Placing a dollar sign on Infection Prevention
We are living in the IP age.
In these times of COVID-19 and the ongoing battle against Healthcare Associated Infections (HAI), Infection Prevention could not be more vital to our community.
Behind heart disease, cancer, and stroke, HAI’s are the 4th leading cause of death in the U.S.
Regardless of the dire necessity for instituting and practicing optimal methods of effective infection prevention, this field remains a specialized niche within the industry.
In mid-February, the Association for Professionals in Infection Control and Epidemiology (APIC) issued a proclamation to all healthcare organizations, urging them to conduct assessments of the capacity and capabilities of their IP programs. In cases everywhere, these assessments undoubtedly revealed and confirmed the many shortcomings throughout this essential industry.
Why is this the case? Well, one can suppose that while little kids want to grow up to be doctors, and college students study diligently to be nurses, relatively few of us are ‘dreaming to be’ Infection Preventionists when we grow up.
Well, perhaps it’s time that we start telling our children to start dreaming of becoming IP specialists, because though they may not be saving lives in such dramatic ways as comic book heroes, the number of lives that they are saving is beyond calculation.
The Infection Prevention profession is certainly experiencing across-the-board staffing issues, and attracting new personnel into the field remains a top challenge.
“Infection Prevention is not the first field that most new graduates entering the healthcare workforce are interested in pursuing as the job may not be appealing to these novice professionals,” indicated J. Hudson Garrett Jr., Ph.D., FNAP, FSHEA, FIDSA, Adjunct Assistant Professor of Medicine, Infectious Diseases, University of Louisville School of Medicine, states. “
“Healthcare facilities must create a powerful recruitment approach that entices new graduates and experienced healthcare professionals to enter the field of Infection Prevention. With the ongoing staffing challenges that are facing across healthcare generally, recruiting specialized Personnel such as Infection Preventionists will sadly only prove to be more and more challenging. Employees want to work for an employer that is invested in their future and success as a healthcare professional. Employers that demonstrate a culture of support and just culture are more likely to be successful in recruiting highly engaged and qualified Infection Preventionists. One innovative idea that would likely yield more Infection Preventionists would be for health systems to partner together to offer on-the-job training in the form of an Infection Prevention Fellowship.”
The strains, the pains
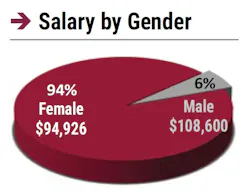
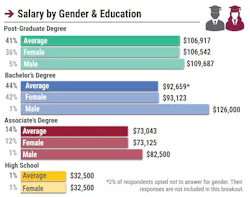
HPN’s latest survey found that the average salary of an IP professional comes in at approximately $95,000. Although this number is practically identical to survey findings last year, it is up almost $10,000 since the onset of COVID in 2019, and nearly $18,000 since 2016. Moreover, 69% of respondents reported that their annual base salary has increased in comparison to 2021, with the largest chunk (35%) indicating an increase between 2% and 3%.
Thus, it is clear that IP professionals are valued for their work, or, better said, overwork. COVID-19 has, beyond all doubt, transformed the entirety of the field. In terms of the ways in which COVID-19 has done this, close to 90% reported the ‘need to implement new infection prevention protocols;’ over 60% of those who responded saw increases in patient volume and decreases in both staff and personal protective equipment (PPE) as key elements pressurizing the job.
“Overworked, tired and burnt out [are] all of the things I would use to express my current state of mind,” McCready admitted. “Yes, we or at least I was asked to go above and beyond normal functioning. Simply the reporting involved with the pandemic was incredibly daunting and time consuming. There was not enough time in any day or week to complete all of the things that needed to be completed. And certainly, we didn’t have time to keep up with what our jobs actually were,” she added.
McCready’s thoughts seem to echo those of her Infection Prevention colleagues.
“Forty hours turned into 70 hours at the high end of the COVID-19 Pandemic,” noted Paulina Rodriguez, MSN, RN, Infection Preventionist at a major healthcare facility in the southwest. “We (started) teaching PPE to everyone in the facility. We had to submit spreadsheets every day.”
