The maturation of clinically integrated supply chain maturity models
In 2017, the Association for Healthcare Resource and Materials Management (AHRMM) launched its Clinically Integrated Supply Chain (CISC) Task Force, under the direction of Jimmy Chung, MD, who will become chair of the association in 2022. AHRMM defined CISC as “an interdisciplinary approach to deliver patient care with the highest value (high quality, best outcomes and minimal waste at the lowest cost of care) that is achieved through assimilation and coordination of clinical and supply chain knowledge, data and leadership toward care across the continuum that is safe, timely, evidenced-based, efficient, equitable and patient focused.”
Since then, several other organizations have offered their own definitions and/or maturity models that generally fall into two different areas of emphasis:
• Using clinical evidence to reduce unwarranted variation in how care is delivered (including products used), resulting in lower costs and better quality care
• Tracking inventory utilization to minimize medical errors and adverse events and generate real world evidence on what works best on which patient populations
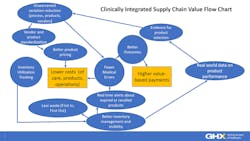
It is not about choosing one model over another, but rather understanding the full breadth of clinical-supply chain integration and how the various models are both complementary and mutually reinforcing, as depicted below.
Use of clinical evidence can help clinicians and supply chain collaborate to determine the best products that deliver the best care at the most optimal price. Armed with this data, hospitals and health systems can standardize on specific products and vendors, often resulting in better contract pricing. Less variation can also increase clinician familiarity with the product, often resulting in fewer errors in use.
On the other hand, by tracking inventory, clinicians can be alerted in real time if a product that is expired or recalled is about to be used on a patient. Better inventory visibility also supports practices that reduce waste by prioritizing the use of products that are closest to their expiration dates. Capturing data on which products are used on which patients not only supports better case costing, it can also help generate more real world evidence on how products perform in routine clinical practice, which can further support variation reduction efforts.
The use of inventory management tools and practices in the clinical environment is central to a couple of the maturity models. Developed prior to the pandemic, these models do not reference how better inventory utilization tracking can support demand planning, a topic that has garnered considerable attention in the wake of severe supply shortages (See the September 2020 issue of Standard Practices, https://hpnonline.com/21150785). While the magnitude of the pandemic may have still resulted in shortages, hospitals could have shared usage data with manufacturers to help them understand actual demand. Suppliers, in turn, could have provided hospitals with better visibility into when they can expect product shipments and in what quantity.
During the pandemic, hospitals were required to report their inventory levels, burn rates, and anticipated shipments. Many were previously not tracking this data, but now that they have developed these capabilities, it will be interesting to see if such practices become standard operating practice. Certainly, there is a business case for better inventory management, and that case only gets stronger as hospitals seek more clinical-supply chain integration. The key will be broadening our view as we recognize the interdependencies between the quality and cost of healthcare delivery and the day-to-day operations upon which healthcare delivery depends. Adding these aspects to the various maturity models in existence will support our collective ability to lower the costs of healthcare, while generating evidence on what delivery outcomes matter to patients relative to the costs to achieve those outcomes.
1. Clinically Integrated Supply Outcomes Model | HIMSS Analytics - North America
About the Author

Karen Conway
CEO, Value Works
Karen Conway, CEO, ValueWorks
Karen Conway applies her knowledge of supply chain operations and systems thinking to align data and processes to improve health outcomes and the performance of organizations upon which an effective healthcare system depends. After retiring in 2024 from GHX, where she served as Vice President of Healthcare Value, Conway established ValueWorks to advance the role of supply chain to achieve a value-based healthcare system that optimizes the cost and quality of care, while improving both equity and sustainability in care delivery. Conway is former national chair of AHRMM, the supply chain association for the American Hospital Association, and an honorary member of the Health Care Supplies Association in the UK.