The desire for clinicians to see clearly inside the human body has driven the proliferation and advancement of instruments and devices for this purpose, including extremely high-resolution medical grade displays. It is big business. The global medical displays market is expected to reach $2.45B by 2025, driven by the growth in diagnostic imaging centers and hybrid operating rooms (OR).1
Manufacturers of medical displays and monitors continue to stretch the bounds of what can be made visible to the human eye to improve procedural precision and patient outcomes. At the same time, they are developing larger screens that can take the place of multiple, smaller monitors to improve procedural area workflows by reducing complexity and clutter.
Clinical training is another key consideration when it comes to medical display and monitor selection. With the shift to remote learning that has taken place during the COVID-19 pandemic, high-resolution displays can bring medical students into a surgery from anywhere when paired with supporting technologies.
And with safety always critical to successful patient procedures, medical display and monitor manufacturers are designing new products with infection control/prevention in mind.
The visualization evolution
According to Sony’s Marketing Manager, Anne Bondulich, many of the trends in medical grade displays and monitors are tied to the pursuit of better visualization during surgery and post-procedure. She points to 4K, 3D and High Dynamic Range (HDR) as some of the latest technology innovations in this area, stating:
“4K offers four times the resolution of standard HD and virtually no pixelation. This is helpful for medical professionals because the enhanced level of detail, clarity and in turn, more information, provides a better view of a procedure.”
Bondulich says Sony’s 4K medical displays can also provide upscaling of HD video content. Additionally, medical teams using Sony’s 4K display technologies have the capability to see a “quad-split” view of four full HD signals (1920x1080) on one display, helping them view four full HD sources at one time.
“3D offers depth of field that helps to increase immersion,” Bondulich explains. “In addition, HDR delivers better contrast with more realistic peaks of brightness, shadow detail and deeper blacks, which are important when identifying and working with blood, blood vessels, nerves and other critical structures. All of these technologies help provide more engaging and realistic training and education.”
“In addition, having access to the most advanced tools and technologies helps surgeons see more, be more efficient and helps promote accuracy,” she added. “Having enhanced access and visualization can result in the potential for improved patient outcomes.”
Larger displays maximize visibility, reduce OR footprint
The continued growth in the types and number of minimally invasive surgical procedures performed on patients has driven the need for improved surgical imaging. Between 2016 and 2020, minimally invasive surgery demand grew 4% and this demand is expected to continue in the years ahead driven by the benefits over open surgeries (e.g., less trauma, reduced complication risk, faster recovery times, etc.).2
Hilary Dilsaver, Product Manager, 4K Imaging, Surgical Endoscopy, Olympus America, has seen an increase in Big Screen end-to-end 4K monitor (often 55”) usage for laparoscopy in the OR, which enables surgical teams see four times the resolution of HD imaging for help in visualizing details in difficult procedures, stating:
“The larger, natural color gamut helps in delineation of tissue boundaries, visualization of blood vessels and lesions. The larger monitors also may provide the OR staff a more immersive experience. All eyes can be on the Big Screen monitor regardless of an OR team member’s position in the room.”
Dilsaver explains how 4K systems deliver four times the pixels, higher resolution, better light and a wider color gamut than High-Definition (HD) displays for a Big Screen Surgery experience in the OR.
While the vast array of equipment for surgeries is growing, in most cases the square footage of ORs is not. Surgical staff members struggle to care for the patient surrounded by machines, monitors, cords and other related items. Dilsaver says Big Screen monitors help OR teams overcome this challenge:
“By using a larger screen, hospitals are replacing the clutter of smaller monitors in the room as well as decreasing the footprint in the OR.”
Displays designed for infection prevention
Hospital-acquired infections (HAI), including surgical site infections (SSI), endanger patient lives and add billions of dollars in healthcare costs each year. Research has shown that in “open clean surgery, risk of SSI is strongly correlated with the amount of airborne bacteria being present in the operating room and the surgical field.”3
Medical display and monitor manufacturers are designing new technologies with features that reduce the risk for contamination of the sterile field from airborne microbes, as Matt Bottino, Director of Marketing, Surgical Solutions, STERIS, describes:
“STERIS Surgical Displays are designed for use within the sterile field or any clean environment. Unlike other displays, STERIS Surgical Grade displays are sealed, ventless and fanless so they don’t collect or blow contaminants into the environment. They can also be disinfected quickly without worry that the cleaning agent will get inside the display.”
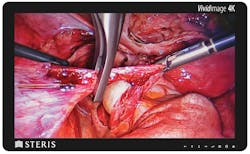
The STERIS Vividimage 4K Surgical Display delivers accurate, true-to-life surgical video in the OR. With four times the detail of HD video, surgeons experience greater visual depth and a wider range of colors allowing them to visualize fine details in tissues and structures.
With a sealed, fanless and durable design, the Vividimage 4K Surgical Display is silent, easy to clean and highly resistant to impact in the surgical suite. This surgical monitor is also designed for staff comfort and safety, offering a black bezel to reduce eye strain and a white back for visibility in a dimly lit OR.
Streamlined education and training
The consolidation of monitors and displays can help with staff education as clinicians can train on fewer pieces of equipment, explains Katie Szyman, Corporate Vice President, Critical Care, Edwards Lifesciences.
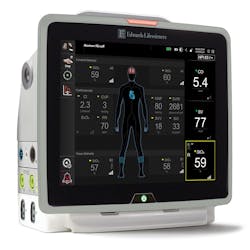
“Our latest monitor, HemoSphere advanced monitor, is the only monitoring platform on the market that offers compatibility with noninvasive finger cuffs, sensors and catheters,” said Szyman. “We believe the all-in-one solution is an important advancement, and one that could help clinicians and hospitals on many fronts.” This full-range compatibility enables individualized patient management across a diversity of patient profiles and across care settings and can help simplify the variety of different monitors a hospital needs to purchase.