The statistics presented by HPN’s survey affirm that 88% of IP professionals saw their work hours increased by the demands of the COVID-19 pandemic, and 82% stated that their job responsibilities broadened in scope. These responses included persons who said things such as, “emotionally draining,” “burned out,” and “increased stress.”
Such feelings from those in the field is likely not doing much in the way of drawing new persons into the IP workforce. Rodriguez continued, “It is true. There are less people wanting to take over IP roles,” Rodriguez acknowledged. “These are daunting positions with lots of responsibility. When people look at the job responsibilities, it overwhelms them and they realize that it’s too much responsibility. I think that after what we have been through as IP’s with this COVID-19 Pandemic and are still going through presently.”
An overwhelming 72% responded that they have taken on additional roles and responsibilities outside of their expected job duties during the pandemic. In fact, several persons responded that, in essence, they have evolved into ‘all-encompassing educators for COVID.’
There seems to be some other glaring numbers regarding the IP industry, and they are particularly even more glaring by the suggested notion that the already seemingly small workforce may not be far removed from getting even smaller.
On top of the well-established fact that it is not easy to draw young healthcare professionals into the IP trade, those already employed encompass many who are seasoned with many years under their belt. Sixty-two percent were over 51 years of age, with the average age of all IP personnel coming in at 53. Only a meager 14% were under the age of 40, and only 4% 30 or younger.
The studies on the studies
Although, a more relevant question would be is there enough focus on Infection Prevention in academic programs today? One IP expert attributes the result to the availability of IP educational programs.
According to Garrett, “from an academic program, there are very few programs which produce Infection Preventionists thru a degree program, and even fewer new graduates from healthcare professions that are interested in entering this field initially. We must have a better mousetrap in terms of recruiting and developing highly capable Infection Preventionists in order to remain competitive in today’s challenging times.”
What Infection Preventionists are doing is immeasurably invaluable. They are saving hospitals and healthcare facilities from more than can ever be imagined. The lives being impacted, and the lives being saved (not to mention dollars) from avoiding infections lies at the very essence of healthcare, regardless of how tangible it is to measure.
“Most of the time what we do goes unseen and certainly ‘hurts the bottom line.’ IP is an expense to an organization without reimbursement that can be measured. Meaning, an infection prevented is hard to prove, and is even harder to place a dollar sign on. Hospital leaderships don’t always see the big picture,” says Jamie McCready.
In totality, Infection Prevention, though so desperately needed, seems to be underappreciated and undervalued. Couldn’t measures be taken to ensure we have more highly-skilled, passionate professionals who are dedicated this field?
So how might healthcare organizations rectify the disconnect?
According to Dr. Hudson Garrett, the healthcare field personnel is, collectively speaking, under great duress, and could benefit from the utilization of team-based tactics, such as the Agency for Healthcare Research and Quality’s TeamSTEPPS program:
“Healthcare as a whole is on the brink of burnout in many instances, and Infection Preventionists are no exception. As a healthcare sector, we must invest in our personnel and our teams thru the use of evidence-based approaches to improving resilience in frontline healthcare professionals and management personnel. This requires a concentrated effort by executive leadership, human resources, and healthcare personnel leaders across all of healthcare to reinvest in our teams and ensure that they know they are appreciated. Another powerful tool that can be deployed to assist with these challenges is the AHRQ TeamSTEPPS program which enables healthcare teams to create highly effective interprofessional communication. TeamSTEPPS is an excellent method to improve communication and ensure that tense situations can be de-escalated and managed appropriately.”
If anything, COVID-19 should be an event that triggers increased involvement in the IP professional, experts agree. Building stronger Infection Prevention programs within healthcare facilities will significantly curb and prevent infections from occurring.
As we have learned over past few years, fighting infection IS the most critical line of defense in modern healthcare.
About the Author
Scott Tomko
Managing Editor
Scott Tomko was previously Managing Editor for Healthcare Purchasing News.