Q
I worked at a different medical facility, and they provided ear protection. What does ANSI/AAMI ST79 say about this? Because where I am now, they do not provide any ear protection.
A
Your question is centered on ANSI/AAMI ST79 and what it states about noise exposure and protections for staff. In reviewing ST79, AAMI does not currently address this topic, but maybe in the future. So, let us look at what standards would address any staff members’ concern(s) about noise exposure?
As with anything concerning workers’ safety, each medical facility (and the department within that facility) should conduct a risk analysis of where all employees work. This is outlined in OSHA standards.
Under the regulation [29 CFR 1910.95(i)(1)], OSHA requires that employers shall make hearing protectors available to all employees exposed to an 8-hour time-weighted average (TWA) of 85 decibels or greater at no cost to the employees. Hearing protectors shall be replaced, as necessary.
A safe or acceptable noise level for constant exposure is 68 decibels (dB) or below. The decibel is a unit used to measure the intensity of a sound. Hearing damage can occur when exposed to a constant background noise of 80 to 90 dB.
You may have worn ear protection while working in the decontamination area. That makes sense, and I have seen ear protection increasingly used in departments from simple orange earplugs to full headphone ear protection provided to all staff members.
Think about this. You have noise being created constantly by:
• Instrument washers
• Cart washers
• Ultrasonic cleaners
• Case carts coming and going
• Water running.
My suggestion is to work with your risk management department and department management team to ask for noise levels to be measured in your department. This provides documentation and helps instate a policy and program to protect workers hearing safety.
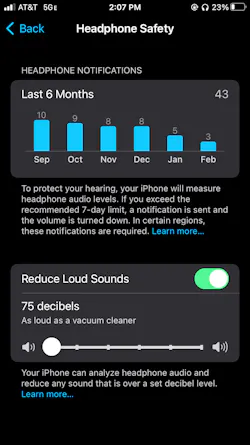
It is worthwhile to note Apple® iPhone® iOS 14 users have a new Settings option called “Headphone Safety” (Fig. 1). The “Reduce Loud Sounds” option empowers users with an extra means of hearing protection (required in certain regions), by setting a desired decibel-level to your headphones/audio buds. Mine is set at 75 decibels (as loud as a vacuum cleaner). If the user exceeds the set level over a seven-day limit, they will receive notification and the volume automatically reduced.
Q
Can you explain the difference between the push and the pull method for using a brush to clean medical devices?
A
Brushing a medical device is dependent upon the brush selected and the device to be cleaned.
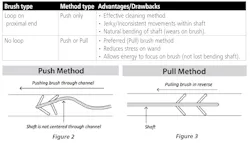
• Brush with a loop on its proximal—only use the push-type method.
• Brush without a loop—use either a push or a pull-type method.
The Push Method is the method most people use. This method is used when a brush has a loop on its end or the lumen is dead ended, thus you cannot use the pull method. While it is effective, it does have its drawbacks. Cleaning by pushing the fiber end of the brush through first creates a series of jerky and inconsistent movements within the shaft. This problem does not occur with the pull through method. Using the push cleaning method also creates a natural bending of the shaft (Fig. 2), which wears on the brush.
The Pull Method (traction) is my personal preference (when possible) for brushing a channel that has two-open ends. Insert the non-brush end into the less contaminated side of the channel. Once the shaft tip appears on the other side of the channel, pull it through. This allows for proper and continuous cleaning of the inner channel for medical and surgical instruments (Fig. 3). The physics of brushing with this method reduces the stress on the shaft allowing energy to focus more on the brush and not be lost in the bending of a shaft, which can happen with the push method.
Remember, when possible, with either method, try to twist or turn the shaft as you go into the lumen. This additional friction is important when cleaning any medical device.
Reference:- AAMI. (2017). ANSI/AAMI ST79:2017 Comprehensive guide to steam sterilization and sterility assurance in health care facilities. Association for the Advancement of Medical Instrumentation (AAMI).
- Occupational Safety & Health Administration (OSHA). (2011, February 10). 29 CFR Part 1910, Subpart I, Enforcement Guidance for Personal Protective Equipment in General Industry. United States Department of Labor. https://www.osha.gov/enforcement/directives/cpl-02-01-050.
- Occupational Safety & Health Administration (OSHA). (2006, April 20). 1910.95(a)- Occupational noise exposure. United States Department of Labor. https://www.osha.gov/laws-regs/regulations/standardnumber/1910/1910.95.
- Occupational Safety & Health Administration (OSHA). [n.d.]. Occupational Noise Exposure. United States Department of Labor. https://www.osha.gov/noise.
- Occupational Safety & Health Administration (OSHA). (1996, March 26). 1910.95, Requirements of the Occupational Noise Exposure Standard with regards to hearing protectors. United States Department of Labor. https://www.osha.gov/laws-regs/standardinterpretations/1996-03-26-1.
- Paavola, A. (2018, January 4). The art of brushing – how to properly clean medical equipment to ensure patient safety. Becker’s Clinical Leadership & Infection Control. Accessed 2022, January 13. https://www.beckershospitalreview.com/quality/the-art-of-brushing-how-to-properly-clean-medical-equipment-to-ensure-patient-safety.html.
- The Texas Department of Insurance (TDI), Safety@Work Division of Workers’ Compensation (DWC). [n.d.]. HS04-050C (10-20) Noise and Hearing Protection Fact Sheet. https://www.tdi.texas.gov/pubs/videoresource/fsnoise.pdf.
Stephen M Kovach, BS, CFER, started in the medical field in 1975 as a sterilization orderly and has worked in many positions within the Healthcare Industry. He presently is Clinical Educator Emeritus at Healthmark Industries.
About the Author

Stephen M. Kovach
Stephen M Kovach, BS, CFER, started in the medical field in 1975 as a sterilization orderly and has worked in many positions within the Healthcare Industry. He presently is Clinical Educator Emeritus at Healthmark, A Getinge company.