Midwestern IDN supply chain team creates, regenerates value for clinicians, patients
For many healthcare organizations and professionals, value analysis merely represents a form or function, a procedure or process. But that’s not enough for one Midwest integrated delivery network treating patients in the heartland.
For The University of Kansas Health System, value analysis represents a key component of a much-larger over-arching philosophy and way of thinking that they purposefully root within well-defined clinical integration to drive cost-effective operations.
Thirteen professionals comprise the “Clinical Supply Optimization” (CSO) team at the Kansas City, KS-based IDN that services the entire organization. The team spans seven in CSO’s Value Analysis group—four Value Analysis Analysts, two Implementation Analysts and one System Manager of Value Analysis; and four in the Utilization Management group—two Utilization Management Analysts, one Procedural Supply Optimization Analyst and one System Manager of Utilization Management. The two groups report to the System Director of Clinical Supply Optimization and the System Senior Director of Supply Chain Management and Administration and up to the Vice President of Supply Chain.
University of Kansas’ CSO team may be small, but they’re effective and efficient in the value they bring to the organization in bridging—if not filling—any gaps between administrative, clinical and financial operations, which earned them the 2023 Value Analysis Performance Excellence in Supply Chain Award by Healthcare Purchasing News.
What follows is an edited version of their nomination profile that traces the development of the CSO team just prior to and during the pandemic to now.
Teamwork’s inherent value
If you give a Value Analysis team the right people, processes, and systems they might just create extraordinary value for their organization. If you give a Value Analysis team hundreds of clinical end users to work alongside, they just might create something extraordinary for patient care.
What if you gave a Value Analysis team both? That is what happened when The University of Kansas Health System ventured down a new pathway to transform their Value Analysis team in 2020. The journey started with asking three main questions:
1. How can the health system achieve a successful clinically integrated supply chain?
2. How can Supply Chain Value Analysis bring the most value to the organization?
3. Are the right people at the table?
The University of Kansas Health System takes pride in placing its patients and its people as its top priority. With people and patients at the top of the list, they saw a need to fully understand what it meant to have a health system that generates and maintains true clinical alignment with the supply chain. The next three years highlight how these focus areas were foundational in growing the Value Analysis department into what is now called Clinical Supply Optimization (CSO).
2020-2021 – Discovery during a pandemic
Faced with the greatest of needs in the throes of a global pandemic that the world had not faced since the early 1900s, there was much to do, and it all had to be done with urgency. The University of Kansas Health System's Supply Chain department had already been planning to expand the Value Analysis team and knew that pausing that work would not benefit the organization. The need to be fully clinically integrated as a supply chain was greater now than ever before.
Getting the right people
Throughout the fact-finding process, they determined that a key piece to drive a successful clinically integrated supply chain was missing and that the focus had to go beyond financial outcomes by including clinical and operational perspectives. To do this, they needed to recruit executive leadership support to form an additional arm to Value Analysis called Utilization Management (UM). UM extends the scope of work beyond the projected value of a new product into the organization. This team takes supply chain initiatives and reviews their clinical, operational, and economic outcomes for 12 months. UM stays in constant communication with those end users to drive conversations to achieve the best value for patients, staff, and the organization as a whole.
As VA and UM combined formed the CSO team, the next step was to spread awareness throughout the health system and to share how the team supported its clinical end-users. This occurred through inviting key clinical stakeholders to participate in discussions and in making strategic decisions on which products are used organization wide through clinical evidence gathering, best practice sharing, market trends and insights and by leveraging the organization’s group purchasing organization (GPO) contracts and committed-volume contracts (Vizient and Captis, respectively). These conversations took place as part of committee involvement.
Today, CSO leads or participates in more 40 clinical committees and facilitates a governance meeting that supports the strategic mission and vision for supply chain to provide the highest quality products to patients and staff at the best value for the organization. These committees are focused on quality and safety, patient outcomes, advanced technology to support new patient populations, and the economic and operational impacts these decisions could make. It is the collaboration between each clinician and CSO team member that creates the success of this program.
2021-2022: Execution and implementation
During the second year, CSO discovered a gap within the team—an opportunity identified to enhance the speed to value on project initiatives. Therefore, the team held a business case review and determined a need to incorporate an Implementation Team that would drive conversions from time of product and/or purchased service approval to first invoice paid. This team is instrumental in leveraging end-to-end supply chain knowledge that accounts for changes in purchasing, distribution, and inventory management and control. The team’s collaboration with both clinical and ancillary departments across the health system, has accounted for achieving contract compliance and a total of $90,000 in savings on converting patient bathing wipes and moving to vendor scrubs alone.
Additionally, the CSO team began supporting two new bodies of work: Recall Management and Non-conforming Processes, also known as defective products. CSO embodies Supply Chain Quality and Safety, and these processes help staff and patients experience safe, high-quality products. UM put together processes, formalized a policy and rolled out the added support the CSO team would provide for departments across the health system. One of the most recognized non-conforming products the organization endeavored resulted in a supplier changing their manufacturing process due to the negative product feedback submitted to them, resulting in The University of Kansas Hospital receiving an FDA Certificate for Outstanding Contribution in Promoting Patient Safety with Medical Devices in January 2023. This is the power of the non-conforming process. To date, the UM team has managed more than 325 non-conforming products resulting in more than $100,000 in credits back from suppliers.
