monkeypox clusters in several countries that do not have endemic disease and involving patients with no direct travel history to an area with endemic monkeypox suggests person-to-person community spread. Close contact with infected persons or fomites (e.g., shared linens) is the most significant risk factor for Monkeypox virus infection in human monkeypox outbreaks.