The HemoSphere monitor also supports more efficient and effective clinician workflows through its software. Szyman says it is the only monitor on the market that is compatible with software that predicts the likelihood of intraoperative hypotension, Acumen Hypotension Prediction Index software.
“Intraoperative hypotension is common and associated with risks such as acute kidney injury and myocardial injury,” Szyman explained. “Using the HemoSphere monitor along with a noninvasive cuff or an arterial line sensor, clinicians can access this software and get an alert if a patient is trending towards a hypotensive event. The clinician can also get insights on the root cause and inform a potential course of action.”
In support of remote learning
The COVID-19 pandemic has presented significant challenges to medical education and training. An international team of clinicians from the U.S., UK and Europe published a review article in 2020 on the subject, stating:
“The shutdown of academic institutions, alongside the novel challenge imposed on healthcare systems worldwide, have taken an immense toll on the quantity and quality of medical education. Medical students and junior doctors are thus faced with the oxymoron of not receiving adequate education but being required to potentially serve in the frontlines. How can medical students and residents bridge the gaps created in their training, and ensure that they will continue to receive the knowledge and skills required to progress as competent and safe clinicians?”4
The Association of American Medical Colleges (AACM) describes how medical educators shifted their approach as “Webcams captured hospital rounds, 3D images replaced cadavers, and Zoom classes had students raising virtual hands to debate diagnoses.”5
Bondulich comments on the trend toward virtual learning for medical students and describes how medical displays have supported this new approach:
“The pandemic forever altered how medical students are trained on surgical procedures. The benefits of having fewer people in an operating room to minimize the spread of disease rapidly came into focus. Having tools like a large, state-of-the-art display helps everyone inside or outside of the OR to have the same view as the primary surgeon – whether it’s members of the care team or students.”
“What’s also beneficial is that Sony’s displays can easily be integrated with remote monitoring solutions including PTZ cameras and the Sony NUCLeUS video-over-IP system to enable a live surgery to be viewed remotely, from virtually any location in the hospital, including conference rooms or lecture halls,” Bondulich added.
The future of surgical imaging and visualization
Innovation never stops, especially in the medical field. Manufacturers are constantly working to develop new technologies that will enhance visualization during surgery and the surgeon experience. Here are two new products recently announced by manufacturers that leverage digital capabilities, such as artificial intelligence (AI), machine learning (ML), extended reality (XR), robotics and computer vision (CV).
Cloud-enabled, 3D modeling:
“The potential of INTRAVISION XR technology extends not only to patient education and surgical planning but will also push the barriers of actual real-time surgical guidance,” said DICOM Director’s CEO David B. Pearlstone, MD, MBA. “With object placement and registration we will have the capability to create ‘virtual x-ray vision’ in the OR.”
AI-enhanced laser visualization;
Certes by Perfusio allows surgeons to see the actual dynamic physiology of blood flow distribution in tissue, using a proprietary combination of multi-spectral imaging and AI-enhanced laser speckle contrast analytics with immediate real-time display of quantified tissue perfusion.
Perfusio’s Certes resolves this dilemma by providing new knowledge utilizing multiple wavelength illumination and AI-enhanced analytics based on laser speckle contrast imaging to display in immediate real-time multi-spectral physiologic visualization (MSPV) of the actual dynamic physiology of blood flow distribution in tissues.
MSPV does not require patient contact, dyes or ionizing radiation. It is safe for patients and providers, even when used multiple times during an operative procedure to enhance surgeon judgment and decision-making. MSPV immediately identifies which tissues have normal perfusion, and which tissues do not, giving the surgeon the opportunity to identify and correct perfusion problems at the time of the initial procedure.
“Our purpose at Perfusio is to implement solutions that improve patient lives and to create significant overall savings to the healthcare system by developing a new standard of care with AI-enhanced visualization and new knowledge,” Tucker added.
Google Maps for the body6
Proprio, based in Seattle, is developing an advanced surgical imaging platform that leverages CV and ML to improve surgical navigation. By synthesizing views from multiple sensors, the platform enables users to navigate surgical environments in 3D.
References
1. Global Medical Display Market, Size, Outlook, Trends and Forecast (2021-2026), Envision Intelligence, June 30, 2021, https://www.envisioninteligence.com/industry-report/global-medical-display-market/
2. Minimally Invasive Surgery Market to Surge 1.6x, back by Preference for Robotic Surgery: Fact.MR Study, Fact.MR, September 27, 2021, https://www.factmr.com/media-release/2368/global-minimally-invasive-surgery-trends
3. Persson M. Airborne contamination and surgical site infection: Could a thirty-year-old idea help solve the problem? Med Hypotheses. 2019 Nov;132:109351. doi: 10.1016/j.mehy.2019.109351. Epub 2019 Jul 31. PMID: 31421424.
4. Medical and Surgical Education Challenges and Innovations in the COVID-19 Era: A Systematic Review, In Vivo, May/June 2020, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8378024/
5. No classrooms, no clinics: Medical education during a pandemic, AAMC, April 15, 2020, https://www.aamc.org/news-insights/no-classrooms-no-clinics-medical-education-during-pandemic
6. “Google Maps for the human body” – AI’s rise in surgical tech, June 9, 2021, https://www.propriovision.com/news/google-maps-for-the-human-body-ais-rise-in-surgical-tech
About the Author
Kara Nadeau
Senior Contributing Editor
Kara Nadeau is Sterile Processing Editor for Healthcare Purchasing News.