Also in 2022, The University of Kansas Health System aligned with Medline as its strategic distribution partner. Medline provides supply distribution for acute and non-acute care encompassing approximately $60.5 million in spend and also supports the organization’s home medical equipment (HME) business that provides hospital-to-home healthcare. Quarterly, both the Supply Chain department and Medline conduct business reviews in which the parties collaborate to discuss opportunities that are then brought before the committees for review and approval. This has helped the health system realize a 97% price accuracy and achieve $425,000 in savings with product conversions.
When CSO reviews any product category, the team discusses opportunities with Medline to determine whether it meets the clinical, operational, and economic needs of the organization. In 2021, The University of Kansas Health System transitioned its medical device reprocessing program to Medline. To date, savings have accounted to more than $1.8 million by utilizing reprocessed products. The health system has also diverted 17,222 pounds in medical waste out of local landfills. Additionally, Medline has supported the organization in reducing production variation and contributes to product formularies. For example, during the transition to Medline non-acute the team was able to reduce the product formulary by 50%. This strategic partnership with Medline has resulted in successful outcomes due to clinical integration and the dedicated Medline support team.
With the creation of the Implementation Team, the execution of new workflows and the strategic partnership establishment with Medline, the CSO team was able to provide $9 million in savings across the health system since inception in mid-2020.
The CSO team’s efforts earned them several national awards and recognitions in 2022:
- Vizient Connections Summit—“5 Rights” of Clinical Supply Management
- GHXcellence Awards—Elevating the Clinically Integrated Supply Chain Award
- Medline Sustainability and Supply Excellence Gold Award—Medline ReNewal reprocessing program
2022 – 2023: Continuous improvement
By the third year, the CSO team had a devoted, talented group in place with consistent and effective processes in working order. The next step was to grow the team for future sustainability by creating and establishing a Procedural Supply Optimization (PSO) team. PSO’s main responsibility is to partner with clinicians and physicians in surgical and procedural settings to prevent waste and optimize supply utilization that brings the best clinical, operational, and economical outcomes for the health system. The team has clinical experience to support intricate conversations with clinical end-users, yet robust supply chain knowledge to drive conversations that could lead to a product utilization change by a physician or clinician to achieve contract compliance and reduce cost per case.
CSO is proud but never satisfied and is always looking to set the bar higher through evaluating advanced technologies with clinical, financial, and strategic partners following their mission statement: To utilize evidence-based analytics to optimize clinical, operational, and economical stewardship that drive decisions across the health system. The team connects with internal and external customers to enhance processes and build upon the workflows currently in place today to ensure long-term sustainability. Finally, the CSO team applies supportive technologies and systems to improve processes and communication with its customers.
The CSO team’s efforts continue to earn them national awards and recognitions this year, too:
- The University of Kansas Health System and the University of Kansas Medical Center Safety Symposium Presentation—How Supplies Impact Patient Safety
- Vizient Connections Summit—A Robust Product Reprocessing Program, A Trifecta of Success
Together, the CSO team built a program designed to work in tandem with clinical teams and health system leadership to enhance patient safety, provide financial and operational data that help drive decisions, and incorporate clinical evidence into its workflows. Since inception, the program has helped achieve more than $23.8 million in savings, demonstrating the value of teamwork at its finest.
Sidebar w/chart:
Midwestern CSO team explains mindset, motivation for driving value
The Clinical Supply Optimization (CSO) team at The University of Kansas Health System fuses solid professional working relationships between clinicians and administrators that delivers value to the doctors, nurses and surgeons in the clinical theater as well as the administrators and supply chain professionals in the finance and operations theater. Together, these efforts at sourcing, contracting, acquisition, utilization and disposal constitute the lifecycle of support for high quality patient care within the communities they serve. Angie Bruns, senior director, Supply Chain Management and Administration shares with Healthcare Purchasing News Senior Editor Rick Dana Barlow the background and underpinnings of their success.
HPN: Does a clinically integrated supply chain hinge on the application/inclusion of value analysis? Why?
BRUNS: It does for The University of Kansas Health System. The Value Analysis team was the catalyst for this endeavor, taking time to listen to end users. As an industry, we recognized the challenges value analysis programs faced and began to develop a new program that could support the organization’s needs. The initial focus was on building relationships between clinicians and supply chain by bringing forth clinical evidence data analyses.
The data drives the decisions. However, it is the relationships with those end users that enable the team to share it effectively, timely and with ease. Those connections are essential in establishing the team now known as “Clinical Supply Optimization,” which encompasses additional bodies of work that require supply chain support.
The team's work on recall management and non-conforming products are examples of two programs that enabled the team to collaborate closely with the quality and safety teams, risk management, and educators to support the use of products.
There seems to be many definitions of the term “clinically integrated supply chain.” What’s yours and why does it matter?
The University of Kansas Health System defines a clinically integrated supply chain as an interdisciplinary model which utilizes evidence-based analytics to optimize clinical, operational, and economical stewardship to produce world-class patient care at a fair cost. Everything we do is for the patient. This model places focus on quality, safety, and outcomes, it also brings essential questions and topics of operational and financial components into focus.
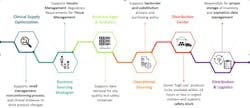
True clinical integration relies on the entire department to achieve outcomes. There are many components within the health system’s supply chain department as shown below. Clinical integration cannot occur without all the functional areas connecting, aligning, and collaborating on one goal: world-class patient care.
The need to establish a clinically integrated supply chain was the main motivation. The Value Analysis team was the driver, but the team does not stand alone. Without support from and collaboration with all the functional areas of supply chain and clinical leaders, becoming clinically integrated would not be possible.
The CSO program is modeled throughout the health system. In January 2021, the organization acquired a new facility with one of the goals through 2024 being to integrate the CSO program into that facility. End-users have joined clinical committees in which they review product requests and discuss contract opportunities to align the facility’s product utilization. Success rides on building relationships, listening to clinicians, and providing evidence-based data outcomes to support patients’ needs.
What value analysis project success story are you most proud of so far and why? How replicable is it?
Most recently, the team partnered with the health system’s quality and safety teams to support CAUTI [catheter-associated urinary tract infections] reduction. One piece was to change patient bathing wipes to a different product which also came with significant savings of just over $49,000. The bigger win was a decrease in patient CAUTIs. This would not have been feasible without the support of clinical end users, supply chain team partners and supplier partners.
The CSO program and its processes are meant to be replicable and scalable, leaving room for continuous process improvements. The CSO team strives to review initiatives beyond the price by evaluating the price of the product and the price of patient outcomes.
In your opinion, what are the toughest administrative challenges for value analysis in the following four areas and how did or might you overcome each:
· Administrative—Executive leadership support.
Leadership sets the strategic vision, holds the teams accountable, and removes barriers. Executive leadership also presents the value of the program with emphasis on patient and staff safety. Without this support, the CSO program would not exist.
· Clinical—Support from clinicians.
Feedback from clinicians is crucial in building a successful, clinically integrated supply chain. There is no clinical integration without clinicians, therefore, involvement from clinical leaders is necessary. Clinical leaders are included in conversations on opportunities for improvement. As committees were formed, clear expectations of the work were established together to review initiatives, execute, and monitor clinical and fiscal outcomes.
· Financial—Having all the right data.
Partnering with other departments enables the teams to view the full project scope. Decisions may need data on evidence, budgetary impact, physician utilization, reimbursement, or offer a strategic perspective. Clinicians are responsible for guiding these decisions and supply chain provides the evidence necessary to support the decisions.
· Operational—Executing a new program requires successful communication.
The health system leveraged a one-on-one meeting structure. It also holds regular leadership meetings, small team huddles, and daily email communication to communicate the new program. Communication included CSO’s purpose, goals, and how everyone in the health system can participate in this journey. There were weeks of time invested in preparing and following up on communication provided throughout the health system.
The CSO program is designed to work within any medical center regardless of size. By leveraging committee structures and daily organizational communication, team members have awareness, have a seat at the table, and participate in decision-making.
What are the top three priorities for CSO’s value analysis (VA) and utilization management (UM) subgroups going into 2024 and why?
1. Program expansion. In 2023, The University of Kansas Health System acquired a new facility in the southwest Kansas City market. The Supply Chain department in actively implementing Clinical Supply Optimization into the new facility. To achieve this, there needs to be program centralization that includes voices from every facility. Moving together as one system to deliver care to every patient that comes through the door.
2. Cost-per-case opportunities. The team uses data to review, discuss and drive down cost-per-case opportunities within the surgical departments. This achieves the lowest cost of care component in a clinically integrated supply chain model.
3. Product variation reduction and contract maximization. The CSO team focuses on opportunities that will reduce variation of products across organization. This will help drive down costs and put more focus on providing the best patient care possible.
The equation VA + UM = CSO represents an interesting development that seems borne from the pandemic. Could or would you have pursued this concept or model regardless of a major crisis or did/do you need such a crisis to ignite this kind of thinking and progress? Why?
As the only Academic Medical Center in Kansas, our vision is to lead the nation in caring, healing, teaching and discovery. For Supply Chain we knew our part of this vision was a clinically integrated supply chain. Our strategic focus began in 2019. The mindset was to view it from a quality and safety and economic perspective. Culturally, the team was seen as wanting to change products to save money, though it is much more than that.
The health system became deeply affected by the pandemic in March 2020, though the clinical integration work had already begun. End-users were faced with having to utilize various products out of necessity due to global supply and raw-material shortages. If anything, the pandemic enhanced the clinical integration work across the Supply Chain department, not just Value Analysis by bringing clinicians and supply chain together to tackle supply challenges.